Journal Description
Pharmacy
Pharmacy
is an international, scientific, peer-reviewed, open access journal dealing with pharmacy education and practice and is published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 19.5 days after submission; acceptance to publication is undertaken in 3.4 days (median values for papers published in this journal in the first half of 2023).
- Recognition of Reviewers: Reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.2 (2022);
5-Year Impact Factor:
2.3 (2022)
Latest Articles
Evaluating the Quality of the Core Entrustable Professional Activities for New Pharmacy Graduates
Pharmacy 2023, 11(4), 126; https://doi.org/10.3390/pharmacy11040126 - 08 Aug 2023
Abstract
This study aimed to evaluate the quality of the American Association of Colleges of Pharmacy Core Entrustable Professional Activities (Core EPAs) for New Pharmacy Graduates according to standards outlined in competency-based education literature utilizing the Queen’s EPA Quality (EQual) rubric. A cohort of
[...] Read more.
This study aimed to evaluate the quality of the American Association of Colleges of Pharmacy Core Entrustable Professional Activities (Core EPAs) for New Pharmacy Graduates according to standards outlined in competency-based education literature utilizing the Queen’s EPA Quality (EQual) rubric. A cohort of pharmacists with EPA expertise rated Core EPA quality with the EQual rubric and provided recommendations for revisions. A generalizability study determined the reliability of the EQual ratings with pharmacist users. Nine pharmacists responded (4.4%). Most EPAs (9/15) did not reach the overall cut-off score, indicating low quality. EPAs 1 through 5 and EPA 14 (fulfill a medication order) were deemed high quality. EPA 12 (use evidence-based information to advance patient care) scored the lowest at 3.47 (SEM 0.29). EPA 14 scored the highest at 4.60 (SEM 0.14). EPA 15 (create a written plan for continuous professional development) was the only EPA to fail to reach the cut-off across all EQual domains. EPAs in the Patient Care Provider Domain received significantly higher ratings than other EPAs. On average, three respondents recommended revision for each. Most comments aligned with the EPA’s EQual rubric performance. The generalizability study analysis revealed excellent reliability (G = 0.80). Determining EPA quality utilizing objective measurement tools should drive EPA development and revisions to more accurately reflect the roles, responsibilities, and expectations of pharmacists on the healthcare team.
Full article
(This article belongs to the Section Pharmacy Education and Student/Practitioner Training)
Open AccessArticle
The Value of Pharmacogenomics for White and Indigenous Americans after Kidney Transplantation
by
, , , , , , , and
Pharmacy 2023, 11(4), 125; https://doi.org/10.3390/pharmacy11040125 - 08 Aug 2023
Abstract
Background: There is a paucity of evidence to inform the value of pharmacogenomic (PGx) results in patients after kidney transplant and how these results differ between Indigenous Americans and Whites. This study aims to identify the frequency of recommended medication changes based on
[...] Read more.
Background: There is a paucity of evidence to inform the value of pharmacogenomic (PGx) results in patients after kidney transplant and how these results differ between Indigenous Americans and Whites. This study aims to identify the frequency of recommended medication changes based on PGx results and compare the pharmacogenomic (PGx) results and patients’ perceptions of the findings between a cohort of Indigenous American and White kidney transplant recipients. Methods: Thirty-one Indigenous Americans and fifty White kidney transplant recipients were studied prospectively. Genetic variants were identified using the OneOme RightMed PGx test of 27 genes. PGx pharmacist generated a report of the genetic variation and recommended changes. Pre- and post-qualitative patient surveys were obtained. Results: White and Indigenous American subjects had a similar mean number of medications at the time of PGx testing (mean 13 (SD 4.5)). In the entire cohort, 53% received beta blockers, 30% received antidepressants, 16% anticoagulation, 47% pain medication, and 25% statin therapy. Drug–gene interactions that warranted a clinical action were present in 21.5% of patients. In 12.7%, monitoring was recommended. Compared to the Whites, the Indigenous American patients had more normal CYP2C19 (p = 0.012) and CYP2D6 (p = 0.012) activities. The Indigenous American patients had more normal CYP4F2 (p = 0.004) and lower VKORC (p = 0.041) activities, phenotypes for warfarin drug dosing, and efficacy compared to the Whites. SLC6A4, which affects antidepressant metabolism, showed statistical differences between the two cohorts (p = 0.017); specifically, SLC6A4 had reduced expression in 45% of the Indigenous American patients compared to 20% of the White patients. There was no significant difference in patient perception before and after PGx. Conclusions: Kidney transplant recipients had several drug–gene interactions that were clinically actionable; over one-third of patients were likely to benefit from changes in medications or drug doses based on the PGx results. The Indigenous American patients differed in the expression of drug-metabolizing enzymes and drug transporters from the White patients.
Full article
(This article belongs to the Special Issue Pharmacists’ Role in the Management of Kidney Disease)
►▼
Show Figures
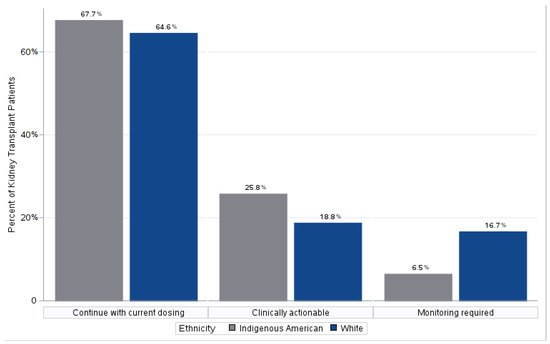
Figure 1
Open AccessArticle
What Are the Drug-Related Problems Still Faced by Patients in Daily Life?—A Qualitative Analysis at the Pharmacy Counter
by
, , , , , and
Pharmacy 2023, 11(4), 124; https://doi.org/10.3390/pharmacy11040124 - 03 Aug 2023
Abstract
Background: Drug-related problems (DRPs) affect many patients. Many activities in general practice, hospitals, and community pharmacies have been initiated to tackle DRPs. However, recent studies exploring what DRP patients are still facing in their daily lives are scarce. Methods: Danish pharmacy staff registered
[...] Read more.
Background: Drug-related problems (DRPs) affect many patients. Many activities in general practice, hospitals, and community pharmacies have been initiated to tackle DRPs. However, recent studies exploring what DRP patients are still facing in their daily lives are scarce. Methods: Danish pharmacy staff registered DRPs in prescription encounters to understand what DRPs patients are still experiencing in daily life. They noted short descriptions of what happened in the encounter that qualified the incident as a DRP. The descriptions were subjected to an inductive content analysis. Results: A wide range of DRPs that impacted patients’ daily lives practically and healthwise were identified. In total, eighteen percent of patients with prescriptions had a DRP. Three overall stages of DRPs were identified: challenges in receiving the medications, not knowing how or why to take the medications, and not experiencing satisfactory effects. Patients were emotionally affected by these problems. Conclusions: DRPs are still widespread in patients’ daily lives and influence their well-being. The identified DRPs illustrated the complexity of obtaining medications to work as intended and demonstrate that health professionals must take even the basics of medication intake much more seriously.
Full article
(This article belongs to the Section Pharmacy Practice and Practice-Based Research)
Open AccessArticle
Lessons Learned from a Shared Curriculum on Tobacco Cessation Using a Mixed-Methods Approach
by
, , , and
Pharmacy 2023, 11(4), 123; https://doi.org/10.3390/pharmacy11040123 - 02 Aug 2023
Abstract
Although the sharing of curricular content between health professional schools can reduce faculty burden, the literature provides little guidance to support these efforts. The objective of this investigation was to synthesize data from two prior studies to delineate recommendations guiding the future development
[...] Read more.
Although the sharing of curricular content between health professional schools can reduce faculty burden, the literature provides little guidance to support these efforts. The objective of this investigation was to synthesize data from two prior studies to delineate recommendations guiding the future development of shared curricula in health professional education. Applying Rogers’ Diffusion of Innovations Theory as a guiding framework, relevant data were extracted from a two-phase mixed-methods study evaluating the long-term impact of the shared Rx for Change: Clinician-Assisted Tobacco Cessation program. Phase 1, a qualitative study, involved telephone interviews with faculty participants of train-the-trainer workshops conducted between 2003 and 2005. These results informed the development of a phase 2 national survey, administered electronically as a long-term follow-up (13 to 15 years later) with train-the-trainer workshop participants. Results from the two studies were synthesized and summarized, producing seven key recommendations to guide development of shared curricula: (1) appeal to attendees, (2) relate content to clinical practice, (3) deliver live, in-person training, (4) develop high-quality materials, delivered by experts, (5) provide support, (6) meet accreditation standards, and (7) demonstrate effectiveness. Future program developers should consider these recommendations to enhance dissemination, adoption, and long-term sustainability of shared curricular content.
Full article
(This article belongs to the Special Issue Pharmacy: State-of-the-Art and Perspectives in USA)
Open AccessArticle
Exploring the Impact of an Innovative Peer Role-Play Simulation to Cultivate Student Pharmacists’ Motivational Interviewing Skills
by
and
Pharmacy 2023, 11(4), 122; https://doi.org/10.3390/pharmacy11040122 - 29 Jul 2023
Abstract
Effective patient-centered communication is a foundational skill for student pharmacists, with recent decades broadening the scope of professional responsibilities to include an increased emphasis on empathic communication and motivational interviewing (MI) as tools to support patients’ therapeutic adherence. Role-play is a potentially effective
[...] Read more.
Effective patient-centered communication is a foundational skill for student pharmacists, with recent decades broadening the scope of professional responsibilities to include an increased emphasis on empathic communication and motivational interviewing (MI) as tools to support patients’ therapeutic adherence. Role-play is a potentially effective pedagogical approach to cultivate these skills, although previous research has identified common shortcomings that can hinder its educational value, particularly in peer role-play with relatively inexperienced learners. The purpose of this study is to describe and provide initial assessment data for an innovative approach to peer role-play that incorporates pedagogical principles to address these common shortcomings. Using a mixed-methods study design that includes instructor-graded rubrics and inductive thematic analysis of student reflections, our findings indicate that students successfully demonstrated a range of important competencies through this experience and perceived it to be both challenging and highly beneficial for their personal and professional development. Among the MI principles and techniques practiced, students performed especially well on expressing empathy and frequently reflected on its importance for future patient care and clinical collaborations. Our findings also suggest that peer engagement through team activities and partnered role-play provides a felicitous context to explore empathic communication together.
Full article
(This article belongs to the Section Pharmacy Education and Student/Practitioner Training)
►▼
Show Figures
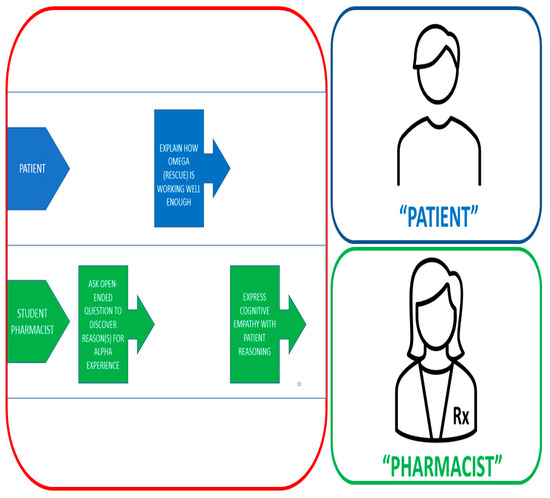
Figure 1
Open AccessProject Report
Community Pharmacy Recruitment for Practice-Based Research: Challenges and Lessons Learned
by
, , , , , and
Pharmacy 2023, 11(4), 121; https://doi.org/10.3390/pharmacy11040121 - 22 Jul 2023
Abstract
To support the successful integration of community pharmacies into value-based care models, research on the feasibility and effectiveness of novel pharmacist-provided patient care services is needed. The UNC Eshelman School of Pharmacy, supported by the National Association of Chain Drug Stores (NACDS) Foundation,
[...] Read more.
To support the successful integration of community pharmacies into value-based care models, research on the feasibility and effectiveness of novel pharmacist-provided patient care services is needed. The UNC Eshelman School of Pharmacy, supported by the National Association of Chain Drug Stores (NACDS) Foundation, designed the Community-based Valued-driven Care Initiative (CVCI) to (1) identify effective value-based patient care interventions that could be provided by community pharmacists, (2) implement and evaluate the feasibility of the selected patient care interventions, and (3) develop resources and create collaborative sustainability opportunities. The purpose of this manuscript is to describe recruitment strategies for CVCI and share lessons learned. The project team identified pharmacies for recruitment through a mixed data analysis followed by a “fit” evaluation. A total of 42 pharmacy organizations were identified for recruitment, 24 were successfully contacted, and 9 signed on to the project. During recruitment, pharmacies cited concerns regarding the financial sustainability of implementing and delivering the patient care services, challenges with staffing and infrastructure, and pharmacists’ comfort level. To foster participation, it was vital to have leadership buy-in, clear benefits from implementation, and assured sustainability beyond the research period.
Full article
(This article belongs to the Special Issue Community-Based Pharmacy Practice Quality Improvement and Research)
Open AccessBrief Report
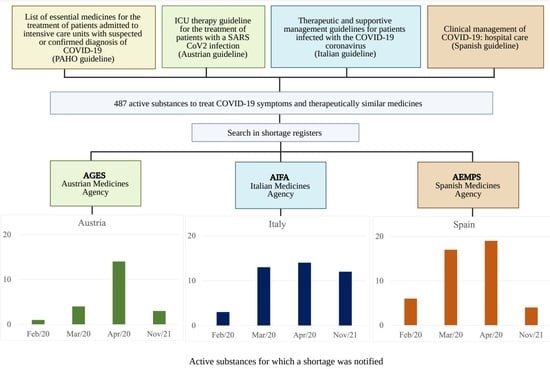
Shortages of Medicines to Treat COVID-19 Symptoms during the First Wave and Fourth Wave: Analysis of Notifications Reported to Registers in Austria, Italy, and Spain
Pharmacy 2023, 11(4), 120; https://doi.org/10.3390/pharmacy11040120 - 21 Jul 2023
Abstract
►▼
Show Figures
The study aimed to investigate medicine shortages of critical relevance in the pandemic. A total of 487 active substances for the treatment of COVID-19-related symptoms and therapeutically similar medicines were reviewed as to whether or not a shortage had been notified in Austria,
[...] Read more.
The study aimed to investigate medicine shortages of critical relevance in the pandemic. A total of 487 active substances for the treatment of COVID-19-related symptoms and therapeutically similar medicines were reviewed as to whether or not a shortage had been notified in Austria, Italy, and Spain for February 2020, March 2020, April 2020 (first wave of the pandemic), and, in comparison, in November 2021 (fourth wave). Publicly accessible shortage registers managed by the national regulatory authorities were consulted. For 48 active substances, a shortage was notified for at least one of the study months, mostly March and April 2020. Out of these 48 active substances, 30 had been explicitly recommended as COVID-19 therapy options. A total of 71% of the active substances with notified shortage concerned medicines labeled as essential by the World Health Organization. During the first wave, Spain and Italy had higher numbers of shortage notifications for the product sample, in terms of active substances as well as medicine presentations, than Austria. In November 2021, the number of shortage notifications for the studied substances reached lower levels in Austria and Spain. The study showed an increase in shortage notifications for COVID-19-relevant medicines in the first months of the pandemic.
Full article
Graphical abstract
Open AccessArticle
Pharmacists’ Perceptions on Safety Alerts of the Drug Utilization Review (DUR) in Electronic Health Records in a Tertiary Healthcare Hospital
by
and
Pharmacy 2023, 11(4), 119; https://doi.org/10.3390/pharmacy11040119 - 20 Jul 2023
Abstract
►▼
Show Figures
Electronic Drug Alarms and Drug Utilization Reviews (DURs) are crucial in improving patient safety by reducing the dispensing of contraindicated medications and minimizing adverse drug events. The DUR system often generates low-level alerts, making it challenging for pharmacists and doctors to discern more
[...] Read more.
Electronic Drug Alarms and Drug Utilization Reviews (DURs) are crucial in improving patient safety by reducing the dispensing of contraindicated medications and minimizing adverse drug events. The DUR system often generates low-level alerts, making it challenging for pharmacists and doctors to discern more critical alerts. This can result in alert fatigue, causing burnout and jeopardizing patient safety. A cross-sectional study was conducted in a tertiary hospital to explore pharmacists’ perspectives and experience with the DUR system. This study aimed to identify their responses to alerts indicating a need to change the original prescription and the difficulties encountered. Out of all the participants, 85% had prior experience with DUR alerts. However, 40% of them expressed dissatisfaction with the alerts. Moreover, 88% of the participants received highly frequent DUR alerts, but only 40% believed that DUR alerts could identify rare adverse drug reactions. Additionally, only 27% of the participants altered their prescriptions based on alerts for the MAOI/serotonin modulator. The survey showed that 66% of participants believe improvements are necessary for the DUR system. Specifically, 77% of participants felt that more information is needed on overlapping prescriptions, 82% on patients with chronic diseases, and 82% on potential reactions caused by co-administration. At the same time, 75% raised concern about the need for backup for any server breakdown. Positive perceptions about DUR lead to changing the prescription in response to an alert. Therefore, improving the DUR system is crucial to prevent pharmacists from missing important alerts and to increase their awareness of clinically significant alarm signals. By doing so, we can optimize patient safety and contribute to providing high-quality healthcare services.
Full article
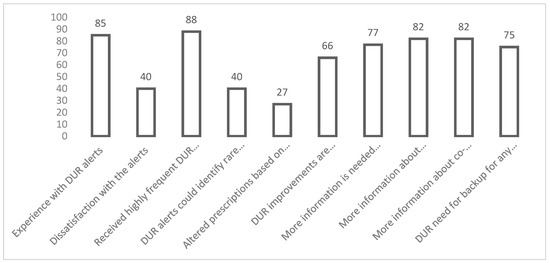
Figure 1
Open AccessCommunication
A Look into Pharmacy Practices among the Purépecha Indigenous Community
by
and
Pharmacy 2023, 11(4), 118; https://doi.org/10.3390/pharmacy11040118 - 19 Jul 2023
Abstract
This report describes the adoption and integration of Western medicine in Cherán K’eri after the social changes in the 1940s which led to the transition from healer to pharmacist. There are various health models that rely heavily on community pharmacies. The place used
[...] Read more.
This report describes the adoption and integration of Western medicine in Cherán K’eri after the social changes in the 1940s which led to the transition from healer to pharmacist. There are various health models that rely heavily on community pharmacies. The place used as the basis for this report was a clinic managed by a Purépecha-speaking physician and pharmacist that served primarily monolingual indigenous Purépecha patients, whose population was around 9550 according to the 2010 census. Twelve major differences were observed between community pharmacies in the United States and the community pharmacies of Cherán. It was also observed that the modern approach to the health of the indigenous population used a combination of Western medicine together with traditional methods and only resorted to short-term therapies with Western medicines lasting five days or less. A formulary from the clinic’s community pharmacy compiled in 2022 listed the 38 most common medications. Medications used included anti-infectives (n = 3), central nervous system (n = 2), endocrine/hormonal (n = 3), gastrointestinal (n = 3), musculoskeletal (n = 17), respiratory or allergy (n = 6), and genitourinary (n = 2).
Full article
(This article belongs to the Special Issue Delivery of Pharmaceutical Care—Leaving No One Behind)
Open AccessReview
Effectiveness and Safety of Glucosamine in Osteoarthritis: A Systematic Review
by
, , , , , , and
Pharmacy 2023, 11(4), 117; https://doi.org/10.3390/pharmacy11040117 - 14 Jul 2023
Abstract
Knee osteoarthritis is the most popular type of osteoarthritis that causes extreme pain in the elderly. Currently, there is no cure for osteoarthritis. To lessen clinical symptoms, glucosamine was suggested. The primary goal of our systematic review study is to evaluate the effectiveness
[...] Read more.
Knee osteoarthritis is the most popular type of osteoarthritis that causes extreme pain in the elderly. Currently, there is no cure for osteoarthritis. To lessen clinical symptoms, glucosamine was suggested. The primary goal of our systematic review study is to evaluate the effectiveness and safety of glucosamine based on recent studies. Electronic databases such as PubMed, Scopus, and Cochrane were used to assess the randomized controlled trial (RCT). From the beginning through March 2023, the papers were checked, and if they fulfilled the inclusion criteria, they were then examined. The Western Ontario and McMaster Universities Osteoarthritis (WOMAC) and Visual Analog Scale (VAS) scales were considered the main outcome measures. A total of 15 studies were selected. Global pain was significantly decreased in comparison to placebo, as measured by the VAS index, with an overall effect size of standardized mean difference (SMD) of −7.41 ([95% CI] 14.31, 0.51). The WOMAC scale confirmed that pain, stiffness, and physical function had improved, however the effects were insufficient. A statistical update also revealed that there were no reports of serious medication interactions or significant adverse events. To summarize, glucosamine is more effective than a placebo at reducing pain in knee osteoarthritis patients. In long-term treatment, oral glucosamine sulfate 1500 mg/day is believed to be well tolerated.
Full article
(This article belongs to the Special Issue Medication Use and Patient Safety in Clinical Pharmacy)
►▼
Show Figures
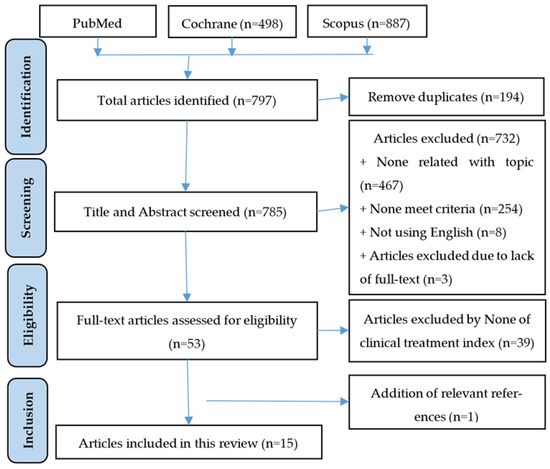
Figure 1
Open AccessArticle
Student Perspectives on the Pharmacist’s Role in Deprescribing Opioids: A Qualitative Study
by
, , , , and
Pharmacy 2023, 11(4), 116; https://doi.org/10.3390/pharmacy11040116 - 13 Jul 2023
Abstract
Introduction: Opioid over-prescribing has led to changes in prescribing habits and a reduction in the amount of opioid prescriptions per patient. Deprescribing has proved to be an effective way of decreasing the number of opioids patients are receiving, and pharmacists are in the
[...] Read more.
Introduction: Opioid over-prescribing has led to changes in prescribing habits and a reduction in the amount of opioid prescriptions per patient. Deprescribing has proved to be an effective way of decreasing the number of opioids patients are receiving, and pharmacists are in the optimal position to provide these services for their patients. However, student pharmacists require additional education and training to be able to understand their role in deprescribing opioids upon entering the profession. Methods: Student pharmacists at three United States of America schools of pharmacy were invited to participate in virtual focus groups about deprescribing opioids in Fall 2021. A trained qualitative researcher conducted the focus groups, which were audio-recorded and later transcribed verbatim for thematic analysis. Two independent qualitative researchers coded the transcripts using both inductive and deductive approaches. The researchers then met to identify, discuss, and describe themes from the data. Results: Thematic analysis revealed two themes: (1) perceived obstacles and enablers to initiate deprescribing for opioid medications and (2) additional pharmacy curricula experiences are necessary to better equip student pharmacists to address deprescribing. These themes emphasize the challenges student pharmacists face as well as opportunities to enhance their knowledge to be practice-ready. Conclusion: Varying educational approaches to teaching deprescribing in the pharmacy curriculum, including objective structured clinical exams, interprofessional education, and motivational interviewing, should be further assessed.
Full article
(This article belongs to the Section Pharmacy Education and Student/Practitioner Training)
►▼
Show Figures
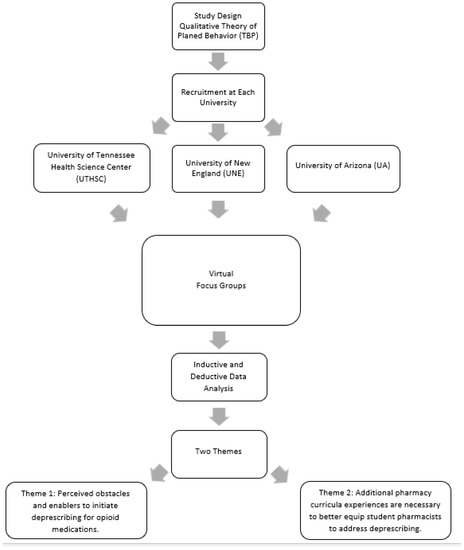
Figure 1
Open AccessArticle
Uncovering the Burden of Rhinitis in Patients Purchasing Nonprescription Short-Acting β-Agonist (SABA) in the Community
by
, , , , , and
Pharmacy 2023, 11(4), 115; https://doi.org/10.3390/pharmacy11040115 - 10 Jul 2023
Abstract
Asthma and rhinitis are common comorbidities that amplify the burden of each disease. They are both characterized by poor symptom control, low adherence to clinical management guidelines, and high levels of patient self-management. Therefore, this study aims to investigate the prevalence of self-reported
[...] Read more.
Asthma and rhinitis are common comorbidities that amplify the burden of each disease. They are both characterized by poor symptom control, low adherence to clinical management guidelines, and high levels of patient self-management. Therefore, this study aims to investigate the prevalence of self-reported rhinitis symptoms in people with asthma purchasing Short-Acting Beta Agonist (SABA) reliever medication from a community pharmacy and compare the medication-related behavioral characteristics among those who self-report rhinitis symptoms and those who do not. Data were analyzed from 333 people with asthma who visited one of eighteen community pharmacies in New South Wales from 2017–2018 to purchase SABA and completed a self-administered questionnaire. Participants who reported rhinitis symptoms (71%), compared to those who did not, were significantly more likely to have coexisting gastroesophageal reflux disease (GERD), overuse SABA, and experience side effects. They may have been prescribed daily preventer medication but forget to take it, and worry about its side effects. They were also more likely to experience moderate-to-severe rhinitis (74.0%), inaccurately perceive their asthma as well-controlled (50.0% self-determined vs. 14.8% clinical-guideline defined), and unlikely to use rhinitis medications (26.2%) or daily preventer medication (26.7%). These findings enhance our understanding of this cohort and allow us to identify interventions to improve patient outcomes.
Full article
(This article belongs to the Special Issue Community-Based Pharmacy Practice Quality Improvement and Research)
►▼
Show Figures
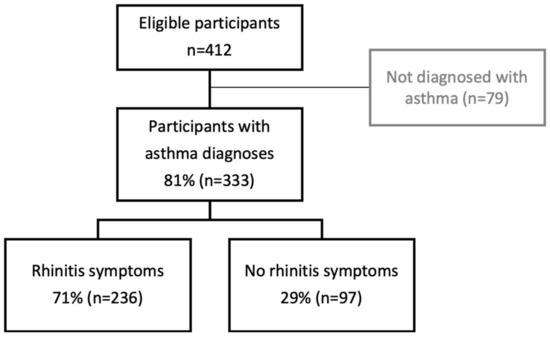
Figure 1
Open AccessArticle
A Pilot Study to Establish the Leadership Development Needs of Community Pharmacist Leads in Lambeth, South East London
Pharmacy 2023, 11(4), 114; https://doi.org/10.3390/pharmacy11040114 - 06 Jul 2023
Abstract
Primary care networks (PCNs) are geographical networks consisting of 30,000 to 50,000 patients and groups of general practices working in a multidisciplinary team, including community pharmacists. Community pharmacy (CP) neighbourhood leads act as a conduit between pharmacy contractors and general practitioners (GPs) in
[...] Read more.
Primary care networks (PCNs) are geographical networks consisting of 30,000 to 50,000 patients and groups of general practices working in a multidisciplinary team, including community pharmacists. Community pharmacy (CP) neighbourhood leads act as a conduit between pharmacy contractors and general practitioners (GPs) in these networks, sharing information and providing a voice for the community pharmacy locally. The Lambeth medicines team (NHS South East London Integrated Care Board) recognised the need to continue funding these leadership roles to address barriers to relationship-building between community pharmacies and general practices, the consistency of service delivery and effective communication. The aim of this study was to understand the current experience of CP neighbourhood leads to inform their further development. All eight CP neighbourhood leads individually completed a semi-structured interview over Microsoft Teams, which was then reviewed using content analysis. Ethical approval was received. Leads reported the use of common communication methods such as emails, text messaging applications and telephone calls to engage GPs and pharmacies in their neighbourhoods. Barriers to undertaking their roles included time constraints, delays in responses, high workloads and competing pressures. Other factors impacting their effectiveness and ability to undertake their roles included the scheduling of meetings outside of working hours, finding time during busy working days and organising locum cover on an ad hoc basis. The leads also reported they spent more time focussed on building relationships with their peers and less time focussed on general practice colleagues. Support for CP neighbourhood leads could include ensuring that funded time is protected; communication and technology training; and the provision of more structural support for communication with GPs. The findings of this study can be used to inform future work.
Full article
(This article belongs to the Special Issue Pharmacy: State-of-the-Art and Perspectives in UK)
►▼
Show Figures
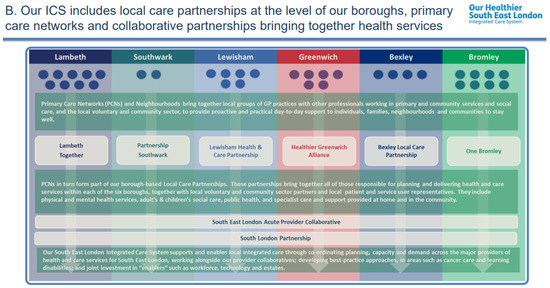
Figure 1
Open AccessBrief Report
Evaluation of Peak Inspiratory Flow Rate in Hospitalized Palliative Care Patients with COPD
Pharmacy 2023, 11(4), 113; https://doi.org/10.3390/pharmacy11040113 - 06 Jul 2023
Abstract
Dry powder inhalers are an effective yet costly COPD medication-delivery device. Patients must possess a minimum peak inspiratory flow rate (PIFR) for inhaled medication to be properly deposited into the lungs. Hospitalized palliative-care patients with diminished lung function due to advanced COPD may
[...] Read more.
Dry powder inhalers are an effective yet costly COPD medication-delivery device. Patients must possess a minimum peak inspiratory flow rate (PIFR) for inhaled medication to be properly deposited into the lungs. Hospitalized palliative-care patients with diminished lung function due to advanced COPD may not possess the minimum PIFR (30 L/min) for adequate drug delivery. This study aims to quantify PIFR values for hospitalized palliative-care patients with advanced COPD to evaluate whether these patients meet the minimum PIFR requirements. Hospitalized patients ≥18 years old with a palliative-care consultation were eligible if they had a diagnosis of advanced COPD (GOLD C or D). Patients were excluded if they lacked decision-making capacity or had a positive COVID-19 test within the previous 90 days. Three PIFR values were recorded utilizing the In-CheckTM device, with the highest of the three PIFR attempts being utilized for statistical analysis. Eighteen patients were enrolled, and the mean of the highest PIFR readings was 72.5 L/min (±29 L/min). Post hoc analysis indicated 99.9% power when comparing the average best PIFR to the minimum PIFR (30 L/min) but only 51.4% power when compared to the optimal PIFR (60 L/min). This study found that palliative-care patients possess the minimum PIFR for DPI drug delivery.
Full article
(This article belongs to the Special Issue Medicine Use and Management in Palliative Care)
►▼
Show Figures
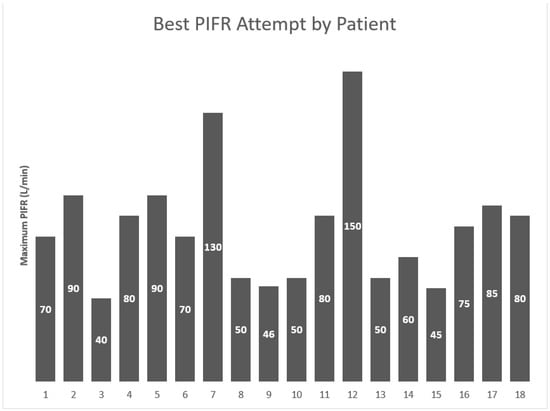
Figure 1
Open AccessArticle
Student Perceptions of Substance Use Disorder Stigma as a Factor for Health Disparities: A Mixed-Methods Study
by
, , , , and
Pharmacy 2023, 11(4), 112; https://doi.org/10.3390/pharmacy11040112 - 01 Jul 2023
Abstract
Background: The prevalence of substance use disorders (SUDs) is an alarming problem in the United States; however, only a fraction of patients receive treatment. Stigma from both healthcare professionals and society at large negatively impacts SUD treatment. There are limited data regarding the
[...] Read more.
Background: The prevalence of substance use disorders (SUDs) is an alarming problem in the United States; however, only a fraction of patients receive treatment. Stigma from both healthcare professionals and society at large negatively impacts SUD treatment. There are limited data regarding the perceptions of healthcare students on SUD stigma as a health disparity. Methods: We conducted a concurrent mixed-methods study among students enrolled in six health-related colleges at one mid-south health science center in the US over 3 months. Both an electronic survey consisting of 17 close-ended questions and researcher-led focus groups were conducted to understand their perceptions of stigma and SUDs. The research team followed the six steps recommended by Braun and Clarke regarding the data that aimed to capture associations between categories and extract and conceptualize the themes, and thematic analysis was done using Dedoose® (Manhattan Beach, CA, USA) qualitative software, which facilitated all the codes being kept organized and compared the frequency of codes across categories. Results: A total of n = 428 students participated in the survey (response rate = 13%), and n = 31 students took part in five focus groups. Most student respondents, on average, either agreed or strongly agreed that: stigma currently exists in the healthcare field; stigma can lead to patients’ not receiving the appropriate care for an SUD; and stigma can lead to lower quality care provided to patients with SUDs. Two themes were identified based on the thematic analysis: (1) additional training is necessary to better equip students for addressing SUDs in practice and (2) suggestions were formed to develop synergy between didactic and clinical rotations to improve SUD training. Conclusions: It is evident that students perceive the stigma surrounding SUDs as a detriment to patient care. Opportunities may exist in professional training programs to more seamlessly and intentionally weave SUD treatment and management concepts throughout the curriculum, as well as to empower students to operate in the complex regulatory scheme that exists for SUDs in the US.
Full article
Open AccessArticle
Navigating Access and Optimizing Medication Infusions in an Academic Medical Center: A Quality Improvement Study
by
and
Pharmacy 2023, 11(4), 111; https://doi.org/10.3390/pharmacy11040111 - 30 Jun 2023
Abstract
►▼
Show Figures
(1) Background: The rising prices of medical infusions have resulted in the increased utilization of policies for payors to manage costs. These policies can be disruptive to the continuity of care, and health systems should develop a systematic strategy to address market changes
[...] Read more.
(1) Background: The rising prices of medical infusions have resulted in the increased utilization of policies for payors to manage costs. These policies can be disruptive to the continuity of care, and health systems should develop a systematic strategy to address market changes and prevent patient leakage. (2) Methods: A quality improvement study was conducted by an interdisciplinary workstream to assess the current state of infusion services in an academic medical center in the Midwest and to provide recommendations for immediate access improvement and long-term system planning. An organizational assessment of the value stream was completed, which analyzed the available infusion capacity, billing strategy, patient mix/volumes, payor mix, staffing levels, and current policies. The interventions implemented after developing the infusion system strategy were triaging patients to the appropriate site of care to increase infusion capacity and eliminating paper orders in one of the health system’s Infusion Centers. (3) Results: Patients receiving medical infusions for oncologic conditions warrant unique considerations in evaluating the Infusion Center’s efficiency due to the infusion regimen’s length, complexity, and tolerability. The management of the payor site of care also poses a challenge for health systems to triage patients effectively without fragmenting care. (4) Conclusions: An organizational strategy around infusion services must include broad stakeholder representation to address the clinical, operational, and financial challenges to provide timely care to patients.
Full article
Figure 1
Open AccessBrief Report
Telehealth Integration into Pharmacy Practice Curricula: An Exploratory Survey of Faculty Perception
by
and
Pharmacy 2023, 11(4), 110; https://doi.org/10.3390/pharmacy11040110 - 30 Jun 2023
Abstract
(1) Background: The use of telehealth in the United States during the coronavirus disease 2019 pandemic was accelerated and there was a lack of telehealth training programs available to clinicians of all levels. At the onset of the pandemic, the American Association of
[...] Read more.
(1) Background: The use of telehealth in the United States during the coronavirus disease 2019 pandemic was accelerated and there was a lack of telehealth training programs available to clinicians of all levels. At the onset of the pandemic, the American Association of Colleges of Pharmacy (AACP) had no educational outcomes or professional activity standards for the inclusion of telehealth in the didactic Doctor of Pharmacy curriculum. Yet, in November 2022, the AACP encouraged colleges of pharmacy to include digital health and telehealth. The purpose of this study was to assess faculty perceptions in preparation for a nation-wide survey regarding telehealth integration into pharmacy practice curricula. (2) Methods: An exploratory questionnaire was developed to describe faculty perceptions and opinions of telehealth integration into the pharmacy practice curriculum at a single college of pharmacy. The questionnaire was emailed to 76 faculty members over six weeks in Summer 2022. Data were summarized descriptively. (3) Results: A total of 18 faculty members completed the survey (24% response rate). The responding faculty were typically very aware (median = 4) of telehealth, its benefits, and barriers, and were very comfortable (median = 4) discussing telehealth communication, benefits of telehealth, and barriers of telehealth. Yet, they were less comfortable discussing telehealth applications (median = 2.5). The faculty had a positive perception of telehealth in general (mean = 8.1 ± 1.5), telehealth services (mean = 8.6 ± 1.6), and the incorporation of telehealth instruction into the pharmacy practice curriculum (mean = 7.7 ± 2.7). Most respondents (67%) could discuss telehealth in their course. Lack of time to teach (50%) was the most reported reason by those who did not have plans to incorporate telehealth instruction into their course. (5) Conclusions: This exploratory survey of faculty at one college of pharmacy indicated positive perceptions and opinions of telehealth integration into the Doctor of Pharmacy curriculum. Further efforts to incorporate telehealth into the curriculum at other pharmacy schools is warranted.
Full article
Open AccessArticle
Development, Feasibility, Impact and Acceptability of a Community Pharmacy-Based Diabetes Care Plan in a Low–Middle-Income Country
Pharmacy 2023, 11(4), 109; https://doi.org/10.3390/pharmacy11040109 - 26 Jun 2023
Abstract
Informed by existing research, mostly from high-income countries, this study aimed to develop and test the feasibility of a community pharmacy person-centred goal-setting intervention for people living with type 2 diabetes in a low–middle-income country—Nigeria. The Medical Research Council (MRC) guidance for developing
[...] Read more.
Informed by existing research, mostly from high-income countries, this study aimed to develop and test the feasibility of a community pharmacy person-centred goal-setting intervention for people living with type 2 diabetes in a low–middle-income country—Nigeria. The Medical Research Council (MRC) guidance for developing complex interventions framed the intervention development. Patients participated in monthly community pharmacist consultations over six months. Self-reported and clinical outcome measures were collected at baseline and study completion and analysed in STATA V.14. Twenty pharmacists in 20 pharmacies completed the research and enrolled 104 patients. Of these, 89 patients had complete study data, and 70 patients also completed a post-study evaluation questionnaire. In addition, 15 patients and 10 pharmacists were interviewed. All outcome measures showed statistically significant improvements (p < 0.05). Clinical outcomes (BMI, waist circumference, and fasting plasma glucose) improved significantly. Mean patient activation measure (PAM©), quality of life (EQ-VAS©), and medication adherence improved from baseline to study completion. Eighty-eight per cent of questionnaire respondents were satisfied with the service. Interviews indicated care plan acceptability, patient satisfaction, empowerment, and service enthusiasm. Identified barriers to the consultations included time and technology. This study developed a feasible, effective, well-perceived community pharmacy diabetes care plan in Nigeria.
Full article
(This article belongs to the Special Issue Pharmaceutical Care Services in Pharmacy Practice)
►▼
Show Figures
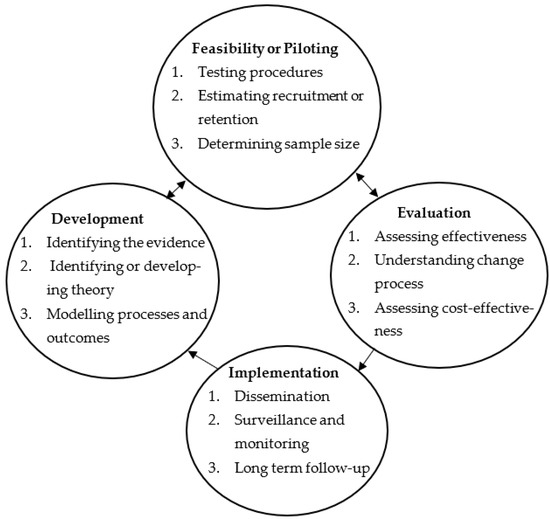
Figure 1
Open AccessArticle
Evaluation of Systemic Antifungal Use in a Latin American General Care Hospital: A Retrospective Study
by
, , and
Pharmacy 2023, 11(4), 108; https://doi.org/10.3390/pharmacy11040108 - 24 Jun 2023
Abstract
Background: Invasive fungal infections significantly contribute to mortality and morbidity rates. Despite the presence of all four major classes of antifungal medications, it is estimated that these infections result in the death of 1.5 million people each year, and death rates are increasing
[...] Read more.
Background: Invasive fungal infections significantly contribute to mortality and morbidity rates. Despite the presence of all four major classes of antifungal medications, it is estimated that these infections result in the death of 1.5 million people each year, and death rates are increasing at an alarming rate. With increasing concerns about the emergence of antifungal resistance, there is a growing consideration in many countries to incorporate antifungal stewardship into existing antimicrobial stewardship programs. This approach aims to address issues hindering the appropriate use of antifungal drugs and to optimize their utilization. Methods: An analytical retrospective study of 48 hospitalized patients was conducted to assess factors related to the use of systemic antifungals and develop and implement an internal protocol to improve its use. Results: All patients with severe comorbidity had SOFA scores linked with a mortality risk of more than 10%. Based on 48 evaluations of antifungal orders, 62.5% were considered appropriate, 14.6% were considered debatable, and 22.9% were considered inappropriate. Infectious disease physicians made most of the prescriptions considered appropriate in this study. Conclusions: Comorbidities and risk factors in patients receiving systemic antifungals can be associated with the development of more serious fungal infections; hence, the implementation of antifungal stewardship as a complement to antimicrobial stewardship programs can help facilitate decision-making when dealing with a suspected case of fungal infection.
Full article
(This article belongs to the Special Issue Improving Antimicrobial Use in Hospitalized Patients 2.0)
►▼
Show Figures
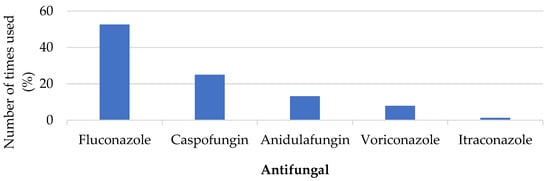
Figure 1
Open AccessOpinion
Would I Trust or Will I Trust? The Gap between Entrustment Determinations and Entrustment Decisions for Trainees in Pharmacy and Other Health Professions
by
and
Pharmacy 2023, 11(3), 107; https://doi.org/10.3390/pharmacy11030107 - 18 Jun 2023
Cited by 1
Abstract
Entrustable Professional Activities (EPAs) and entrustment decision making are rapidly becoming mainstream in competency-based education in the health professions. EPAs are the units of professional practice to entrust graduates with once they have developed the required competencies. They were conceived to enable a
[...] Read more.
Entrustable Professional Activities (EPAs) and entrustment decision making are rapidly becoming mainstream in competency-based education in the health professions. EPAs are the units of professional practice to entrust graduates with once they have developed the required competencies. They were conceived to enable a gradual increase in professional autonomy during training, by allowing trainees to practice activities in which they have demonstrated they have mastered well, with decreasing supervision. However, practicing health care unsupervised generally requires licensure. The question for pharmacy education, as well as for undergraduate medical education, is can students be given any autonomy in practice, even when they have fully mastered an EPA yet remain unlicensed? While entrustment decisions for licensed practitioners have autonomy consequences, some educators in undergraduate programs speak of ‘entrustment determinations’, to avoid decisions about students that affect patient care, in other words saying, we would trust you, rather than we will trust you. However, graduating learners without the experience of responsibility and reasonable autonomy creates a gap with full practice responsibilities, which may jeopardize patient safety after training. What can programs do to retain the power of using EPAs while at the same time guarding patient safety?
Full article
(This article belongs to the Special Issue Advances in Experiential Learning in Pharmacy)

Journal Menu
► ▼ Journal Menu-
- Pharmacy Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Editorial Office
- 10th Anniversary of Pharmacy
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
JCM, Pharmaceuticals, Pharmacoepidemiology, Pharmacy, Vaccines, Healthcare
Mass Vaccination Campaigns: From Post-authorization Benefit-Risk Assessment to Public Health Impact
Topic Editors: Giampiero Mazzaglia, Lorenzo Mantovani, Ippazio Cosimo AntonazzoDeadline: 30 November 2023
Topic in
Antioxidants, Applied Biosciences, Biomolecules, Horticulturae, Molecules, Pharmacy, Plants
Bioactive Substances, Pharmacognosy and Metabolomics
Topic Editors: Jiri Gruz, Lucie RárováDeadline: 10 December 2023
Topic in
Healthcare, JPM, Medicines, Pharmacy, Pharmaceutics, Pharmaceuticals
Drug Utilization and Medication Adherence: Strategies, Technologies and Practices
Topic Editors: Tamás Ágh, Enrica MendittoDeadline: 31 December 2023
Topic in
Healthcare, IJERPH, JCM, Nutrients, Pharmacy
The Promotion and Development of Community Health for Personal Health: Theories and Applications
Topic Editors: Yang Gao, Lianyong Qi, Chia-Huei Wu, Yu-Hsi Yuan, Datian BiDeadline: 31 August 2024

Conferences
Special Issues
Special Issue in
Pharmacy
Pharmacy Reviews in 2022
Guest Editors: Jack Fincham, Jon SchommerDeadline: 15 August 2023
Special Issue in
Pharmacy
Pharmaceutical Care Services in Pharmacy Practice
Guest Editors: Andrea Brajkovic, Iva MucaloDeadline: 1 September 2023
Special Issue in
Pharmacy
Pharmacists’ Role in Reducing Problematic Opioid Use
Guest Editor: Catriona MathesonDeadline: 15 September 2023
Special Issue in
Pharmacy
Women’s Special Issue Series: Pharmacy
Guest Editors: Maree Simpson, Cheryl A. Sadowski, Daisy VolmerDeadline: 30 September 2023
Topical Collections
Topical Collection in
Pharmacy
New Insights into Pharmacy Teaching and Learning during COVID-19
Collection Editors: Ana Seselja Perisin, Darko Modun









