Journal Description
Onco
Onco
is an international, peer-reviewed, open access journal on the whole field of oncotargets and cancer therapies research published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- Rapid Publication: first decisions in 16 days; acceptance to publication in 5.8 days (median values for MDPI journals in the first half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Onco is a companion journal of Cancers.
Latest Articles
Peripheral Blood CD8+ T-Lymphocyte Subsets Are Associated with Prognosis in Prostate Cancer Patients
Onco 2023, 3(3), 165-174; https://doi.org/10.3390/onco3030012 - 26 Jul 2023
Abstract
►
Show Figures
Background: Various studies have reported associations between frequencies of total peripheral blood lymphocytes and prostate cancer prognosis, but none so far has addressed the prognostic role of CD8+ T-lymphocyte subsets. Methods: A total of 43 prostate cancer patients with metastatic disease and 81
[...] Read more.
Background: Various studies have reported associations between frequencies of total peripheral blood lymphocytes and prostate cancer prognosis, but none so far has addressed the prognostic role of CD8+ T-lymphocyte subsets. Methods: A total of 43 prostate cancer patients with metastatic disease and 81 patients with non-metastatic disease were included in this study. Flow cytometry analyses were employed for determining the frequencies of peripheral CD8+ T-lymphocyte subsets. Results: Statistically significant lower levels of terminally differentiated effector (TEMRA) cells in patients with non-metastatic disease vs. patients with metastatic disease were observed. Central memory (CM) and effector memory (EM) CD8+ subsets, were found to be significantly higher in patients with non-metastatic disease vs. patients with metastatic disease. A similar profile was revealed when these CD8+ subsets were analyzed based on the patients’ Gleason scores, as well as by combined disease stage (i.e., non-metastatic vs. metastatic disease) and Gleason score. Conclusions: Peripheral blood-derived CD8+ T-lymphocyte memory subsets could function as biomarkers for the prognosis of PCa.
Full article
Open AccessReview
NUP98 Rearrangements in AML: Molecular Mechanisms and Clinical Implications
Onco 2023, 3(3), 147-164; https://doi.org/10.3390/onco3030011 - 18 Jul 2023
Abstract
►▼
Show Figures
NUP98 fusions constitute a small subgroup of AML patients and remain a high-risk AML subtype. There are approximately 30 types of NUP98 fusions identified in AML patients. These patients show resistance to currently available therapies and poor clinical outcomes. NUP98 fusions with different
[...] Read more.
NUP98 fusions constitute a small subgroup of AML patients and remain a high-risk AML subtype. There are approximately 30 types of NUP98 fusions identified in AML patients. These patients show resistance to currently available therapies and poor clinical outcomes. NUP98 fusions with different fusion partners have oncogenic transformation potential. This review describes how the NUP98 gene acquires oncogenic properties after rearrangement with multiple partners. In the mechanistic part, the formation of nuclear bodies and dysregulation of the HoxA/Meis1 pathway are highlighted. This review also discusses mutational signatures among NUP98 fusions and their significance in leukemogenesis. It also discusses the clinical implications of NUP98 fusions and their associated mutations in AML patients. Furthermore, it highlights therapeutic vulnerabilities in these leukemias that can be exploited as therapeutic strategies. Lastly, this review discusses the gaps in our knowledge regarding NUP98 fusions in AML, as well as future research opportunities.
Full article
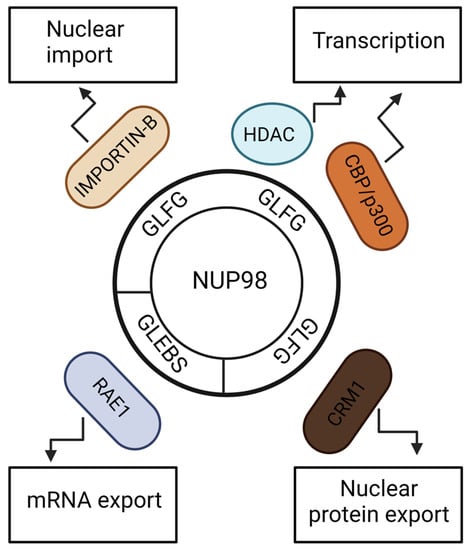
Figure 1
Open AccessReview
Precision Medicine Revolutionizing Esophageal Cancer Treatment: Surmounting Hurdles and Enhancing Therapeutic Efficacy through Targeted Drug Therapies
Onco 2023, 3(3), 127-146; https://doi.org/10.3390/onco3030010 - 15 Jul 2023
Abstract
►▼
Show Figures
Esophageal cancer is a formidable challenge in the realm of cancer treatment. Conventional methods such as surgery, chemotherapy, and immunotherapy have demonstrated limited success rates in managing this disease. In response, targeted drug therapies have emerged as a promising strategy to improve outcomes
[...] Read more.
Esophageal cancer is a formidable challenge in the realm of cancer treatment. Conventional methods such as surgery, chemotherapy, and immunotherapy have demonstrated limited success rates in managing this disease. In response, targeted drug therapies have emerged as a promising strategy to improve outcomes for patients. These therapies aim to disrupt specific pathways involved in the growth and development of esophageal cancer cells. This review explores various drugs used to target specific pathways, including cetuximab and monoclonal antibodies (gefitinib) that target the epidermal growth factor receptor (EGFR), trastuzumab that targets human epidermal growth factor receptor 2 (HER-2), drugs targeting the vascular endothelial growth factor receptor (VEGFR), mTOR inhibitors, and cMET inhibitors. Additionally, the article discusses the impact of drug resistance on the effectiveness of these therapies, highlighting factors such as cancer stem cells, cancer-associated fibroblasts, immune-inflammatory cells, cytokines, hypoxia, and growth factors. While drug targeting approaches do not provide a complete cure for esophageal cancer due to drug resistance and associated side effects, they offer potential for improving patient survival rates.
Full article

Figure 1
Open AccessEditorial
Onco: A Promising Player Amidst Oncology Journals
Onco 2023, 3(2), 125-126; https://doi.org/10.3390/onco3020009 - 01 Jun 2023
Abstract
As the new Editor-in-Chief of the journal, I believe that I must continue the efforts of my predecessor even more actively and with greater enthusiasm and dedication so that the journal becomes a pole of attraction for the publication of excellent studies of
[...] Read more.
As the new Editor-in-Chief of the journal, I believe that I must continue the efforts of my predecessor even more actively and with greater enthusiasm and dedication so that the journal becomes a pole of attraction for the publication of excellent studies of basic, translational and clinical research for the treatment of cancer [...]
Full article
Open AccessReview
A Comprehensive Review on the Role of Human Epidermal Growth Factor Receptor 2 (HER2) as a Biomarker in Extra-Mammary and Extra-Gastric Cancers
by
, , , , , , and
Onco 2023, 3(2), 96-124; https://doi.org/10.3390/onco3020008 - 26 May 2023
Abstract
►▼
Show Figures
The human epidermal growth factor receptors (HERs) are expressed abundantly in the human body. The tumorigenic potential of HER2/neu is linked to its overexpression, amplification or somatic mutation. The HER2 gene amplification leading to protein overexpression has been reported in 25–30% of breast
[...] Read more.
The human epidermal growth factor receptors (HERs) are expressed abundantly in the human body. The tumorigenic potential of HER2/neu is linked to its overexpression, amplification or somatic mutation. The HER2 gene amplification leading to protein overexpression has been reported in 25–30% of breast cancers and 10–30% of gastric/gastroesophageal cancers. While HER2 is a well-documented predictive, prognostic, and therapeutic marker in breast and gastric/gastroesophageal cancers, its relevance has also been demonstrated in multiple other malignancies. In this article, we will conduct an extensive review of current data pertaining to HER2 amplification, overexpression, or mutation in cancers other than breast and gastric cancers.
Full article

Figure 1
Open AccessArticle
Transcriptome Analysis Identifies Tumor Immune Microenvironment Signaling Networks Supporting Metastatic Castration-Resistant Prostate Cancer
by
, , , , and
Onco 2023, 3(2), 81-95; https://doi.org/10.3390/onco3020007 - 10 Apr 2023
Abstract
Prostate cancer (PCa) is the second most common cause of cancer death in American men. Metastatic castration-resistant prostate cancer (mCRPC) is the most lethal form of PCa and preferentially metastasizes to the bones through incompletely understood molecular mechanisms. Herein, we processed RNA sequencing
[...] Read more.
Prostate cancer (PCa) is the second most common cause of cancer death in American men. Metastatic castration-resistant prostate cancer (mCRPC) is the most lethal form of PCa and preferentially metastasizes to the bones through incompletely understood molecular mechanisms. Herein, we processed RNA sequencing data from patients with mCRPC (n = 60) and identified 14 gene clusters (modules) highly correlated with mCRPC bone metastasis. We used a novel combination of weighted gene co-expression network analysis (WGCNA) and upstream regulator and gene ontology analyses of clinically annotated transcriptomes to identify the genes. The cyan module (M14) had the strongest positive correlation (0.81, p = 4 × 10−15) with mCRPC bone metastasis. It was associated with two significant biological pathways through KEGG enrichment analysis (parathyroid hormone synthesis, secretion, and action and protein digestion and absorption). In particular, we identified 10 hub genes (ALPL, PHEX, RUNX2, ENPP1, PHOSPHO1, PTH1R, COL11A1, COL24A1, COL22A1, and COL13A1) using cytoHubba of Cytoscape. We also found high gene expression for collagen formation, degradation, absorption, cell-signaling peptides, and bone regulation processes through Gene Ontology (GO) enrichment analysis.
Full article
(This article belongs to the Topic Molecular Profiling and Identification of Molecular Signatures Associated with Tissue Development, Tumorigenesis, and Anticancer Agents’ Action)
►▼
Show Figures
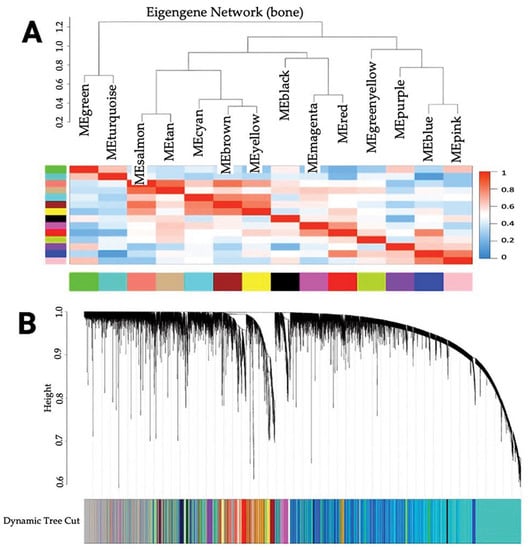
Figure 1
Open AccessArticle
CT Radiomics and Clinical Feature Model to Predict Lymph Node Metastases in Early-Stage Testicular Cancer
by
, , , , , , , and
Onco 2023, 3(2), 65-80; https://doi.org/10.3390/onco3020006 - 10 Apr 2023
Abstract
Accurate retroperitoneal lymph node metastasis (LNM) prediction in early-stage testicular germ cell tumours (TGCTs) harbours the potential to significantly reduce over- or undertreatment and treatment-related morbidity in this group of young patients as an important survivorship imperative. We investigated the role of computed
[...] Read more.
Accurate retroperitoneal lymph node metastasis (LNM) prediction in early-stage testicular germ cell tumours (TGCTs) harbours the potential to significantly reduce over- or undertreatment and treatment-related morbidity in this group of young patients as an important survivorship imperative. We investigated the role of computed tomography (CT) radiomics models integrating clinical predictors for the individualised prediction of LNM in early-stage TGCT. Ninety-one patients with surgically proven testicular germ cell tumours and contrast-enhanced CT were included in this retrospective study. Dedicated radiomics software was used to segment 273 retroperitoneal lymph nodes and extract features. After feature selection, radiomics-based machine learning models were developed to predict LN metastasis. The robustness of the procedure was controlled by 10-fold cross-validation. Using multivariable logistic regression modelling, we developed three prediction models: a radiomics-only model, a clinical-only model, and a combined radiomics–clinical model. The models’ performances were evaluated using the area under the receiver operating characteristic curve (AUC). Finally, decision curve analysis was performed to estimate the clinical usefulness of the predictive model. The radiomics-only model for predicting lymph node metastasis reached a greater discrimination power than the clinical-only model, with an AUC of 0.87 (±0.04; 95% CI) vs. 0.75 (±0.08; 95% CI) in our study cohort. The combined model integrating clinical risk factors and selected radiomics features outperformed the clinical-only and the radiomics-only prediction models, and showed good discrimination with an area under the curve of 0.89 (±0.03; 95% CI). The decision curve analysis demonstrated the clinical usefulness of our proposed combined model. The presented combined CT-based radiomics–clinical model represents an exciting non-invasive tool for individualised LN metastasis prediction in testicular germ cell tumours. Multi-centre validation is required to generate high-quality evidence for its clinical application.
Full article
(This article belongs to the Topic Artificial Intelligence in Cancer Diagnosis and Therapy)
►▼
Show Figures
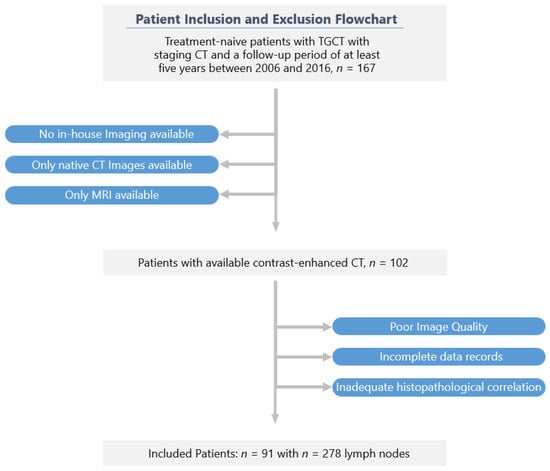
Figure 1
Open AccessArticle
The Chart Diagnostic System Improves the Diagnostic Accuracy of Cervical Lymph Node Metastasis in Oral Squamous Cell Carcinoma
by
, , , , , and
Onco 2023, 3(1), 53-64; https://doi.org/10.3390/onco3010005 - 07 Feb 2023
Abstract
►▼
Show Figures
Purpose: To establish a diagnosis method based on imaging findings and histopathological factors associated with cervical lymph node metastasis. Methods: A total of 1587 cervical lymph nodes that were detected using imaging tools in 73 OSCC patients who underwent surgical treatment were enrolled
[...] Read more.
Purpose: To establish a diagnosis method based on imaging findings and histopathological factors associated with cervical lymph node metastasis. Methods: A total of 1587 cervical lymph nodes that were detected using imaging tools in 73 OSCC patients who underwent surgical treatment were enrolled to evaluate the association between imaging findings (long diameter, short diameter, long–short ratio, US findings (hilum and internal echo), contrast effect with enhanced CT, standardized uptake value (SUV) max and SUV average with 18F FDG-Positron Emission Tomography (PET)) and metastatic cervical lymph nodes. In 57 OSCC patients, biopsy specimens were evaluated for histopathologic factors (budding score, lymphatic invasion, vascular invasion, nerve invasion, and YK classification) and the presence of cervical lymph node metastases. Cervical lymph node metastasis was determined based on histopathological examination of the lymph nodes of patients with no metastasis observed 3 years after primary surgery. Results: In total, 22 of the 73 patients had cervical lymph node metastasis pathologically. In the comparison of the presence of metastatic lymph nodes, univariate analysis showed significant differences in cervical lymph node long and short diameter, long/short ratio, internal echo, rim enhancement, SUV max, SUV average, budding score, and vascular invasion. Multivariable analysis showed significant differences in internal echo, rim enhancement, SUV max, and budding score. Conclusions: We propose a chart diagnostic system that combines imaging and histopathological findings to improve the diagnosis of cervical lymph node metastasis.
Full article
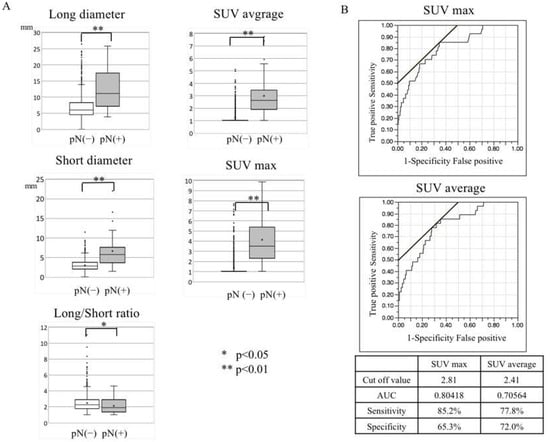
Figure 1
Open AccessArticle
Fractionated Volumetric Modulated Arc Therapy (FVMAT) for Oligometastatic Brain Tumor
Onco 2023, 3(1), 43-52; https://doi.org/10.3390/onco3010004 - 02 Feb 2023
Abstract
Intracranial metastasis is very common in adult cancer patients with an overall incidence of approximately 10–40%. The most common primary tumors responsible for this in adults are lung and breast cancer. Brain metastasis signifies a grave prognosis, with a median survival of 6
[...] Read more.
Intracranial metastasis is very common in adult cancer patients with an overall incidence of approximately 10–40%. The most common primary tumors responsible for this in adults are lung and breast cancer. Brain metastasis signifies a grave prognosis, with a median survival of 6 to 12 months. They are traditionally managed with palliative care and whole brain radiotherapy (WBRT). WBRT was an effective method to control brain metastases, decreasing corticosteroid use to control tumor-associated edema, and potentially improving overall survival; however, WBRT was found to be associated with a serious neurocognitive degeneration, this adverse effect (AE) follows a biphasic pattern beginning with a transient decline in mental functioning at around 4 months post-treatment, slowly leading to an irreversible neurologic impairment from months to years later. Evidence supports that WBRT can cause radiation injury to the hippocampus, which in turn will lead to a decline in neurocognitive function (NCF). Volumetric modulated arc therapy (VMAT) is a relatively new type of image-guided radiotherapy that treats multiple brain metastasis simultaneously and efficiently with less neurocognitive sequelae. Eighteen cancer patients with limited (≤5 brain tumors) or oligometastatic brain tumor were treated with a spatially fractionated VMAT technique for a total dose of 30 Gy in 10 fractions, the patients tolerated the VMAT treatment with no radiation-induced neurologic toxicities after a mean follow-up of 1 year. Local control rate was 84%, and the median survival for these 19 patients was 11.3 months (range: 9.1–22.4 months). In conclusion, the VMAT is a suitable technique that is a safe and effective treatment for brain oligometastases.
Full article
(This article belongs to the Topic Cancer Biology and Radiation Therapy)
►▼
Show Figures
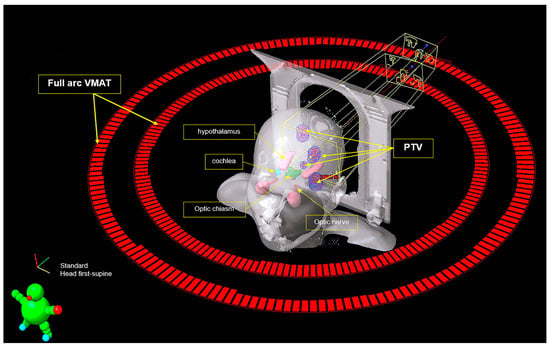
Figure 1
Open AccessReview
Risk Factors and Prevention of Gastric Cancer Development—What Do We Know and What Can We Do?
by
, , , , and
Onco 2023, 3(1), 26-42; https://doi.org/10.3390/onco3010003 - 30 Jan 2023
Cited by 1
Abstract
Gastric cancer (GC) is one of the most common causes of cancer-related deaths. Gastric tumors show a high aggressiveness, which, in turn, contributes to a low survival rate of fewer than 12 months. Considering the above, it was decided to review the current
[...] Read more.
Gastric cancer (GC) is one of the most common causes of cancer-related deaths. Gastric tumors show a high aggressiveness, which, in turn, contributes to a low survival rate of fewer than 12 months. Considering the above, it was decided to review the current scientific studies that indicate the potential prevention of gastric cancer and clarify the relationship between gastric cancer and the composition of the microorganisms inhabiting the human body. Accordingly, a review paper was prepared based on 97 scientific sources from 2011 to 2022. Particular attention was paid to the most recent scientific studies from the last five years, which account for more than 80% of the cited sources. Taking care of one’s overall health, including undertaking treatment for Helicobacter pylori infection, and following a diet high in anti-inflammatory and immunomodulatory ingredients are the most important factors in reducing the risk of developing gastric cancer.
Full article
(This article belongs to the Topic Non Herbal Nutraceutical, Probiotic, Vitamins and Fatty Acids in Cancer)
►▼
Show Figures
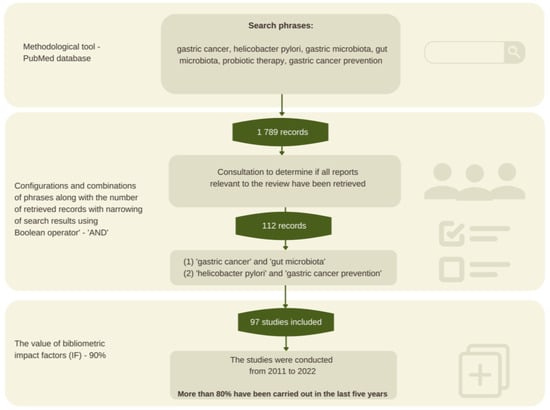
Figure 1
Open AccessArticle
Regulation of Epithelial–Mesenchymal Transition Pathway and Artificial Intelligence-Based Modeling for Pathway Activity Prediction
by
, , , , , , , and
Onco 2023, 3(1), 13-25; https://doi.org/10.3390/onco3010002 - 06 Jan 2023
Abstract
Because activity of the epithelial–mesenchymal transition (EMT) is involved in anti-cancer drug resistance, cancer malignancy, and shares some characteristics with cancer stem cells (CSCs), we used artificial intelligence (AI) modeling to identify the cancer-related activity of the EMT-related pathway in datasets of gene
[...] Read more.
Because activity of the epithelial–mesenchymal transition (EMT) is involved in anti-cancer drug resistance, cancer malignancy, and shares some characteristics with cancer stem cells (CSCs), we used artificial intelligence (AI) modeling to identify the cancer-related activity of the EMT-related pathway in datasets of gene expression. We generated images of gene expression overlayed onto molecular pathways with Ingenuity Pathway Analysis (IPA). A dataset of 50 activated and 50 inactivated pathway images of EMT regulation in the development pathway was then modeled by the DataRobot Automated Machine Learning platform. The most accurate models were based on the Elastic-Net Classifier algorithm. The model was validated with 10 additional activated and 10 additional inactivated pathway images. The generated models had false-positive and false-negative results. These images had significant features of opposite labels, and the original data were related to Parkinson’s disease. This approach reliably identified cancer phenotypes and treatments where EMT regulation in the development pathway was activated or inactivated thereby identifying conditions where therapeutics might be applied or developed. As there are a wide variety of cancer phenotypes and CSC targets that provide novel insights into the mechanism of CSCs’ drug resistance and cancer metastasis, our approach holds promise for modeling and simulating cellular phenotype transition, as well as predicting molecular-induced responses.
Full article
(This article belongs to the Topic Artificial Intelligence in Cancer Diagnosis and Therapy)
►▼
Show Figures
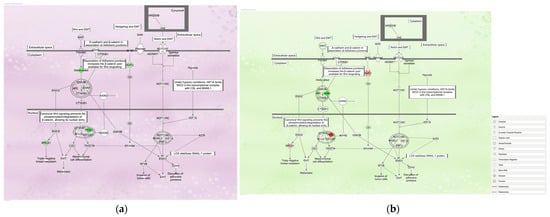
Figure 1
Open AccessReview
Review of Template-Based Neuroimaging Tools in Neuro-Oncology: Novel Insights
by
, , , , , , , , , , , and
Onco 2023, 3(1), 1-12; https://doi.org/10.3390/onco3010001 - 23 Dec 2022
Abstract
►▼
Show Figures
Background: A common MRI reference space allows for easy communication of findings, and has led to high-impact discoveries in neuroscience. Brain MRI of neuro-oncology patients with mass lesions or surgical cavities can now be accurately transformed into reference space, allowing for a
[...] Read more.
Background: A common MRI reference space allows for easy communication of findings, and has led to high-impact discoveries in neuroscience. Brain MRI of neuro-oncology patients with mass lesions or surgical cavities can now be accurately transformed into reference space, allowing for a reliable comparison across patients. Despite this, it is currently seldom used in neuro-oncology, leaving analytic tools untapped. The aim of this study was to systematically review the neuro-oncology literature utilizing reference space. Methods: A systematic review of the neuro-oncology publications was conducted according to PRISMA statement guidelines. Studies specially reporting the use of the Montreal Neurological Institute (MNI) reference space were included. Studies were categorized according to their type of input data and their contributions to the field. A sub-analysis focusing on connectomics and transcriptomics was also included. Results: We identified only 101 articles that utilized the MNI brain in neuro-oncology research. Tumor locations (n = 77) and direct electrocortical stimulation (n = 19) were the most common source of data. A majority of studies (n = 51) provided insights on clinical factors such as tumor subtype, growth progression, and prognosis. A small group of studies (n = 21) have used the novel connectomic and transcriptomic tools. Conclusions: Brain MRI of neuro-oncology patients can be accurately transformed to MNI space. This has contributed to enhance our understanding of a wide variety of clinical questions ranging from tumor subtyping to symptom mapping. Many advanced tools such as connectomics and transcriptomics remain relatively untapped, thereby hindering our knowledge of neuro-oncology.
Full article
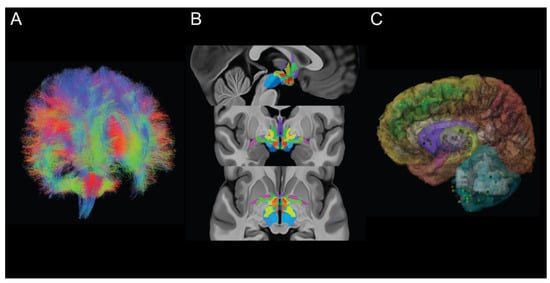
Figure 1
Open AccessArticle
Gene Screening in High-Throughput Right-Censored Lung Cancer Data
Onco 2022, 2(4), 305-318; https://doi.org/10.3390/onco2040017 - 17 Oct 2022
Abstract
►▼
Show Figures
Background: Advances in sequencing technologies have allowed collection of massive genome-wide information that substantially advances lung cancer diagnosis and prognosis. Identifying influential markers for clinical endpoints of interest has been an indispensable and critical component of the statistical analysis pipeline. However, classical variable
[...] Read more.
Background: Advances in sequencing technologies have allowed collection of massive genome-wide information that substantially advances lung cancer diagnosis and prognosis. Identifying influential markers for clinical endpoints of interest has been an indispensable and critical component of the statistical analysis pipeline. However, classical variable selection methods are not feasible or reliable for high-throughput genetic data. Our objective is to propose a model-free gene screening procedure for high-throughput right-censored data, and to develop a predictive gene signature for lung squamous cell carcinoma (LUSC) with the proposed procedure. Methods: A gene screening procedure was developed based on a recently proposed independence measure. The Cancer Genome Atlas (TCGA) data on LUSC was then studied. The screening procedure was conducted to narrow down the set of influential genes to 378 candidates. A penalized Cox model was then fitted to the reduced set, which further identified a 6-gene signature for LUSC prognosis. The 6-gene signature was validated on datasets from the Gene Expression Omnibus. Results: Both model-fitting and validation results reveal that our method selected influential genes that lead to biologically sensible findings as well as better predictive performance, compared to existing alternatives. According to our multivariable Cox regression analysis, the 6-gene signature was indeed a significant prognostic factor (p-value < 0.001) while controlling for clinical covariates. Conclusions: Gene screening as a fast dimension reduction technique plays an important role in analyzing high-throughput data. The main contribution of this paper is to introduce a fundamental yet pragmatic model-free gene screening approach that aids statistical analysis of right-censored cancer data, and provide a lateral comparison with other available methods in the context of LUSC.
Full article
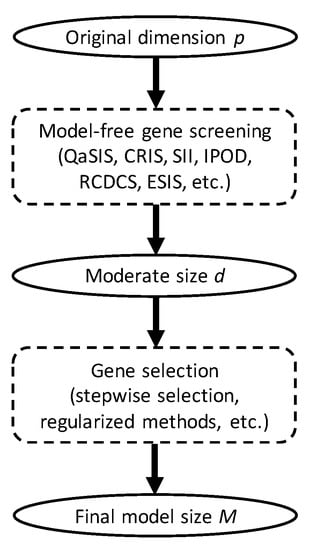
Figure 1
Open AccessArticle
ERBB1/EGFR and JAK3 Tyrosine Kinases as Potential Therapeutic Targets in High-Risk Multiple Myeloma
by
and
Onco 2022, 2(4), 282-304; https://doi.org/10.3390/onco2040016 - 14 Oct 2022
Cited by 2
Abstract
Our main objective was to identify abundantly expressed tyrosine kinases in multiple myeloma (MM) as potential therapeutic targets. We first compared the transcriptomes of malignant plasma cells from newly diagnosed MM patients who were risk-categorized based on the patient-specific EMC-92/SKY-92 gene expression signature
[...] Read more.
Our main objective was to identify abundantly expressed tyrosine kinases in multiple myeloma (MM) as potential therapeutic targets. We first compared the transcriptomes of malignant plasma cells from newly diagnosed MM patients who were risk-categorized based on the patient-specific EMC-92/SKY-92 gene expression signature values vs. normal plasma cells from healthy volunteers using archived datasets from the HOVON65/GMMG-HD4 randomized Phase 3 study evaluating the clinical efficacy of bortezomib induction/maintenance versus classic cytotoxic drugs and thalidomide maintenance. In particular, ERBB1/EGFR was significantly overexpressed in MM cells in comparison to normal control plasma cells, and it was differentially overexpressed in MM cells from high-risk patients. Amplified expression of EGFR/ERBB1 mRNA in MM cells was positively correlated with increased expression levels of mRNAs for several DNA binding proteins and transcription factors with known upregulating activity on EGFR/ERBB1 gene expression. MM patients with the highest ERBB1/EGFR expression level had significantly shorter PFS and OS times than patients with the lowest ERBB1/EGFR expression level. High expression levels of EGFR/ERBB1 were associated with significantly increased hazard ratios for unfavorable PFS and OS outcomes in both univariate and multivariate Cox proportional hazards models. The impact of high EGFR/ERBB1 expression on the PFS and OS outcomes remained significant even after accounting for the prognostic effects of other covariates. These results regarding the prognostic effect of EGFR/ERBB1 expression were validated using the MMRF-CoMMpass RNAseq dataset generated in patients treated with more recently applied drug combinations included in contemporary induction regimens. Our findings provide new insights regarding the molecular mechanism and potential clinical significance of upregulated EGFR/ERBB1 expression in MM.
Full article
(This article belongs to the Special Issue Feature Papers in Onco)
►▼
Show Figures
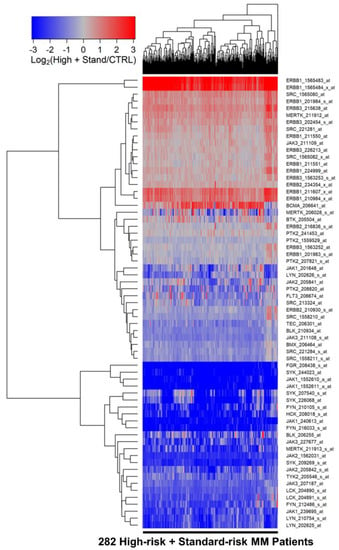
Figure 1
Open AccessArticle
The Dependence of Compensation Dose on Systematic and Random Interruption Treatment Time in Radiation Therapy
Onco 2022, 2(3), 264-281; https://doi.org/10.3390/onco2030015 - 05 Sep 2022
Abstract
►▼
Show Figures
Introduction: In this work, we develop a multi-scale model to calculate corrections to the prescription dose to predict compensation required for the DNA repair mechanism and the repopulation of the cancer cells due to the occurrence of patient scheduling variabilities and the treatment
[...] Read more.
Introduction: In this work, we develop a multi-scale model to calculate corrections to the prescription dose to predict compensation required for the DNA repair mechanism and the repopulation of the cancer cells due to the occurrence of patient scheduling variabilities and the treatment time-gap in fractionation scheme. Methods: A system of multi-scale, time-dependent birth-death Master equations is used to describe stochastic evolution of double-strand breaks (DSBs) formed on DNAs and post-irradiation intra and inter chromosomes end-joining processes in cells, including repair and mis-repair mechanisms in microscopic scale, with an extension appropriate for calculation of tumor control probability (TCP) in macroscopic scale. Variabilities in fractionation time due to systematic shifts in patient’s scheduling and randomness in inter-fractionation treatment time are modeled. For an illustration of the methodology, we focus on prostate cancer. Results: We derive analytical corrections to linear-quadratic radiobiological indices
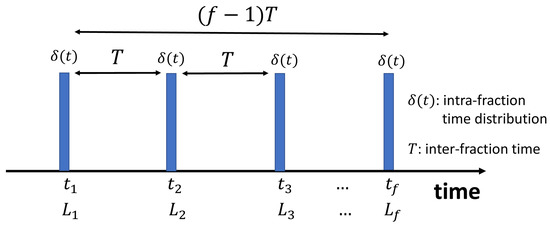
Figure 1
Open AccessArticle
Augmented Expression of the IL3RA/CD123 Gene in MLL/KMT2A-Rearranged Pediatric AML and Infant ALL
by
and
Onco 2022, 2(3), 245-263; https://doi.org/10.3390/onco2030014 - 25 Aug 2022
Abstract
Here, we evaluated transcript-level IL3RA/CD123 expression in mixed lineage leukemia 1 (MLL) gene/KMT2A-rearranged (MLL-R+) vs. MLL-R− pediatric AML as well as infant ALL by comparing the archived datasets of the transcriptomes of primary leukemic cells from the corresponding patient populations.
[...] Read more.
Here, we evaluated transcript-level IL3RA/CD123 expression in mixed lineage leukemia 1 (MLL) gene/KMT2A-rearranged (MLL-R+) vs. MLL-R− pediatric AML as well as infant ALL by comparing the archived datasets of the transcriptomes of primary leukemic cells from the corresponding patient populations. Our studies provide unprecedented evidence that IL3RA/CD123 expression exhibits transcript-level amplification in MLL-R+ pediatric AML and infant ALL cells. IL3RA was differentially upregulated in MLL-AF10+ (2.41-fold higher, p-value = 4.4 × 10−6) and MLL-AF6+ (1.83-fold higher, p-value = 9.9 × 10−4) but not in MLL-AF9+ cases compared to other pediatric AML cases. We also show that IL3RA/CD123 expression is differentially amplified in MLL-AF4+ (1.76-fold higher, p-value = 2.1 × 10−4) as well as MLL-ENL+ infant ALL (1.43-fold higher, p-value = 0.055). The upregulated expression of IL3RA/CD123 in MLL-R+ pediatric AML and infant ALL suggests that CD123 may be a suitable target for biotherapy in these high-risk leukemias.
Full article
(This article belongs to the Special Issue Feature Papers in Onco)
►▼
Show Figures
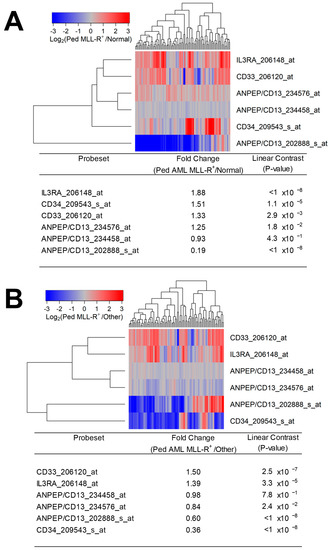
Figure 1
Open AccessReview
Genomic and Gene Expression Studies Helped to Define the Heterogeneity of Small-Cell Lung Cancer and Other Lung Neuroendocrine Tumors and to Identify New Therapeutic Targets
Onco 2022, 2(3), 186-244; https://doi.org/10.3390/onco2030013 - 15 Aug 2022
Abstract
►▼
Show Figures
Small-cell lung cancer (SCLC) is a high-grade neuroendocrine carcinoma, corresponding to about 15% of lung cancers, occurring predominantly in smokers and associated with a very poor prognosis. Key genetic alterations very frequently observed in SCLC are represented by the loss of TP53 and
[...] Read more.
Small-cell lung cancer (SCLC) is a high-grade neuroendocrine carcinoma, corresponding to about 15% of lung cancers, occurring predominantly in smokers and associated with a very poor prognosis. Key genetic alterations very frequently observed in SCLC are represented by the loss of TP53 and RB1, due to mutational events or deletions; frequent amplification or overexpression of MYC family genes (MYC, MYCL and MYCN); frequent genetic alterations by mutation/deletion of KMT2D, RB family members p107 (RBL1) and p130 (RBL2), PTEN, NOTCH receptors and CREBBP. The profile of expression of specific transcription factors allowed to differentiate four subtypes of SCLC defined according to levels of ASCL1 (SCLC-A), NEUROD1 (SCLC-N), POUF23 (SCLC-P) or YAP1 (SCLC-Y). A recent study identified the subgroup SCLC-I, characterized by the expression of inflammatory/immune-related genes. Recent studies have characterized at molecular level other lung neuroendocrine tumors, including large cell neuroendocrine cancers (LCNECs) and lung carcinoids. These molecular studies have identified some therapeutic vulnerabilities that can be targeted using specific drugs and some promising biomarkers that can predict the response to this treatment. Furthermore, the introduction of immunotherapy (immune checkpoint blockade) into standard first-line treatment has led to a significant clinical benefit in a limited subset of patients.
Full article
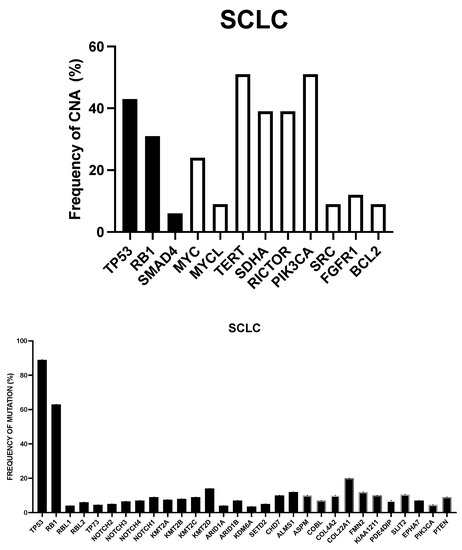
Figure 1
Open AccessCommentary
The Role of Liquid Biopsy in the Diagnostic Testing Algorithm for Advanced Lung Cancer
by
Onco 2022, 2(3), 181-185; https://doi.org/10.3390/onco2030012 - 14 Jul 2022
Cited by 2
Abstract
The discovery of therapeutically targetable oncogenic driver alterations has led to marked improvements in NSCLC outcomes. Targeted agents have been approved for an expanding list of biomarkers. Consequently, the accurate and timely identification of targetable alterations with diagnostic molecular profiling is crucial. The
[...] Read more.
The discovery of therapeutically targetable oncogenic driver alterations has led to marked improvements in NSCLC outcomes. Targeted agents have been approved for an expanding list of biomarkers. Consequently, the accurate and timely identification of targetable alterations with diagnostic molecular profiling is crucial. The use of multiplexed tissue assays, such as next-generation sequencing (NGS), has increased significantly. However, significant limitations with tissue NGS remain, such as insufficient tissue, scheduling limitations, the need for repeat biopsies, and long turnaround times. Liquid biopsies, using plasma circulating tumor DNA (ctDNA), have the potential to overcome these issues, with simpler sample processing requirements, greater convenience, and better patient acceptability. In particular, an early liquid biopsy may allow patients access to highly effective therapies faster, allow better symptom control and quality of life, prevent rapid clinical deterioration, and reduce patient anxiety at diagnosis. More broadly, it may also allow for the more cost-effective delivery of healthcare to patients.
Full article
(This article belongs to the Special Issue Feature Papers in Onco)
►▼
Show Figures
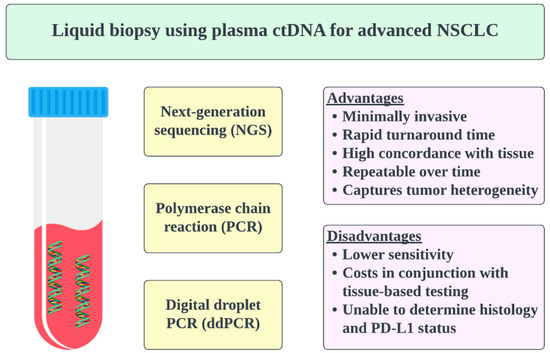
Figure 1
Open AccessReview
The Role of Immune Checkpoint Blockade in Acute Myeloid Leukemia
Onco 2022, 2(3), 164-180; https://doi.org/10.3390/onco2030011 - 11 Jul 2022
Cited by 1
Abstract
Immune checkpoint inhibition (ICI) has emerged as a therapeutic option for acute myeloid leukemia (AML) for patients that suffer from relapsed or high-risk disease, or patients ineligible for standard therapy. We aimed to study ICI as monotherapy and/or combined therapy (with chemotherapy (QT),
[...] Read more.
Immune checkpoint inhibition (ICI) has emerged as a therapeutic option for acute myeloid leukemia (AML) for patients that suffer from relapsed or high-risk disease, or patients ineligible for standard therapy. We aimed to study ICI as monotherapy and/or combined therapy (with chemotherapy (QT), for AML patients. The PRISMA statement was used. The literature used comprised clinical trials, randomized controlled trials, and systematic reviews published within the last 7 years. The blockade of CTLA-4 presented a 42% of complete remission within AML. Nivolumab in high-risk AML showed a median recurrence-free survival (RFS) of 8.48 months. The same drug on relapsed hematologic malignancies after allogenic transplantation shows a 1-year OS of 56%. The use of prophylaxis post allogenic transplantation cyclophosphamide (PTCy), following checkpoint inhibition, demonstrated different baseline disease and transplantation characteristics when compared to no-PCTy patients, being 32% and 10%, respectively. CTLA-4 blockage was a worthy therapeutic approach in relapsed hematologic malignancies, presenting long-lasting responses. The approach to AML and myelodysplastic syndrome patients with ICI before allogenic hematopoietic stem cell transplantation and the use of a graft-versus-host disease prophylaxis have shown improvement in the transplantation outcomes, and therefore AML treatment.
Full article
(This article belongs to the Special Issue Feature Papers in Onco)
►▼
Show Figures
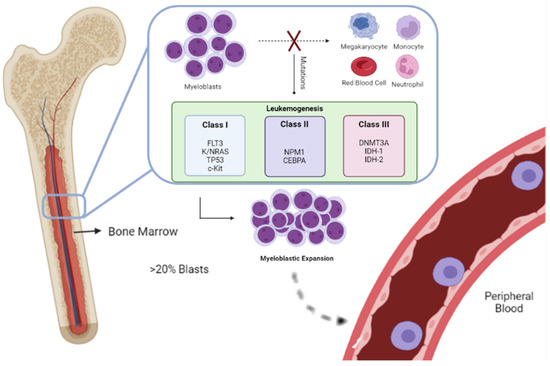
Figure 1
Open AccessArticle
Fucoxanthinol Promotes Apoptosis in MCF-7 and MDA-MB-231 Cells by Attenuating Laminins–Integrins Axis
by
, , , , , , , and
Onco 2022, 2(3), 145-163; https://doi.org/10.3390/onco2030010 - 08 Jul 2022
Abstract
Fucoxanthinol (FxOH), the main metabolite of the marine carotenoid fucoxanthin, exerts anti-cancer effects. However, fragmentary information is available on the growth-inhibiting effects of FxOH on breast cancer (BC). We investigated the growth-inhibiting effects of FxOH on human BC cells (MCF-7 and MDA-MB-231 cells),
[...] Read more.
Fucoxanthinol (FxOH), the main metabolite of the marine carotenoid fucoxanthin, exerts anti-cancer effects. However, fragmentary information is available on the growth-inhibiting effects of FxOH on breast cancer (BC). We investigated the growth-inhibiting effects of FxOH on human BC cells (MCF-7 and MDA-MB-231 cells), and the underlying mechanisms, differently from previous studies, by using comprehensive transcriptome analysis. The molecular mechanisms of FxOH were evaluated using flow cytometry, microarray, Western blotting, and gene knockdown analyses. FxOH (20 μM) significantly induced apoptosis in MCF-7 and MDA-MB-231 cells. Transcriptome analysis revealed that FxOH modulated the following 12 signaling pathways: extracellular matrix (ECM), adhesion, cell cycle, chemokine and cytokine, PI3K/AKT, STAT, TGF-β, MAPK, NF-κB, RAS/Rho, DNA repair, and apoptosis signals. FxOH downregulated the levels of laminin β1, integrin α5, integrin β1, integrin β4, cyclin D1, Rho A, phosphorylated (p)paxillin (Tyr31), pSTAT3(Ser727), and pSmad2(Ser465/467), which play critical roles in the 12 signaling pathways mentioned above. Additionally, FxOH upregulated the levels of pERK1/2(Thr202/Tyr204) and active form of caspase-3. Integrin β1 or β4 knockdown significantly inhibited the growth of MCF7 and MDA-MB-231 cells. These results suggest that FxOH induces apoptosis in human BC cells through some core signals, especially the ECM–integrins axis, and the downstream of cell cycle, STAT, TGF-β, RAS/Rho, MAPK, and/or DNA repair signals.
Full article
(This article belongs to the Special Issue Feature Papers in Onco)
►▼
Show Figures
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biology, Biomedicines, Cancers, Current Oncology, Onco
Targeting Signaling Networks for Cancer Therapy
Topic Editors: Renato Bassan, Jose-Maria Ribera, Linlin GuoDeadline: 5 September 2023
Topic in
Biomedicines, Cancers, Current Oncology, ncRNA, Onco
Non-coding RNAs in Cancer: Markers in Disease Progression and Therapy
Topic Editors: Balaji Krishnamachary, Oliver TreeckDeadline: 31 October 2023
Topic in
Biology, Cancers, Current Oncology, Diagnostics, Onco, JCM
Artificial Intelligence in Cancer, Biology and Oncology
Topic Editors: Ali Hekmatnia, Rahele Kafieh, Hamid KhayyamDeadline: 20 December 2023
Topic in
Biomolecules, Cancers, Current Oncology, JCM, Onco
Extracellular Vesicles in Cancer Diagnosis and Treatment
Topic Editors: Shenglin Huang, Linlin Guo, Jialei WangDeadline: 20 July 2024

Conferences
Special Issues
Special Issue in
Onco
Current Challenge and Future Advances for Lung Cancer: Genetics, Instrumental Diagnosis and Treatment 2.0
Guest Editor: Giovanni VicidominiDeadline: 20 November 2023
Special Issue in
Onco
Progress in Vaccination against Cancer - 2023 (PIVAC-23)
Guest Editors: Constantin N. Baxevanis, Sotirios P. Fortis, Maria GoulielmakiDeadline: 22 December 2023
Special Issue in
Onco
Targeting of Tumor Dormancy Pathway
Guest Editors: Athanassios Kotsinas, Constantin N. BaxevanisDeadline: 31 December 2023
Special Issue in
Onco
The Evolving Landscape of Contemporary Cancer Therapies
Guest Editor: Constantin N. BaxevanisDeadline: 29 March 2024











