-
 Rtf1 Transcriptionally Regulates Neonatal and Adult Cardiomyocyte Biology
Rtf1 Transcriptionally Regulates Neonatal and Adult Cardiomyocyte Biology -
 Left Atrial Strain Imaging by Speckle Tracking Echocardiography: The Supportive Diagnostic Value in Cardiac Amyloidosis and Hypertrophic Cardiomyopathy
Left Atrial Strain Imaging by Speckle Tracking Echocardiography: The Supportive Diagnostic Value in Cardiac Amyloidosis and Hypertrophic Cardiomyopathy -
 Longitudinal Changes in the Myocardial T1 Relaxation Time, Extracellular Volume Fraction, and Left Ventricular Function in Asymptomatic Men
Longitudinal Changes in the Myocardial T1 Relaxation Time, Extracellular Volume Fraction, and Left Ventricular Function in Asymptomatic Men -
 Cardioneuroablation Using Epicardial Pulsed Field Ablation for the Treatment of Atrial Fibrillation
Cardioneuroablation Using Epicardial Pulsed Field Ablation for the Treatment of Atrial Fibrillation
Journal Description
Journal of Cardiovascular Development and Disease
Journal of Cardiovascular Development and Disease
is an international, scientific, peer-reviewed, open access journal on cardiovascular medicine published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: CiteScore - Q2 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.1 days after submission; acceptance to publication is undertaken in 2.5 days (median values for papers published in this journal in the first half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.4 (2022);
5-Year Impact Factor:
3.0 (2022)
Latest Articles
Impact of Obesity on Atrial Electrophysiological Substrate
J. Cardiovasc. Dev. Dis. 2023, 10(8), 342; https://doi.org/10.3390/jcdd10080342 - 08 Aug 2023
Abstract
(1) Background. Obesity is a well-established worldwide recognised risk factor for atrial fibrillation (AF). Prior review papers reported on the associations between obesity and AF development, but not on the relation between obesity and atrial electrophysiology. We therefore conducted a systematic review to
[...] Read more.
(1) Background. Obesity is a well-established worldwide recognised risk factor for atrial fibrillation (AF). Prior review papers reported on the associations between obesity and AF development, but not on the relation between obesity and atrial electrophysiology. We therefore conducted a systematic review to describe the current knowledge of the characteristics of the atrial electrophysiological substrate in obese individuals and how they relate to the development of AF. (2) Methods. A search was conducted in Pubmed, Embase, and the Cochrane Library for publications evaluating the impact of obesity on atrial electrophysiology, electrical substrates, and their relation to the development of AF. (3) Results. A systematic literature search retrieved 477 potential publications based on the inclusion criteria; 76 full-text articles were selected for the present systematic review. The literature demonstrated that obesity predisposes to not only a higher AF incidence but also to more extensive atrial electrophysiological abnormalities increasing susceptibility to AF development. (4) Conclusion. Obesity may predispose to an overall increase in atrial electropathology, consisting of an increase in the slowing of the conduction, conduction block, low-voltage areas, and complex fractionated electrograms. To determine the impact of obesity-induced atrial electrical abnormalities on the long-term clinical outcome, further prospective studies are mandatory.
Full article
(This article belongs to the Special Issue Electropathology as the Foundation of Innovation in Diagnosis and Therapy of Atrial Fibrillation)
►
Show Figures
Open AccessCase Report
Intracoronary Pacing during “Chimney Technique” in Transcatheter Aortic Valve-in-Valve Implantation: An Alternative Temporary Rapid Ventricular Stimulation?
by
, , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 341; https://doi.org/10.3390/jcdd10080341 - 08 Aug 2023
Abstract
Temporary rapid ventricular pacing (TRVP) is required during transcatheter aortic valve implantation (TAVI) in order to reduce cardiac output and to facilitate balloon aortic valvuloplasty, prosthesis deployment, and post-deployment balloon dilation. The two most frequently used TRVP techniques are right endocardial (RE)-TRVP and
[...] Read more.
Temporary rapid ventricular pacing (TRVP) is required during transcatheter aortic valve implantation (TAVI) in order to reduce cardiac output and to facilitate balloon aortic valvuloplasty, prosthesis deployment, and post-deployment balloon dilation. The two most frequently used TRVP techniques are right endocardial (RE)-TRVP and retrograde left endocardial temporary rapid ventricular pacing (RLE)-TRVP. The first one could be responsible for cardiac tamponade, one of the most serious procedural complications during TAVI, while the second one could often be unsuccessful. Intracoronary (IC)-TRVP through a coronary guidewire has been described as a safe and efficient procedure that could avoid such complications. We describe two clinical cases in which IC-TRVP has been effectively used during valve-in-valve TAVI with coronary protection via the “chimney technique”, after unsuccessful RLE-TRVP.
Full article
(This article belongs to the Special Issue Aortic Stenosis: Diagnosis, Treatment and Management)
►▼
Show Figures

Figure 1
Open AccessArticle
First-Trimester Ultrasound Imaging for Prenatal Assessment of the Extended Cardiovascular System Using the Cardiovascular System Sonographic Evaluation Algorithm (CASSEAL)
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 340; https://doi.org/10.3390/jcdd10080340 - 07 Aug 2023
Abstract
Introduction and objectives: To compare fetal images obtained at the first- and second-trimester ultrasound scan when applying the Cardiovascular System Sonographic Evaluation Algorithm (CASSEAL). Methods: Using the CASSEAL protocol, nine sequential axial views were acquired in B-mode and color Doppler at the first-
[...] Read more.
Introduction and objectives: To compare fetal images obtained at the first- and second-trimester ultrasound scan when applying the Cardiovascular System Sonographic Evaluation Algorithm (CASSEAL). Methods: Using the CASSEAL protocol, nine sequential axial views were acquired in B-mode and color Doppler at the first- and second-trimester ultrasound scans, visualizing the main components of the extended fetal cardiovascular system. Images were compared qualitatively between both trimesters. Results: We obtained comparable images for all the nine axial views described in the CASSEAL protocol, with few differences and limitations. Conclusions: The CASSEAL protocol is reproducible in the first trimester, and could help in the early detection of fetal cardiovascular abnormalities. It represents a promising additional tool in order to increase the CHD detection rate.
Full article
(This article belongs to the Special Issue Echocardiography in Pediatric Heart Disease)
►▼
Show Figures
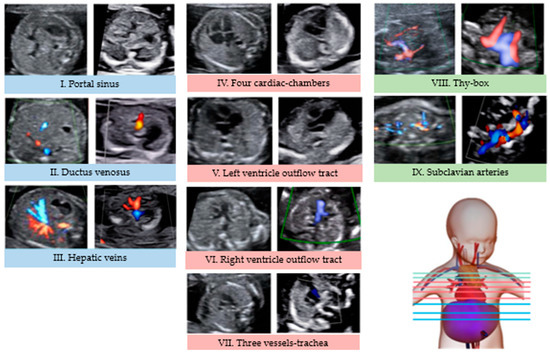
Figure 1
Open AccessCase Report
Transapical Mitral Valve-in-Ring Replacement Using the Innovative System under 3-Dimensional Printing Guidance
J. Cardiovasc. Dev. Dis. 2023, 10(8), 339; https://doi.org/10.3390/jcdd10080339 - 07 Aug 2023
Abstract
Background: Transcatheter mitral valve-in-ring replacement (TMViR) is an emerging alternative for patients with recurrent mitral regurgitation (MR) after a prior failed annuloplasty ring. However, intraoperative common issues and complications remain to be addressed. Case summary: We describe the case of a 67-year-old male
[...] Read more.
Background: Transcatheter mitral valve-in-ring replacement (TMViR) is an emerging alternative for patients with recurrent mitral regurgitation (MR) after a prior failed annuloplasty ring. However, intraoperative common issues and complications remain to be addressed. Case summary: We describe the case of a 67-year-old male patient who underwent surgical mitral concomitant tricuspid annuloplasty repair 7 years ago who developed recurrent severe MR (New York Heart Association functional class IV). To avoid a high-risk surgical reoperation, we chose to perform a TMViR using an innovative dedicated device—the Mi-thos system—via a transapical approach. A patient-specific, 3-dimensional printed model was used to guide the procedure to avoid potential challenges. The procedure was performed successfully, and the patient exhibited symptomatic improvement. Conclusions: This case report highlights the first use of the innovative Mi-thos system in a TMViR procedure. The findings demonstrate the feasibility and safety of utilizing the Mi-thos system, guided by 3-dimensional printing technology, for patients who have experienced recurrent mitral regurgitation MR following a failed annuloplasty ring.
Full article
(This article belongs to the Topic Usefulness and Clinical Applications of 3D Printing in Cardiovascular Diseases 2.0)
►▼
Show Figures
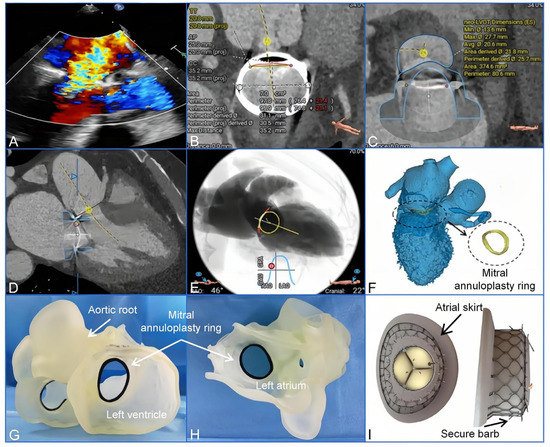
Figure 1
Open AccessArticle
Three Decades of Experience with Aortic Prosthetic Valve Endocarditis
by
, , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 338; https://doi.org/10.3390/jcdd10080338 - 06 Aug 2023
Abstract
The objective of this study was to evaluate early and long-term outcomes of patients with aortic prosthetic valve endocarditis (a-PVE) treated with a prosthetic aortic valve (PAV), prosthetic valved conduit (PVC), or cryopreserved aortic homograft (CAH). A total of 144 patients, 115 male
[...] Read more.
The objective of this study was to evaluate early and long-term outcomes of patients with aortic prosthetic valve endocarditis (a-PVE) treated with a prosthetic aortic valve (PAV), prosthetic valved conduit (PVC), or cryopreserved aortic homograft (CAH). A total of 144 patients, 115 male and 29 female, aged 67 ± 12 years, underwent surgery for a-PVE at our institution between 1994 and 2021. Median time from the original cardiac surgery was 1.9 [0.6–5.6] years, and 47 (33%) patients developed an early a-PVE. Of these patients, 73 (51%) underwent aortic valve replacement (AVR) with a biological or mechanical PAV, 12 (8%) underwent aortic root replacement (ARR) with a biological or mechanical PVC, and 59 (42%) underwent AVR or ARR with a CAH. Patients treated with a CAH had significantly more circumferential annular abscess multiple valve involvement, longer CPB and aortic cross-clamping times, and needed more postoperative pacemaker implantation than patients treated with a PAV. No difference was observed in survival, reoperation rates, or recurrence of IE between patients treated with a PAV, a PVC, or a CAH. CAHs are technically more demanding and more often used in patients who have extensive annular abscess and multiple valve involvement. However, the use of CAH is safe in patients with complex a-PVE, and it shows excellent early and long-term outcomes.
Full article
(This article belongs to the Special Issue Two of the Current Hot Challenges in Cardiac Surgery: Rising Endocarditis Cases and Extensive Use of Antithrombotics)
►▼
Show Figures

Figure 1
Open AccessReview
Arrhythmias in Patients with Cardiac Amyloidosis: A Comprehensive Review on Clinical Management and Devices
by
, , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 337; https://doi.org/10.3390/jcdd10080337 - 05 Aug 2023
Abstract
Cardiac amyloidosis (CA) is a rare but potentially life-threatening disease in which misfolded proteins accumulate in the cardiac wall tissue. Heart rhythm disorders in CA, including supraventricular arrhythmias, conduction system disturbances, or ventricular arrhythmias, play a major role in CA morbidity and mortality,
[...] Read more.
Cardiac amyloidosis (CA) is a rare but potentially life-threatening disease in which misfolded proteins accumulate in the cardiac wall tissue. Heart rhythm disorders in CA, including supraventricular arrhythmias, conduction system disturbances, or ventricular arrhythmias, play a major role in CA morbidity and mortality, and thus require supplementary management. Among them, AF is the most frequent arrhythmia during CA hospitalizations and is associated with significantly higher mortality, while ventricular arrhythmias are also common and are usually associated with poor prognosis. Early diagnosis of potential arrythmias could be performed through ECG, Holter monitoring, and/or electrophysiology study. Clinical management of these patients is quite significant, and it usually includes initiation of amiodarone and/or digoxin in patients with AF, potential electrical cardioversion, or ablation in specific patients with indication, as well as initiation of anticoagulants in all patients, independent of AF and CHADS-VASc score, for potential intracardiac thrombus. Moreover, identification of patients with conduction disorders that could benefit from prophylactic pacemaker implantation and/or CRT as well as identification of patients with life-threatening ventricular arrythmias that could benefit from ICD could both increase the survival rates of these patients and improve their quality of life.
Full article
(This article belongs to the Special Issue Feature Review Papers in Acquired Cardiovascular Disease)
►▼
Show Figures

Figure 1
Open AccessArticle
Subclinical Atrial Fibrillation on Prolonged ECG Holter Monitoring: Results from the Multicenter Real-World SAFARI (Silent Atrial Fibrillation ANCE-Sicily Research Initiative) Study
J. Cardiovasc. Dev. Dis. 2023, 10(8), 336; https://doi.org/10.3390/jcdd10080336 - 04 Aug 2023
Abstract
Background: The detection of subclinical/silent atrial fibrillation (SAF) in the general population is of the utmost importance, given its potential adverse consequences. Incident AF has been observed in 30% to 70% of patients with implanted devices, but its prevalence may indeed be lower
[...] Read more.
Background: The detection of subclinical/silent atrial fibrillation (SAF) in the general population is of the utmost importance, given its potential adverse consequences. Incident AF has been observed in 30% to 70% of patients with implanted devices, but its prevalence may indeed be lower in the general population. The prospective, multicentric, observational Silent Atrial Fibrillation ANCE Research Initiative (SAFARI) study aimed at assessing the SAF prevalence in a real-world outpatient setting by the means of a small, wearable, prolonged ECG Holter monitoring (>5 days) device (CGM HI 3-Lead ECG; CGM TELEMEDICINE, Piacenza, Italy). Methods: Patients ≥ 55 years of age at risk for AF were screened according to the inclusion criteria to undergo prolonged 3-lead ECG Holter monitoring. SAF episodes were classified as follows: Class A, <30 s; Class B, 30 to 299 s; and Class C, ≥300 s. Results: In total, 119 patients were enrolled (64 men; median age 71 (IQR 55–85) years). At a median of 13.5 (IQR 5–21) days of monitoring, SAF episodes were found in 19 patients (16%). A total of 10,552 arrhythmic episodes were registered, 6901 in Class A (n = 7 patients), 2927 in Class B (n = 3), and 724 in Class C (n = 9), (Class A vs. B and C, p < 0.001). This latter group had multiple (all-class) episodes, and two patients had >1000 episodes. There were no clinical, echocardiographic, or laboratory findings able to discriminate patients with SAF from those in sinus rhythm in univariate and multivariable analyses; of note is that the Class C patients showed a higher diastolic blood pressure, resting heart rate, and indexed LA volume. Conclusions. Over a median of 13 days of Holter monitoring, the SAFARI study confirmed the usefulness of small wearable devices in detecting SAF episodes in real-world outpatients at risk for, but with no prior history of, AF.
Full article
(This article belongs to the Special Issue Arrhythmic Risk Stratification)
►▼
Show Figures
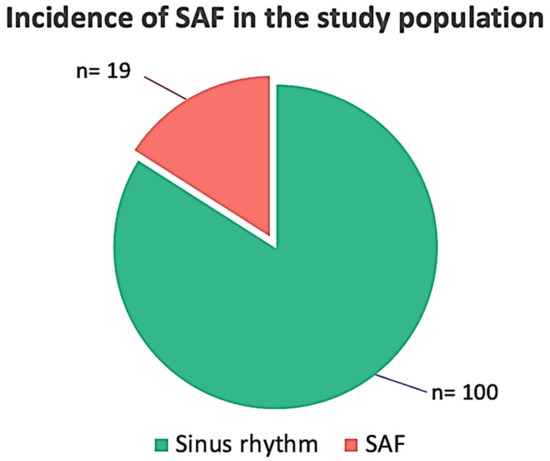
Figure 1
Open AccessBrief Report
The Clinical Validation of a Common Analytical Change Criteria for Cardiac Troponin for Ruling in an Acute Cardiovascular Outcome in Patients Presenting with Ischemic Chest Pain Symptoms
by
, , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 335; https://doi.org/10.3390/jcdd10080335 - 04 Aug 2023
Abstract
Serial cardiac troponin (cTn) testing on patients with symptoms suggestive of acute coronary syndrome (ACS) is primarily to identify those patients with evolving myocardial injury. With the improved analytical performance of the high-sensitivity cTn (hs-cTn) assays, different change criteria have been proposed that
[...] Read more.
Serial cardiac troponin (cTn) testing on patients with symptoms suggestive of acute coronary syndrome (ACS) is primarily to identify those patients with evolving myocardial injury. With the improved analytical performance of the high-sensitivity cTn (hs-cTn) assays, different change criteria have been proposed that are mostly assay dependent. Here, we developed and compared a new Common Change Criteria (3C for the combined criteria of >3 ng/L, >30%, or >15% based on the initial cTn concentration of <10 ng/L, 10 to 100 ng/L, or >100 ng/L, respectively) method, versus the 2 h assay-dependent absolute change criteria endorsed by the European Society of Cardiology (ESC), versus the common relative >20% change criterion. These different analytical change criteria were evaluated in 855 emergency department (ED) patients with symptoms of ACS and who had two samples collected 3 h apart. The cTn concentrations were measured with four different assays (Abbott hs-cTnI, Roche hs-cTnT, Ortho cTnI-ES, and Ortho hs-cTnI). The outcomes evaluated were myocardial infarction (MI) and a composite outcome (MI, unstable angina, ventricular arrhythmia, heart failure, or cardiovascular death) within 7 days of ED presentation. The combined change criteria (3C) method yielded higher specificities (range: 93.9 to 97.2%) as compared to the >20% criterion (range: 42.3 to 88.1%) for all four assays for MI. The 3C method only yielded a higher specificity estimate for MI for the cTnI-ES assay (95.9%) versus the absolute change criteria (71.7%). Similar estimates were obtained for the composite outcome. There was also substantial agreement between hs-cTnT and the different cTnI assays for MI with the 3C method, with the percent agreement being ≥95%. The Common Change Criteria (3C) method combining both absolute and different percent changes may be used with cTnI, hs-cTnT, and different hs-cTnI assays to yield similar high-specificity (rule-in) estimates for adverse cardiovascular events for patients presenting to the ED with ACS symptoms.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Electrocardiographic Characteristics of Ventricular Arrhythmias Originating from Different Areas Adjacent to the Mitral Annulus
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 334; https://doi.org/10.3390/jcdd10080334 - 03 Aug 2023
Abstract
Background: This study aimed to explore the electrocardiographic (ECG) characteristics of ventricular arrhythmias (VAs) arising from epicardial and endocardial areas adjacent to the mitral annulus (MA). Methods: This study involved 283 patients with MA-VAs who received radiofrequency catheter ablation at the center. The
[...] Read more.
Background: This study aimed to explore the electrocardiographic (ECG) characteristics of ventricular arrhythmias (VAs) arising from epicardial and endocardial areas adjacent to the mitral annulus (MA). Methods: This study involved 283 patients with MA-VAs who received radiofrequency catheter ablation at the center. The ECG characteristics of these patients were analyzed retrospectively. Results: The origin of MA-VAs was judged based on the ECG variables. Among all MA-VAs, intrinsicoid deflection time (IDT) > 77 ms or maximum deflection index (MDI) > 0.505 predicted the VAs arising from the epicardium (sensitivity of 70.20% and 73.51%, specificity of 94.70% and 82.58%, positive predictive value (PPV) of 93.81% and 82.84%, and negative predictive value (NPV) of 73.53% and 73.15%). Among all epicardial MA-VAs, the RV1/RV2 ratio > 0.87 predicted the VAs originating from the epicardial anteroseptal wall adjacent to the MA. It had a sensitivity, specificity, PPV, and NPV of 62.86%, 98.06%, 91.67%, and 88.60%, respectively. Among all endocardial MA-VAs, Q(q)R(r) morphology in lead V1 predicted the VAs arising from the endocardial septal wall adjacent to the MA. It had a sensitivity, specificity, PPV, and NPV of 92.98%, 100%, 100%, and 94.94%, respectively. Among all endocardial septal MA-VAs, a predominant positive wave in lead II and a predominant negative wave in lead III predicted the VAs arising from the endocardial midseptal portion adjacent to the MA. It had a sensitivity, specificity, PPV, and NPV of 86.04%, 100%, 100%, and 70.00%, respectively. Conclusion: the ECG characteristics of VAs from the different sites adjacent to the MA can enable judging the arrhythmia’s origin and designing the ablation plan accordingly.
Full article
(This article belongs to the Section Electrophysiology and Cardiovascular Physiology)
►▼
Show Figures
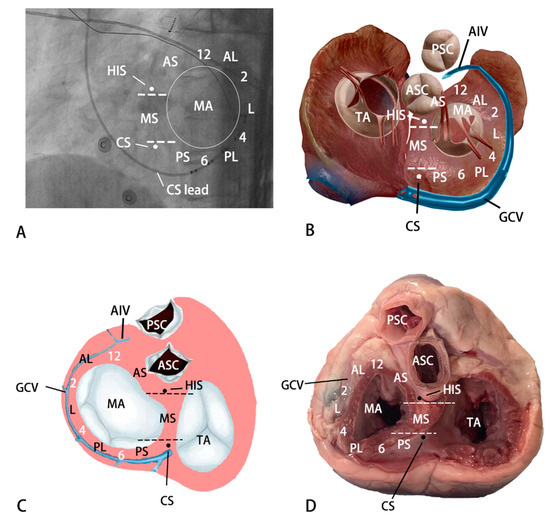
Figure 1
Open AccessReview
Unique Pulmonary Hypertensive Vascular Diseases Associated with Heart and Lung Developmental Defects
J. Cardiovasc. Dev. Dis. 2023, 10(8), 333; https://doi.org/10.3390/jcdd10080333 - 03 Aug 2023
Abstract
Although pediatric pulmonary hypertension (PH) shares features and mechanisms with adult PH, there are also some significant differences between the two conditions. Segmental PH is a unique pediatric subtype of PH with unclear and/or multifactorial pathophysiological mechanisms, and is often associated with complex
[...] Read more.
Although pediatric pulmonary hypertension (PH) shares features and mechanisms with adult PH, there are also some significant differences between the two conditions. Segmental PH is a unique pediatric subtype of PH with unclear and/or multifactorial pathophysiological mechanisms, and is often associated with complex congenital heart disease (CHD), pulmonary atresia with ventricular septal defect, and aortopulmonary collateral arteries. Some cases of complex CHD, associated with a single ventricle after Fontan operation, show pathological changes in the small peripheral pulmonary arteries and pulmonary vascular resistance similar to those observed in pulmonary arterial hypertension (PAH). This condition is termed as the pediatric pulmonary hypertensive vascular disease (PPHVD). Recent advances in genetics have identified the genes responsible for PAH associated with developmental defects of the heart and lungs, such as TBX4 and SOX17. Targeted therapies for PAH have been developed; however, their effects on PH associated with developmental heart and lung defects remain to be established. Real-world data analyses on the anatomy, pathophysiology, genetics, and molecular biology of unique PPHVD cases associated with developmental defects of the heart and lungs, using nationwide and/or international registries, should be conducted in order to improve the treatments and prognosis of patients with these types of pediatric PH.
Full article
(This article belongs to the Special Issue Advances in the Diagnosis and Treatment of Pulmonary Vascular Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
The Perioperative Use of Levosimendan as a Means of Optimizing the Surgical Outcome in Patients with Severe Heart Insufficiency Undergoing Cardiac Surgery
by
, , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 332; https://doi.org/10.3390/jcdd10080332 - 03 Aug 2023
Abstract
►▼
Show Figures
Background: Postoperative myocardial dysfunction following cardiac surgery is a relatively common occurrence. Levosimendan, a calcium sensitizer and inotropic drug, has shown potential in improving outcomes for patients with low preoperative ejection fraction (EF) and myocardial dysfunction after cardiac surgery. This study aims to
[...] Read more.
Background: Postoperative myocardial dysfunction following cardiac surgery is a relatively common occurrence. Levosimendan, a calcium sensitizer and inotropic drug, has shown potential in improving outcomes for patients with low preoperative ejection fraction (EF) and myocardial dysfunction after cardiac surgery. This study aims to evaluate the efficacy of levosimendan in optimizing the surgical outcome for such patients. Methods: A retrospective analysis was conducted on 314 patients with preoperative severe heart failure who underwent cardiac surgery. Among them, 184 patients received perioperative adjunctive therapy with levosimendan, while a comparable group of 130 patients received conventional treatment. Results: The use of levosimendan demonstrated several advantages in postoperative outcomes. It significantly improved short- and long-term survival rates after cardiac surgery, enhanced hemodynamic stability, reduced the requirement for inotropic support, and facilitated faster weaning from ventilator support. Patients who received levosimendan reported reduced angina and dyspnea symptoms, as well as fewer postoperative arrhythmias. Furthermore, levosimendan helped minimize myocardial injury inevitable after cardiac surgery. The levosimendan group also exhibited a notable reduction in hospital readmissions. Conclusions: This study provides evidence of several benefits associated with the perioperative use of levosimendan. However, further prospective randomized studies are warranted to standardize and comprehensively document the other perioperative therapies, in order to validate these findings and establish stronger conclusions.
Full article

Figure 1
Open AccessArticle
Three-Dimensional-Derived Echocardiographic Left Ventricular Structure and Function and Indices from the 12-Lead Electrocardiogram across the Menstrual Cycle in Healthy Physically Active Females: An Exploratory Study
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 331; https://doi.org/10.3390/jcdd10080331 - 03 Aug 2023
Abstract
Background: The impact of the menstrual phases on left ventricular (LV) structure and function using 3D echocardiography and resting electrocardiogram (ECG) in healthy, eumenorrheic, and physically active females has not been investigated. Methods: sixteen females (20 y ± 2) underwent 3D echocardiography
[...] Read more.
Background: The impact of the menstrual phases on left ventricular (LV) structure and function using 3D echocardiography and resting electrocardiogram (ECG) in healthy, eumenorrheic, and physically active females has not been investigated. Methods: sixteen females (20 y ± 2) underwent 3D echocardiography and an ECG at three time points in the menstrual cycle phases (follicular, ovulation, luteal). LV end-diastolic volume (LVEDVi), LV ejection fraction (LVEF), LV mass allometrically indexed to height2.7 (LVMi), torsion, and global longitudinal, circumferential, and radial strain (GLS, GCS, and GRS) were evaluated. ECG data of the P and QRS waves were presented as well as axis deviation, chamber enlargement, and any rhythm abnormalities. Results: LVMi was significantly higher in the luteal phase (36.4 g/m2.7 ± 3.3) compared to the follicular (35.0 g/m2.7 ± 3.7) and ovulation (34.7 g/m2.7 ± 4.3) phases (p = 0.026). There were no differences in other indices of LV structure and function or ECG variables across all phases of the menstrual cycle or evidence of arrhythmia. Conclusions: In physically active females, there is a small but significantly higher LVMi associated with the luteal phase of the menstrual cycle with no concomitant change in LV function or ECG parameters. These findings are important to consider when conducting clinical or research serial assessments.
Full article
(This article belongs to the Special Issue Sports Cardiology in the Modern Era)
►▼
Show Figures

Figure 1
Open AccessArticle
Major Adverse Cardiac and Cerebrovascular Events in Patients Undergoing Simultaneous Heart Surgery and Carotid Endarterectomy
by
, , , , , , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 330; https://doi.org/10.3390/jcdd10080330 - 02 Aug 2023
Abstract
Background. Patients with simultaneous relevant internal carotid artery stenosis and coronary artery heart or valve disease represent a high-risk collective with respect to cerebral or cardiovascular severe events when undergoing surgery. There exist several concepts regarding the timing and modality of carotid revascularization,
[...] Read more.
Background. Patients with simultaneous relevant internal carotid artery stenosis and coronary artery heart or valve disease represent a high-risk collective with respect to cerebral or cardiovascular severe events when undergoing surgery. There exist several concepts regarding the timing and modality of carotid revascularization, which are controversially discussed in patients with heart disease. More data regarding outcome predictors and measures are needed to gain a better understanding of the best treatment option of the discussed patient collective. Methods. This single-center study retrospectively analyzed n = 111 patients undergoing heart surgery with coronary artery bypass grafting or heart-valve surgery and concomitant carotid surgery due to significant internal carotid artery stenosis. In order to do so, patients were divided into two groups with respect to postoperative major adverse cardiac and cerebrovascular events (MACCE) with thirty-day all-cause mortality, valve related mortality, myocardial infarction, stroke and transitory ischemic attack. Results. Preoperative patient’s characteristic in the no-MACCE and MACCE group were mainly balanced, other than higher rates of chronic obstructive pulmonary disease, chronic kidney disease, instable angina pectoris and prior transitory ischemic attack in the MACCE cohort. The analysis of intraoperative characteristics revealed a higher number of intra-aortic balloon pump implantation, which is in line for a higher number of postoperative supports. Besides MACCE, patients suffered significantly more often from postoperative bleeding events and re-thoracotomy, cardiopulmonary reanimation, new onset postoperative dialysis and prolonged intensive care unit stay related complications. Conclusions. Within the reported patient population suffering from MACCE after a simultaneous carotid endarterectomy and heart surgery, a preoperative history of transitory ischemic attack and kidney disease might account for worse outcomes, as severe events were not only neurologically driven but also associated with postoperative cardiovascular complications following heart surgical procedures.
Full article
(This article belongs to the Section Cardiac Surgery)
Open AccessArticle
Lipid-Lowering Treatment and the Lipid Goals Attainment in Patients with a Very High Cardiovascular Risk
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 329; https://doi.org/10.3390/jcdd10080329 - 02 Aug 2023
Abstract
Hypercholesterolemia is the main cardiovascular (CV) risk factor with a large body of evidence. Our aim was to assess the achievement of the main therapeutic goal of Low-Density Lipoprotein Cholesterol (LDL-C) in patients with a very high CV risk and a high-dose statin
[...] Read more.
Hypercholesterolemia is the main cardiovascular (CV) risk factor with a large body of evidence. Our aim was to assess the achievement of the main therapeutic goal of Low-Density Lipoprotein Cholesterol (LDL-C) in patients with a very high CV risk and a high-dose statin therapy. The study group consisted of 1413 consecutive patients hospitalised at the Upper-Silesian Medical Centre in Katowice due to acute myocardial infarction (AMI) treated with atorvastatin ≥ 40 mg or rosuvastatin ≥ 20 mg. The lipid profile was performed on admission and within 12 months after AMI. The main therapeutic goal was defined as LDL-C < 55 mg%. The study group (n = 1413) included 979 males (69.3%) with arterial hypertension (83.3%), diabetes (33.5%), peripheral artery disease (13.6%) and nicotinism (46.2%). In the study group, only 61 patients (4.3%) were additionally taking ezetimibe. During hospitalisation, the primary LDL-C goal was found in only 186 patients (13.2%). Subsequently, a follow-up lipidogram within 12 months was performed in 652 patients (46%), and the therapeutic goal was achieved in 255 patients (39%). There were 258 (18.26%) patients who died within 12 months after myocardial infarction. The lowest mortality rate was found in the subgroup of patients with LDL-C < 55 mg% during follow-up (11.02%). The primary lipid goal attainment among patients with a high-dose statin and a very high CV risk is low and far from the expected rate. Patients hospitalised for AMI should be given a combination of statin and ezetimibe more frequently. Low LDL-C levels measured at follow-up predict a lower risk of death at 12-month follow-up in a large group of patients.
Full article
(This article belongs to the Special Issue Dyslipidemia and Cardiovascular Disease: The Dawn of an Era with New Targets and Novel Therapies)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Longitudinal Trends in Severe Dyslipidemia in the Czech Population: The Czech MONICA and Czech Post-MONICA Study
by
, , , , , , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 328; https://doi.org/10.3390/jcdd10080328 - 31 Jul 2023
Abstract
Background: Severe hypercholesterolemia is associated with an increase in the risk of developing atherosclerotic cardiovascular disease. The aim of this analysis was to assess longitudinal trends in severe dyslipidemia (defined as total cholesterol > 8 mmol/L or LDL-cholesterol > 5 mmol/L) in a
[...] Read more.
Background: Severe hypercholesterolemia is associated with an increase in the risk of developing atherosclerotic cardiovascular disease. The aim of this analysis was to assess longitudinal trends in severe dyslipidemia (defined as total cholesterol > 8 mmol/L or LDL-cholesterol > 5 mmol/L) in a representative population sample of the Czech Republic and to analyze the longitudinal trends in the basic characteristics of individuals with severe dyslipidemia. Methods: Seven independent cross-sectional surveys were organized in the Czech Republic to screen for major cardiovascular risk factors (from 1985 to 2015–2018). A total of 20,443 randomly selected individuals aged 25–64 years were examined. Results: The overall prevalence of severe dyslipidemia was 6.6%, with a significant downward trend from the fifth survey onwards (2000/2001). Over the study period of 30+ years, the individuals with severe dyslipidemia became older, increased in BMI, and did not change their smoking habits. Total cholesterol and non-HDL-cholesterol decreased significantly in both sexes throughout the duration of the study. Conclusions: Despite a significant improvement in lipids in the Czech Republic from 1985, substantially contributing to the decline in cardiovascular mortality, the number of individuals with severe dyslipidemia remained high, and in most cases, they were newly detected during our screening examinations and were thus untreated.
Full article
(This article belongs to the Special Issue Dyslipidemia and Cardiovascular Disease: The Dawn of an Era with New Targets and Novel Therapies)
►▼
Show Figures
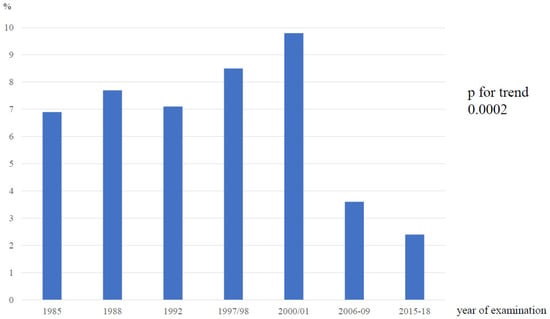
Figure 1
Open AccessReview
Interventions to Address Cardiovascular Risk in Obese Patients: Many Hands Make Light Work
by
, , , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 327; https://doi.org/10.3390/jcdd10080327 - 31 Jul 2023
Abstract
Obesity is a growing public health epidemic worldwide and is implicated in slowing improved life expectancy and increasing cardiovascular (CV) risk; indeed, several obesity-related mechanisms drive structural, functional, humoral, and hemodynamic heart alterations. On the other hand, obesity may indirectly cause CV disease,
[...] Read more.
Obesity is a growing public health epidemic worldwide and is implicated in slowing improved life expectancy and increasing cardiovascular (CV) risk; indeed, several obesity-related mechanisms drive structural, functional, humoral, and hemodynamic heart alterations. On the other hand, obesity may indirectly cause CV disease, mediated through different obesity-associated comorbidities. Diet and physical activity are key points in preventing CV disease and reducing CV risk; however, these strategies alone are not always sufficient, so other approaches, such as pharmacological treatments and bariatric surgery, must support them. Moreover, these strategies are associated with improved CV risk factors and effectively reduce the incidence of death and CV events such as myocardial infarction and stroke; consequently, an individualized care plan with a multidisciplinary approach is recommended. More precisely, this review explores several interventions (diet, physical activity, pharmacological and surgical treatments) to address CV risk in obese patients and emphasizes the importance of adherence to treatments.
Full article
(This article belongs to the Special Issue Cardiovascular Disease: Risk Factors and Prevention)
►▼
Show Figures

Figure 1
Open AccessReview
Minimal-Access Coronary Revascularization: Past, Present, and Future
J. Cardiovasc. Dev. Dis. 2023, 10(8), 326; https://doi.org/10.3390/jcdd10080326 - 31 Jul 2023
Abstract
Minimal-access cardiac surgery appears to be the future. It is increasingly desired by cardiologists and demanded by patients who perceive superiority. Minimal-access coronary artery revascularisation has been increasingly adopted throughout the world. Here, we review the history of minimal-access coronary revascularization and see
[...] Read more.
Minimal-access cardiac surgery appears to be the future. It is increasingly desired by cardiologists and demanded by patients who perceive superiority. Minimal-access coronary artery revascularisation has been increasingly adopted throughout the world. Here, we review the history of minimal-access coronary revascularization and see that it is almost as old as the history of cardiac surgery. Modern minimal-access coronary revascularization takes a variety of forms—namely minimal-access direct coronary artery bypass grafting (MIDCAB), hybrid coronary revascularisation (HCR), and totally endoscopic coronary artery bypass grafting (TECAB). It is noteworthy that there is significant variation in the nomenclature and approaches for minimal-access coronary surgery, and this truly presents a challenge for comparing the different methods. However, these approaches are increasing in frequency, and proponents demonstrate clear advantages for their patients. The challenge that remains, as for all areas of surgery, is demonstrating the superiority of these techniques over tried and tested open techniques, which is very difficult. There is a paucity of randomised controlled trials to help answer this question, and the future of minimal-access coronary revascularisation, to some extent, is dependent on such trials. Thankfully, some are underway, and the results are eagerly anticipated.
Full article
(This article belongs to the Special Issue Minimal Access Cardiac Surgery: State of the Art and Future Perspectives)
►▼
Show Figures

Figure 1
Open AccessReview
Comparative Analysis of Heart Regeneration: Searching for the Key to Heal the Heart—Part I: Experimental Injury Models to Study Cardiac Regeneration
by
, , , and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 325; https://doi.org/10.3390/jcdd10080325 - 31 Jul 2023
Abstract
Cardiovascular diseases are the leading cause of death worldwide, among which, ischemic heart disease is the most prevalent. Myocardial infarction results from occlusion of a coronary artery, which leads to an insufficient blood supply to the myocardium. As is well known, the massive
[...] Read more.
Cardiovascular diseases are the leading cause of death worldwide, among which, ischemic heart disease is the most prevalent. Myocardial infarction results from occlusion of a coronary artery, which leads to an insufficient blood supply to the myocardium. As is well known, the massive loss of cardiomyocytes cannot be solved due the limited regenerative ability of the adult mammalian heart. In contrast, some lower vertebrate species can regenerate the heart after injury; their study has disclosed some of the involved cell types, molecular mechanisms and signaling pathways during the regenerative process. In this two-part review, we discuss the current state of the principal response in heart regeneration, where several involved processes are essential for full cardiac function in recovery.
Full article
(This article belongs to the Special Issue Cardiac Development, Regeneration and Repair)
►▼
Show Figures
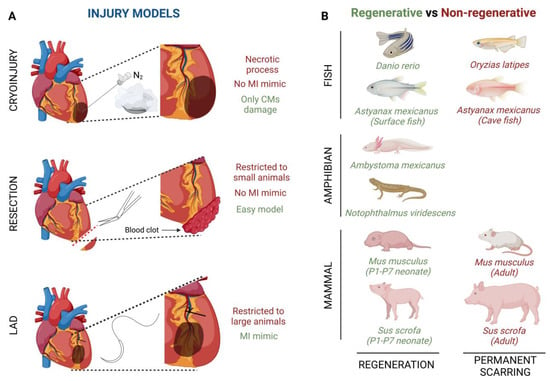
Figure 1
Open AccessCase Report
Plaque Rupture in a Hodgkin Lymphoma Survivor without Cardiovascular Risk Factors 20 Years after Thoracic Radiotherapy: A Case Report
J. Cardiovasc. Dev. Dis. 2023, 10(8), 324; https://doi.org/10.3390/jcdd10080324 - 31 Jul 2023
Abstract
Background: Major improvements in cancer therapies have significantly contributed to increased survival rates of Hodgkin lymphoma (HL) survivors, outweighing cardiovascular side effects and the risks of radiation-induced heart disease. Non-invasive screening for coronary artery disease (CAD) starting five years after irradiation is recommended,
[...] Read more.
Background: Major improvements in cancer therapies have significantly contributed to increased survival rates of Hodgkin lymphoma (HL) survivors, outweighing cardiovascular side effects and the risks of radiation-induced heart disease. Non-invasive screening for coronary artery disease (CAD) starting five years after irradiation is recommended, as plaque development and morphology may differ in this high-risk population. Due to rapid plaque progression and a possibly higher incidence of non-calcified plaques, coronary artery calcium scoring may not be sufficient as a screening modality in HL survivors treated with thoracic radiotherapy. Case summary: A 42-year-old man with a history of HL treated with thoracic radiotherapy presented at the emergency department 20 years after cancer treatment with an ST-elevation myocardial infarction, in the absence of cardiovascular risk factors, for which primary percutaneous coronary intervention of the left anterior descending artery was performed. Four months prior to acute myocardial infarction, invasive coronary angiography only showed wall irregularities. Two years earlier, the Agatston calcium score was zero. Discussion: In HL survivors treated with thoracic radiotherapy, a calcium score of zero may not give the same warranty period for cardiac event-free survival compared to the general population. Coronary computed tomography angiography can be a proper diagnostic tool to detect CAD at an early stage after mediastinal irradiation, as performing calcium scoring may not be sufficient in this population to detect non-calcified plaques, which may show rapid progression and lead to acute coronary syndrome. Also, intensive lipid-lowering therapy should be considered in the presence of atherosclerosis in this patient population.
Full article
(This article belongs to the Special Issue Cardiac Complications and Cardiotoxicity of Radiation Therapy)
►▼
Show Figures

Figure 1
Open AccessReview
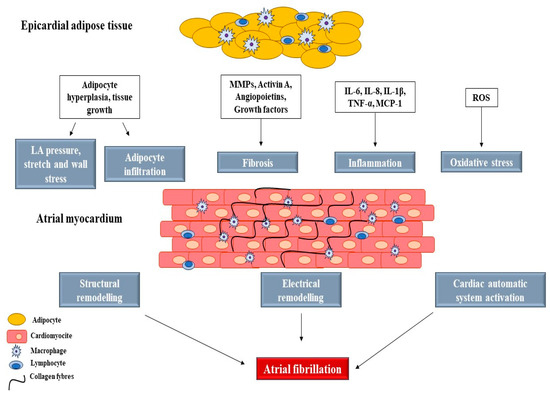
Obesity-Related Atrial Fibrillation: Cardiac Manifestation of a Systemic Disease
by
and
J. Cardiovasc. Dev. Dis. 2023, 10(8), 323; https://doi.org/10.3390/jcdd10080323 - 30 Jul 2023
Abstract
Atrial fibrillation (AF) is the most common arrhythmia worldwide and is associated with increased morbidity and mortality. The mechanisms underlying AF are complex and multifactorial. Although it is well known that obesity is a strong risk factor for AF, the mechanisms underlying obesity-related
[...] Read more.
Atrial fibrillation (AF) is the most common arrhythmia worldwide and is associated with increased morbidity and mortality. The mechanisms underlying AF are complex and multifactorial. Although it is well known that obesity is a strong risk factor for AF, the mechanisms underlying obesity-related AF are not completely understood. Current evidence proposes that in addition to overall hemodynamic changes due to increased body weight, excess adiposity raises systemic inflammation and oxidative stress, which lead to adverse atrial remodeling. This remodeling includes atrial fibrosis, atrial dilation, decreased electrical conduction between atrial myocytes, and altered ionic currents, making atrial tissue more vulnerable to both the initiation and maintenance of AF. However, much remains to be learned about the mechanistic links between obesity and AF. This knowledge will power the development of novel diagnostic tools and treatment options that will help combat the rise of the global AF burden among the obesity epidemic.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, Cancers, Healthcare, JCDD, JCM
New Insights on Chronic Illness: Pathogenesis, Prevalence, Prevention, and Systemic Therapies
Topic Editors: Ram Prasad, Suresh K. VermaDeadline: 31 August 2023
Topic in
Applied Biosciences, Bioengineering, Biomolecules, JCDD, JCM, Micromachines, Reports
Usefulness and Clinical Applications of 3D Printing in Cardiovascular Diseases 2.0
Topic Editors: Zhonghua Sun, Massimo Chessa, Israel Valverde, Alexander Van De BruaeneDeadline: 31 October 2023
Topic in
Biomolecules, Cells, Diseases, IJMS, JMP, Organoids, JCDD
Molecular and Cellular Mechanisms of Diseases: Heart Disease
Topic Editors: Klaus-Dieter Schlüter, Pasi Tavi, Ebru Arioglu-InanDeadline: 24 December 2023
Topic in
Diagnostics, Hearts, JCDD, JCM, JVD
Mechanical Circulatory Support in Heart Failure
Topic Editors: Anton Sabashnikov, Ilija DjordjevicDeadline: 31 December 2023

Conferences
Special Issues
Special Issue in
JCDD
Advances in the Diagnosis and Treatment of Pulmonary Vascular Diseases
Guest Editor: Grzegorz KopecDeadline: 15 August 2023
Special Issue in
JCDD
Cardiovascular Imaging in Heart Failure with Preserved Ejection Fraction
Guest Editor: Daniel A. MorrisDeadline: 31 August 2023
Special Issue in
JCDD
New Pacing Techniques and Non-invasive Methods That May Improve Response and Patient Selection to Cardiac Resynchronization Therapy
Guest Editor: András VereckeiDeadline: 15 September 2023
Special Issue in
JCDD
Heart Failure: Clinical Diagnostics and Treatment
Guest Editors: Evgeny Belyavskiy, Nicolas Merke, Daniel A. MorrisDeadline: 30 September 2023