Journal Description
Geriatrics
Geriatrics
is an international, peer-reviewed, scientific open access journal on geriatric medicine published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, and other databases.
- Journal Rank: CiteScore - Q2 (Health (social science))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 19.6 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the first half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Testimonials: See what our editors and authors say about Geriatrics.
Impact Factor:
2.3 (2022);
5-Year Impact Factor:
2.5 (2022)
Latest Articles
Lessons Learned from Age-Friendly, Team-Based Training
Geriatrics 2023, 8(4), 78; https://doi.org/10.3390/geriatrics8040078 - 28 Jul 2023
Abstract
According to the Institute of Medicine, immediate steps must be taken across the United States to educate and train the healthcare workforce to work collaboratively to address the needs of the growing older adult population. The Geriatric Practice Leadership Institute (GPLI) was designed
[...] Read more.
According to the Institute of Medicine, immediate steps must be taken across the United States to educate and train the healthcare workforce to work collaboratively to address the needs of the growing older adult population. The Geriatric Practice Leadership Institute (GPLI) was designed to support professional teams working in acute and post-acute care in transforming their organization into a designated Age-Friendly Health System. The program was built around the Institute for Healthcare Improvement’s Age-Friendly Health Systems 4Ms framework. This framework focuses on What Matters, Medication, Mentation, and Mobility (the 4Ms) in supporting care for older adults. The GPLI program is an online, seven-month team-based program with four to seven participants from one organization per team. Additionally, each team selected, developed, and completed a quality improvement project based on Age-Friendly Health Systems 4Ms. The curriculum also includes organizational culture, leadership, and interprofessional team-building modules. Using a post-completion survey, the experiences of 41 participants in the GPLI program were assessed. All respondents found the information in the program ‘very’ or ‘extremely’ valuable, and their executive sponsor ‘very’ or ‘extremely’ valuable in supporting their team’s involvement and project. The GPLI program has trained over 200 healthcare professionals and teams that have successfully implemented projects across their organizations.
Full article
(This article belongs to the Special Issue Age-Friendly Ecosystems: Voices from around the World)
Open AccessArticle
An Exploratory Study of Nutrition Knowledge and Challenges Faced by Informal Carers of Community-Dwelling People with Dementia: Online Survey and Thematic Analysis
Geriatrics 2023, 8(4), 77; https://doi.org/10.3390/geriatrics8040077 - 22 Jul 2023
Abstract
►▼
Show Figures
Nutrition knowledge is a primary factor influencing food choices and the ability to identify nutritional risk for carers of people with dementia. Acquiring nutrition knowledge helps carers monitor changes in food intake and micronutrient intake, and whether a healthy and balanced diet is
[...] Read more.
Nutrition knowledge is a primary factor influencing food choices and the ability to identify nutritional risk for carers of people with dementia. Acquiring nutrition knowledge helps carers monitor changes in food intake and micronutrient intake, and whether a healthy and balanced diet is being consumed. This study aimed to assess the nutrition knowledge of carers in the Australian community and their experiences with nutrition education. Using a mixed-methods approach, the nutrition knowledge of informal carers was assessed using the revised General Nutrition Knowledge Questionnaire (AUS-R-NKQ), and interviews of informal carers were used to explore the perspectives in a sub-sample. A total of 57 carers (44 females; mean age of 63.0 ± 13.1) completed the survey, and 11 carers participated in follow-up interviews. The total sample scored 22.9 (±4.57) out of 38 on the AUS-R-NKQ, suggesting basic nutrition knowledge. The interviewed carers acknowledged the importance of healthy nutrition but viewed the provision of a healthy diet for a person with dementia as challenging. In both the survey and interviews, carers reported limited use and availability of dementia-specific nutrition resources. Carers were unsatisfied with the advice and number of referrals provided to improve the nutrition of the person with dementia and desired less confusing nutrition education materials adapted to their level of knowledge. The present study highlights the need for informal carers to be supported to acquire adequate nutrition knowledge.
Full article

Figure 1
Open AccessArticle
The Prevalence of Xerostomia in Older Thai Individuals with Type II Diabetes Mellitus and Its Association with Type of Toothpaste and Oral Functions: A Cross-Sectional Study Using Questionnaires
by
, , , and
Geriatrics 2023, 8(4), 76; https://doi.org/10.3390/geriatrics8040076 - 15 Jul 2023
Abstract
Aim: To investigate the prevalence of xerostomia in older people with diabetes mellitus and its impacts on oral functions, as well as to determine potential risk factors for xerostomia. Methods: An analytical cross-sectional study was conducted on 623 older type 2 diabetes mellitus
[...] Read more.
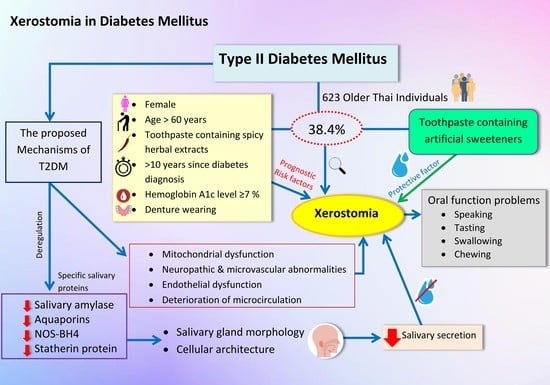
Aim: To investigate the prevalence of xerostomia in older people with diabetes mellitus and its impacts on oral functions, as well as to determine potential risk factors for xerostomia. Methods: An analytical cross-sectional study was conducted on 623 older type 2 diabetes mellitus (T2DM) Thai people using valid structural questionnaires. Patients were interviewed, and data were recorded. Xerostomia was assessed using subjective symptom questionnaires. Risk factors for xerostomia were analyzed using bivariate and multiple logistic regression analyses. Results: Among the study participants, 38.4% of the older T2DM people had xerostomia, which is associated with sex, age, type of toothpaste, years of diabetes, hemoglobin A1c level, other systemic diseases, medication, smoking, alcohol consumption, and denture wearing. It was significant that xerostomia was associated with toothpaste containing spicy herbal extracts (OR: 9.32 [3.46 to 15.25]), while toothpaste containing artificial sweeteners tended to lower the risk of xerostomia. In addition, older T2DM adults with xerostomia had greater impaired oral functions, which include difficulties in speaking (OR: 3.31 [1.11 to 9.80]), tasting (OR: 5.12 [3.26 to 8.06]), swallowing (OR: 3.59 [2.32 to 5.53]), and chewing (OR: 3.34 [1.15 to 5.82]). Conclusions: Xerostomia is prevalent in older Thai people with T2DM. The results suggest that toothpaste containing spicy herbal extracts might increase the risk of xerostomia, resulting in various oral function problems. Therefore, greater awareness of xerostomia in this group should be raised to monitor dental health, and professionals should work in parallel with other aspects of oral health promotion.
Full article
(This article belongs to the Special Issue Health and Disease in Frail Older Individuals: Assessment and Management in Clinical Practice)
►▼
Show Figures
Graphical abstract
Open AccessReview
An Update on Apathy in Alzheimer’s Disease
Geriatrics 2023, 8(4), 75; https://doi.org/10.3390/geriatrics8040075 - 14 Jul 2023
Abstract
Apathy is a complex multi-dimensional syndrome that affects up to 70% of individuals with Alzheimer’s disease (AD). Whilst many frameworks to define apathy in AD exist, most include loss of motivation or goal-directed behaviour as the central feature. Apathy is associated with significant
[...] Read more.
Apathy is a complex multi-dimensional syndrome that affects up to 70% of individuals with Alzheimer’s disease (AD). Whilst many frameworks to define apathy in AD exist, most include loss of motivation or goal-directed behaviour as the central feature. Apathy is associated with significant impact on persons living with AD and their caregivers and is also associated with accelerated cognitive decline across the AD spectrum. Neuroimaging studies have highlighted a key role of fronto-striatial circuitry including the anterior cingulate cortex (ACC), orbito-frontal cortex (OFC) and associated subcortical structures. Importantly, the presence and severity of apathy strongly correlates with AD stage and neuropathological biomarkers of amyloid and tau pathology. Following from neurochemistry studies demonstrating a central role of biogenic amine neurotransmission in apathy syndrome in AD, recent clinical trial data suggest that apathy symptoms may improve following treatment with agents such as methylphenidate—which may have an important role alongside emerging non-pharmacological treatment strategies. Here, we review the diagnostic criteria, rating scales, prevalence, and risk factors for apathy in AD. The underlying neurobiology, neuropsychology and associated neuroimaging findings are reviewed in detail. Finally, we discuss current treatment approaches and strategies aimed at targeting apathy syndrome in AD, highlighting areas for future research and clinical trials in patient cohorts.
Full article
(This article belongs to the Section Geriatric Neurology)
►▼
Show Figures
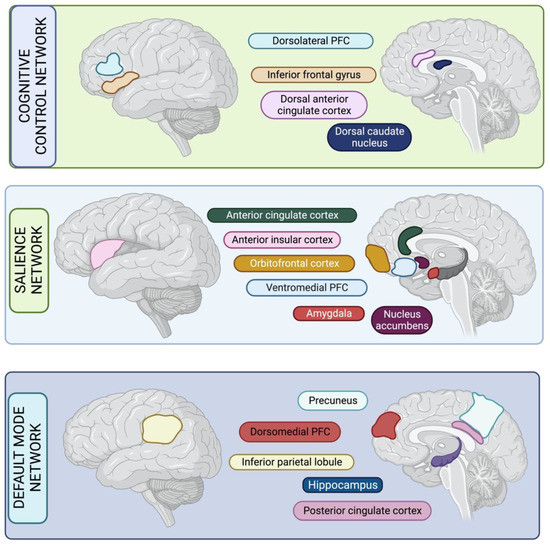
Figure 1
Open AccessArticle
Guiding Post-Hospital Recovery by ‘What Matters:’ Implementation of Patient Priorities Identification in a VA Community Living Center
by
, , , , , and
Geriatrics 2023, 8(4), 74; https://doi.org/10.3390/geriatrics8040074 - 04 Jul 2023
Abstract
Background: Patient priorities care (PPC) is an effective age-friendly health systems (AFHS) approach to aligning care with goals derived from ‘what matters’. The purpose of this quality improvement program was to evaluate the fidelity and feasibility of the health priorities identification (HPI) process
[...] Read more.
Background: Patient priorities care (PPC) is an effective age-friendly health systems (AFHS) approach to aligning care with goals derived from ‘what matters’. The purpose of this quality improvement program was to evaluate the fidelity and feasibility of the health priorities identification (HPI) process in VA Community Living Centers (CLC). Methods: PPC experts worked with local CLC staff to guide the integration of HPI into the CLC and utilized a Plan–Do–Study–Act (PDSA) model for this quality improvement project. PPC experts reviewed health priorities identification (HPI) encounters and interdisciplinary team (IDT) meetings for fidelity to the HPI process of PPC. Qualitative interviews with local CLC staff determined the appropriateness of the health priorities identification process in the CLC. Results: Over 8 months, nine facilitators completed twenty HPI encounters. Development of a Patient Health Priorities note template, staff education and PPC facilitator training improved fidelity and documentation of HPI encounters in the electronic health record. Facilitator interviews suggested that PPC is appropriate in this setting, not burdensome to staff and fostered a person-centered approach to AFHS. Conclusions: The HPI process is an acceptable and feasible approach to ask the ‘what matters’ component of AFHS in a CLC setting.
Full article
(This article belongs to the Special Issue Age-Friendly Ecosystems: Voices from around the World)
►▼
Show Figures

Figure 1
Open AccessArticle
Can Cardiometabolic Risk Be Reduced in the Elderly? Comprehensive Epidemiological Study
Geriatrics 2023, 8(4), 73; https://doi.org/10.3390/geriatrics8040073 - 01 Jul 2023
Abstract
►▼
Show Figures
Through these epidemiological studies, which are based on statistical and observational calculations, without visual appeal, we tracked the incidence of public health problems. In this study, our research objective was to determine and evaluate the health patterns present in a population, along with
[...] Read more.
Through these epidemiological studies, which are based on statistical and observational calculations, without visual appeal, we tracked the incidence of public health problems. In this study, our research objective was to determine and evaluate the health patterns present in a population, along with identifying the factors that contribute to the risks or provide protection against specific diseases or conditions. The progression of cardiometabolic diseases is closely linked to various chronic conditions, such as diabetes, hypertension, dyslipidemia, and chronic kidney disease. This research study involved 578 patients, who were divided into six-year cohorts ranging from 2017 to 2022. The study examined parameters related to cardiometabolic diseases, including alcoholic hepatopathies, non-alcoholic hepatopathy, chronic kidney disease, hypertension, myocardial infarction, other forms of chronic coronary syndrome, peripheral vascular disease, microvascular diseases, macrovascular diseases, and hypercholesterolemia, while considering age and physical activity levels. The study concluded that individuals in the age group of 41–50 years exhibited the highest propensity for cardiometabolic damage. Additionally, the promotion of a healthy and active lifestyle is increasingly gaining traction among elderly patients.
Full article
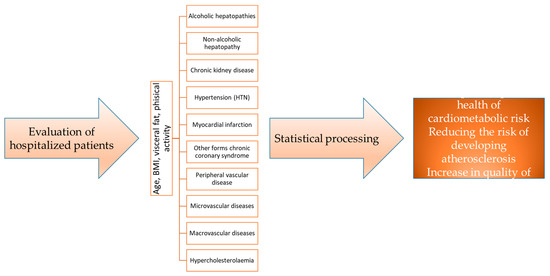
Figure 1
Open AccessArticle
Impact of COVID-19 Pandemic on Fragility Fractures of the Hip: An Interrupted Time-Series Analysis of the Lockdown Periods in Western Greece and Review of the Literature
by
, , , , , , and
Geriatrics 2023, 8(4), 72; https://doi.org/10.3390/geriatrics8040072 - 01 Jul 2023
Abstract
Since December 2019, the COVID-19 pandemic has had a significant impact on healthcare systems worldwide, prompting policymakers to implement measures of isolation and eventually adopt strict national lockdowns, which affected mobility, healthcare-seeking behavior, and services, in an unprecedented manner. This study aimed to
[...] Read more.
Since December 2019, the COVID-19 pandemic has had a significant impact on healthcare systems worldwide, prompting policymakers to implement measures of isolation and eventually adopt strict national lockdowns, which affected mobility, healthcare-seeking behavior, and services, in an unprecedented manner. This study aimed to analyze the effects of these lockdowns on hip-fracture epidemiology and care services, compared to nonpandemic periods in previous years. We retrospectively collected data from electronic patient records of two major hospitals in Western Greece and included patients who suffered a fragility hip fracture and were admitted during the two 5-week lockdown periods in 2020, compared to time-matched patients from 2017–2019. The results showed a drop in hip-fracture incidence, which varied among hospitals and lockdown periods, and conflicting impacts on time to surgery, time to discharge after surgery, and total hospitalization time. The study also found that differences between the two differently organized units were exaggerated during the COVID-19 lockdown periods, highlighting the impact of compliance with social-distancing measures and the reallocation of resources on the quality of healthcare services. Further research is needed to fully understand the specific variations and patterns of geriatric hip-fracture care during emergency health crises characterized by limited resources and behavioral changes.
Full article
(This article belongs to the Collection Frailty in Older Adults)
►▼
Show Figures
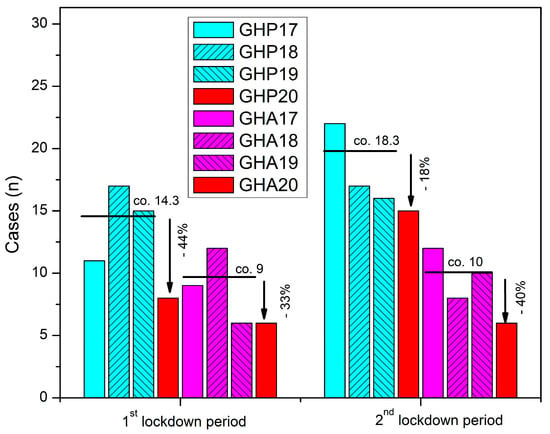
Figure 1
Open AccessBrief Report
Socio-Demographic, Lifestyle, and Clinical Characteristics of Early and Later Weight Status in Older Adults: Secondary Analysis of the ASPREE Trial and ALSOP Sub-Study
by
, , , , , , and
Geriatrics 2023, 8(4), 71; https://doi.org/10.3390/geriatrics8040071 - 29 Jun 2023
Abstract
Objective: To identify the socio-demographic, lifestyle, and clinical characteristics associated with self-reported weight status in early (age 18 years) and late (age ≥ 70 years) adulthood. Methods: The number of participants was 11,288, who were relatively healthy community-dwelling Australian adults aged ≥70 years
[...] Read more.
Objective: To identify the socio-demographic, lifestyle, and clinical characteristics associated with self-reported weight status in early (age 18 years) and late (age ≥ 70 years) adulthood. Methods: The number of participants was 11,288, who were relatively healthy community-dwelling Australian adults aged ≥70 years (mean age 75.1 ± 4.2 years) in the Aspirin in Reducing Events in the Elderly (ASPREE) Longitudinal Study of Older Persons (ALSOP) sub-study. Self-reported weight at the study baseline (age ≥ 70 years) and recalled weight at age 18 years were collected. Height measured at baseline was used to calculate the BMI at both time points. Individuals were categorised into one of five ‘lifetime’ weight status groups: healthy weight (at both age 18 year and ≥70 years), overweight (at either or both times), non-obese (age 18 year) to obesity (age ≥70 years), obesity (age 18 years) to non-obese (age ≥ 70 years), and early and later life obesity (at age 18 years and ≥70 years). Results: Participants who experienced obesity in early and/or late adulthood were at a higher risk of adverse clinical characteristics. Obesity in late adulthood (regardless of early adulthood weight status) was associated with high proportions of hypertension, diabetes, and dyslipidaemia, whereas obesity in early adulthood (regardless of late adulthood weight status) was associated with lower cognitive scores (on all four measures). Discussion/Conclusion: Healthy or overweight weight status in early and later adulthood was associated with more favourable socioeconomic, lifestyle, and clinical measures. Obesity in early adulthood was associated with lower cognitive function in later adulthood, whereas obesity in later adulthood was associated with hypertension, diabetes, and dyslipidaemia.
Full article
(This article belongs to the Special Issue Depressive Symptoms, Cognitive Functioning, Frailty, Multimorbidity and Loneliness among Older Population: An Update)
Open AccessBrief Report
Integrating 4Ms Assessment through Medicare Annual Wellness Visits: Comparison of Quality Improvement Strategies in Primary Care Clinics
by
, , , , and
Geriatrics 2023, 8(4), 70; https://doi.org/10.3390/geriatrics8040070 - 28 Jun 2023
Abstract
The Medicare Annual Wellness Visit (AWV), which includes comprehensive preventative assessments and screenings, is associated with improved preventative services, including vaccination and cancer screenings. However, the AWV alone does not promote whole-person care. Integrating the AWV within an Age-Friendly Health System (AFHS) contextualizes
[...] Read more.
The Medicare Annual Wellness Visit (AWV), which includes comprehensive preventative assessments and screenings, is associated with improved preventative services, including vaccination and cancer screenings. However, the AWV alone does not promote whole-person care. Integrating the AWV within an Age-Friendly Health System (AFHS) contextualizes AWV services within a comprehensive geriatric care framework that integrates the “4Ms” (mentation, medication, mobility, and what matters). This study describes and evaluates quality improvement initiatives to improve the completion of AWV within two different AFHS-recognized health systems (an academic university clinic and a Federally Qualified Health Center). The results from this evaluation present opportunities that other health systems can consider for leveraging electronic health records (EHRs) and enabling services to complete AWVs within a 4Ms framework. The implementation results also suggest an adaptation of the 4Ms assessment schedule for patients with complex chronic conditions who may suffer from multiple comorbidities and cognitive impairment.
Full article
(This article belongs to the Section Healthy Aging)
►▼
Show Figures
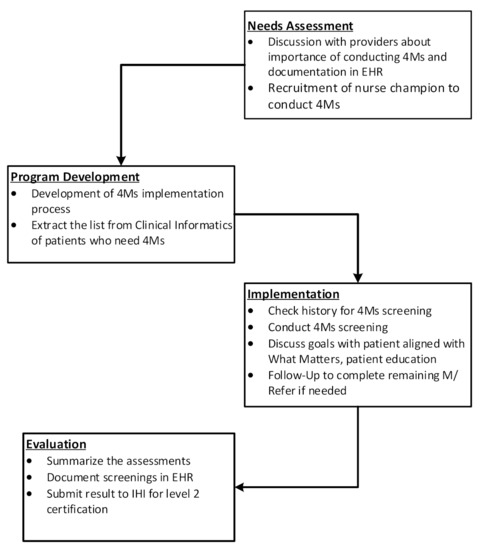
Figure 1
Open AccessArticle
A National Study of Marital Status Differences in Early Uptake of COVID-19 Vaccine among Older Americans
Geriatrics 2023, 8(4), 69; https://doi.org/10.3390/geriatrics8040069 - 28 Jun 2023
Abstract
We provide one of the first nationally representative studies to examine COVID-19 vaccine uptake differences by marital status within the first year after the vaccine was recommended among older Americans. Data were drawn from the National Health and Aging Trends Study (2021). The
[...] Read more.
We provide one of the first nationally representative studies to examine COVID-19 vaccine uptake differences by marital status within the first year after the vaccine was recommended among older Americans. Data were drawn from the National Health and Aging Trends Study (2021). The study sample included 3180 participants aged 65 and older with 1846 women and 1334 men. Results from logistic regression models suggest that divorced/separated older adults were less likely to receive at least one dose of the COVID-19 vaccine in 2021 than their married counterparts, especially among women and individuals with higher education. Widowed and never married respondents were generally not significantly different from married respondents in COVID-19 vaccination status, with only one exception: less-educated never-married respondents were more likely to receive COVID-19 vaccination than their less-educated married counterparts. Our study highlights divorce/separation as a significant social factor associated with COVID-19 vaccine uptake among older adults in the U.S. These findings suggest that divorced/separated older adults are the most vulnerable population segment at risk of low COVID-19 vaccine uptake. Future efforts to improve vaccine equity and uptake should target this group specifically, with tailored interventions to increase their access and uptake of the vaccine.
Full article
(This article belongs to the Section Healthy Aging)
►▼
Show Figures

Figure 1
Open AccessPerspective
Age-Friendly Ecosystems: Expert Voices from the Field
Geriatrics 2023, 8(4), 68; https://doi.org/10.3390/geriatrics8040068 - 21 Jun 2023
Cited by 1
Abstract
(1) Background: With the growth of the age-friendly movement, age-friendly ecosystems (AFE) garnered more attention. The successful development of an AFE is contingent on unified efforts across different stakeholders; however, limited efforts were made to help create a common understanding of the necessary
[...] Read more.
(1) Background: With the growth of the age-friendly movement, age-friendly ecosystems (AFE) garnered more attention. The successful development of an AFE is contingent on unified efforts across different stakeholders; however, limited efforts were made to help create a common understanding of the necessary components of an AFE. (2) Methodology: In response, The John A. Hartford Foundation and The Age-Friendly Institute hosted a series of convenings of international experts to identify a working definition of the characteristics composing an AFE. The goal of these convenings was to provide a foundation on which to unite cross-sector age-friendly work. (3) Results: This paper discussed the findings of the convenings and provided a framework from which future age-friendly work must draw upon. (4) Conclusions: This paper presented a necessary change in how we conceive AFEs.
Full article
(This article belongs to the Special Issue Age-Friendly Ecosystems: Voices from around the World)
►▼
Show Figures
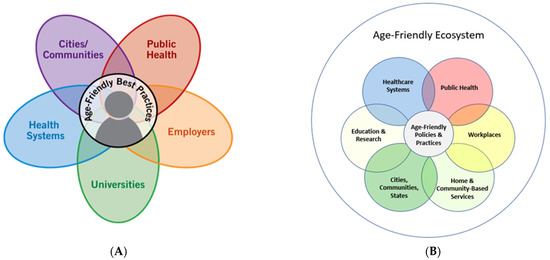
Figure 1
Open AccessBrief Report
Predictors of Nursing Home Entry within 36 Months after Hospitalization via the Emergency Department among Persons Aged 75 Years or Older
Geriatrics 2023, 8(3), 67; https://doi.org/10.3390/geriatrics8030067 - 15 Jun 2023
Abstract
►▼
Show Figures
Objective: We aimed to identify risk factors for nursing home (NH) entry 36 months after hospitalization via the emergency department (ED) in a population of patients aged 75 years or older. Methods: This was a prospective multicentre cohort. Patients were recruited from the
[...] Read more.
Objective: We aimed to identify risk factors for nursing home (NH) entry 36 months after hospitalization via the emergency department (ED) in a population of patients aged 75 years or older. Methods: This was a prospective multicentre cohort. Patients were recruited from the emergency departments (EDs) of nine hospitals. Subjects had been hospitalised in a medical ward in the same hospital as the ED to which they were initially admitted. Subjects who experienced NH entry prior to ED admission were excluded. NH entry has been defined as the incident admission either into an NH or other long-term care facility within the follow-up period. Variables from a comprehensive geriatric assessment of patients were entered into a Cox model with competing risks to predict NH entry during 3 years of follow-up. Results: Among 1306 patients included in the SAFES cohort, 218 (16.7%) who were already in an NH were excluded. The remaining 1088 patients included in the analysis were aged 84 ± 6 years on average. During 3 years of follow-up, 340 (31.3%) entered an NH. The independent risk factors for NH entry were that they: living alone (Hazard ratio (HR) 2.00, had a 95% confidence interval (CI) 1.59–2.54, p < 0.0001), could not independently perform activities of daily living (HR 1.81, 95% CI 1.24–2.64, p = 0.002), and had balance disorders (HR 1.37, 95% CI 1.09–1.73, p = 0.007), dementia syndrome (HR 1.80, 95% CI 1.42–2.29, p < 0.0001) and a risk of pressure ulcers (HR 1.42, 95% CI 1.10–1.82, p = 0.006). Conclusion: The majority of the risk factors for NH entry within 3 years after emergency hospitalization are amenable to intervention strategies. It is therefore reasonable to imagine that targeting these features of frailty could delay or prevent NH entry and improve the quality of life of these individuals before and after NH entry.
Full article
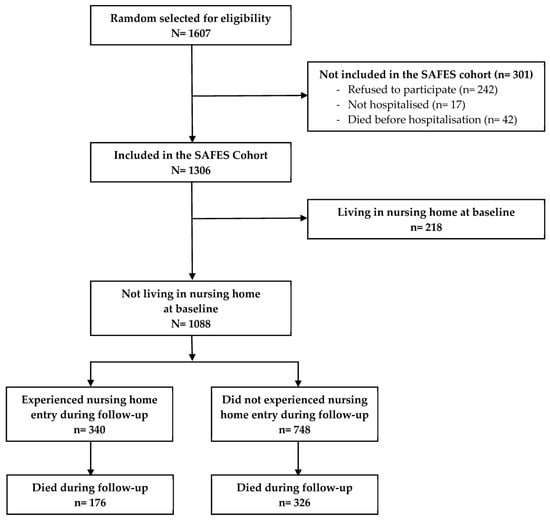
Figure 1
Open AccessArticle
Morbidity and Mortality Analysis in the Treatment of Intertrochanteric Hip Fracture with Two Fixation Systems: Dynamic Hip Screw (DHS) or Trochanteric Fixation Nail Advance (TFNA)
by
, , , , and
Geriatrics 2023, 8(3), 66; https://doi.org/10.3390/geriatrics8030066 - 08 Jun 2023
Abstract
Background: The aim of this study was to compare the clinical outcomes, complications, and mortality of patients with intertrochanteric hip fracture treated with dynamic hip screw (DHS) vs. trochanteric fixation nail advance (TFNA). Methods: We evaluated 152 patients with intertrochanteric fractures concerning age,
[...] Read more.
Background: The aim of this study was to compare the clinical outcomes, complications, and mortality of patients with intertrochanteric hip fracture treated with dynamic hip screw (DHS) vs. trochanteric fixation nail advance (TFNA). Methods: We evaluated 152 patients with intertrochanteric fractures concerning age, sex, comorbidity, Charlson Index, preoperative gait, OTA/AO classification, time from fracture to surgery, blood loss, amount of blood replacement, changes in gait, full weight-bearing at hospital discharge, complications, and mortality. The final indicators encompassed the adverse effects linked to implants, postoperative complications, clinical healing or bone healing duration, and functional score. Results: The study included a total of 152 patients, out of which 78 (51%) received DHS treatment and 74 (49%) received TFNA treatment. The results of this study show that the TFNA group demonstrated superiority (p < 0.001). However, it should be noted that the TFNA group had a higher frequency of the most unstable fractures (AO 31 A3, p < 0.005). Full weight-bearing at discharge also decreased in patients with more unstable fractures (p = 0.005) and severe dementia (p = 0.027). Mortality was higher in the DHS group; however, a longer time from diagnosis to surgery was also observed in this group (p < 0.005). Conclusions: The TFNA group has shown a higher success rate in achieving full weight-bearing at hospital discharge when treating trochanteric hip fractures. This makes it the preferred choice for treating unstable fractures in this region of the hip. Additionally, it is important to note that a longer time to surgery is associated with increased mortality in patients with hip fractures.
Full article
Open AccessFeature PaperArticle
The Institutionalisation of Brazilian Older Abused Adults: A Qualitative Study among Victims and Formal Carers
by
, , , , , , and
Geriatrics 2023, 8(3), 65; https://doi.org/10.3390/geriatrics8030065 - 06 Jun 2023
Abstract
Abuse against elders is acknowledged as a severe and pervasive problem in society. If support services are not tailored to the victims’ knowledge or perceived needs, the intervention is likely to be unsuccessful. This study aimed to explore the experience of institutionalisation of
[...] Read more.
Abuse against elders is acknowledged as a severe and pervasive problem in society. If support services are not tailored to the victims’ knowledge or perceived needs, the intervention is likely to be unsuccessful. This study aimed to explore the experience of institutionalisation of abused older people from the perspective of the victims and their formal carers in a Brazilian social shelter. A qualitative descriptive study was performed with 18 participants, including formal carers and older abused persons admitted to a long-term care institution in the south of Brazil. Qualitative thematic analysis was used to analyse the transcripts of semi-structured qualitative interviews. Three themes were identified: (1) personal, relational, and social bonds: broken or weakened; (2) denial of the violence suffered; and (3) from imposed protection to compassionate care. Our findings provide insights for effective prevention and intervention measures in elder abuse. From a socio-ecological standpoint, vulnerability and abuse might be averted at the community and societal levels (e.g., education and awareness of elder abuse) by creating a minimum standard for the care of older individuals (e.g., law or economic incentives). Further study is needed to facilitate recognition and raise awareness among individuals in need and those offering assistance and support.
Full article
(This article belongs to the Collection Ageism, the Black Sheep of the Decade of Healthy Ageing)
►▼
Show Figures
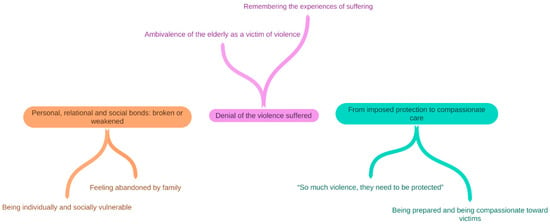
Figure 1
Open AccessArticle
Contribution of Different Brain Disorders and Multimorbidity to Delirium Superimposed Dementia (DSD)
by
and
Tilman Wetterling
Geriatrics 2023, 8(3), 64; https://doi.org/10.3390/geriatrics8030064 - 02 Jun 2023
Abstract
►▼
Show Figures
Delirium, an acute neuropsychiatric disorder characterized by a disturbance of attention and awareness, is often superimposed on dementia with its progressive cognitive decline. Despite the high frequency and clinical relevance of this condition, often called delirium-superimposed dementia (DSD), little is known about possible
[...] Read more.
Delirium, an acute neuropsychiatric disorder characterized by a disturbance of attention and awareness, is often superimposed on dementia with its progressive cognitive decline. Despite the high frequency and clinical relevance of this condition, often called delirium-superimposed dementia (DSD), little is known about possible triggers. In this study using the GePsy-B databank, we investigated the impact of the underlying brain disorder and multimorbidity (MM) on DSD. MM was measured by CIRS and the number of ICD-10 diagnoses. Dementia was diagnosed by CDR, and delirium by DSM IV TR criteria. A total of 218 patients were diagnosed with DSD and these were compared to 105 patients with only dementia, 46 with only delirium, and 197 patients suffering from other psychiatric diseases, mainly depression. No significant differences between groups were found concerning CIRS scores. Based on CT scans, DSD cases were grouped into those with cerebral atrophy only (probably pure neurodegenerative), with brain infarction, or with white matter hyperintensities (WMH), but no between-group differences regarding the MM indices could be found. Regression analysis only revealed age and dementia stage as influencing factors. Conclusion: Our results suggest that neither MM nor morphologic changes in the brain are predisposing factors for DSD.
Full article
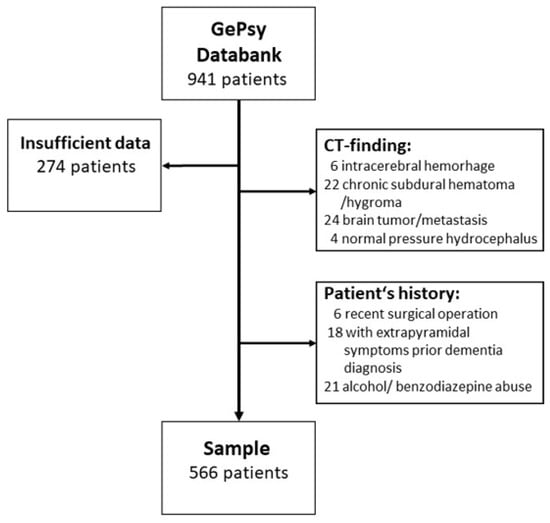
Figure 1
Open AccessCommentary
The Value of Age-Friendly Public Health Systems in the Age-Friendly Ecosystem
by
and
Geriatrics 2023, 8(3), 63; https://doi.org/10.3390/geriatrics8030063 - 02 Jun 2023
Abstract
The United States population is living longer and healthier than ever. This enables our communities—and our society—to continue to benefit from our knowledge, experience, and energy as we age. The public health system is foundational for increasing life expectancy, and now it has
[...] Read more.
The United States population is living longer and healthier than ever. This enables our communities—and our society—to continue to benefit from our knowledge, experience, and energy as we age. The public health system is foundational for increasing life expectancy, and now it has the opportunity to further support older adult health and well-being. Trust for America’s Health (TFAH), in partnership with The John A. Hartford Foundation, launched the age-friendly public health systems initiative in 2017 with the goal of raising awareness within the public health sector of its many potential roles in healthy aging. TFAH has worked with state and local departments of health to build capacity and expertise in older adult health and has provided guidance and technical assistance to expand this work across the U.S. TFAH now envisions a public health system that has healthy aging as a core function. This paper aims to describe why the public health sector should adopt healthy aging policies and practices, how this is being operationalized at the state and local levels, and the value of age-friendly public health systems within the age-friendly ecosystem.
Full article
(This article belongs to the Special Issue Age-Friendly Ecosystems: Voices from around the World)
►▼
Show Figures

Figure 1
Open AccessArticle
Impact of Medical Specialties on Diagnostic and Therapeutic Management of Elderly Cancer Patients
by
, , , , , and
Geriatrics 2023, 8(3), 62; https://doi.org/10.3390/geriatrics8030062 - 01 Jun 2023
Abstract
►▼
Show Figures
The management (diagnostic and therapeutic) of cancer in the geriatric population involves a number of complex difficulties. The aim of this study was to assess the impact of a medical specialty on the diagnostic and therapeutic management of elderly cancer patients. Four clinical
[...] Read more.
The management (diagnostic and therapeutic) of cancer in the geriatric population involves a number of complex difficulties. The aim of this study was to assess the impact of a medical specialty on the diagnostic and therapeutic management of elderly cancer patients. Four clinical scenarios of cancer in the geriatric population, with a dedicated survey to gather information regarding each clinical case’s diagnostic and therapeutic approaches, as well as the different criteria influencing physicians’ therapeutic decisions, were exposed to geriatricians, oncologists, and radiotherapists in Saint-Etienne. The surveys were filled out by 13 geriatricians, 11 oncologists, and 7 radiotherapists. There was a homogeneity of responses regarding the confirmation of cancer diagnostics in the elderly. There were strong disparities (inter- and intra-specialties) for several clinical situations regarding the therapeutic management of cancer. There were significant disparities in terms of surgical management, the implementation of a chemotherapy protocol, and the adaptation of the chemotherapy dosage. Contrary to oncologists, who primarily consider the G8 and the Karnofsky score, geriatric autonomy scores and frailty with cognitive assessment were the key factors determining diagnostic/therapeutic therapy for geriatricians. These results raise important ethical questions, requiring specific studies in geriatric populations to provide the homogenous management of elderly patients with cancer.
Full article
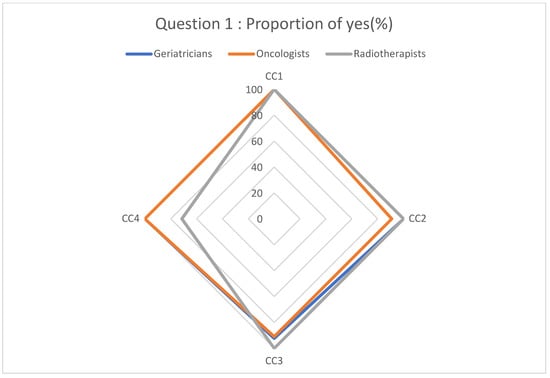
Figure 1
Open AccessArticle
Associations between Physical Activity and Health-Related Quality of Life among Community-Dwelling Older Adults: A Cross-Sectional Study in Urban Greece
by
, , , , , , , , , and
Geriatrics 2023, 8(3), 61; https://doi.org/10.3390/geriatrics8030061 - 01 Jun 2023
Abstract
Physical activity is an important factor in achieving healthy aging, offering older persons multiple benefits in terms of maintaining and improving their health and wellbeing. The aim of this study was to investigate the effect of physical activity on the quality of life
[...] Read more.
Physical activity is an important factor in achieving healthy aging, offering older persons multiple benefits in terms of maintaining and improving their health and wellbeing. The aim of this study was to investigate the effect of physical activity on the quality of life of older adults. A cross-sectional study was conducted from February to May 2022, using the Short-Form Health Survey (SF-36) and the International Physical Activity Questionnaire (IPAQ). A total of 124 people aged 65 and over participated in the survey. The average age of the participants was 71.6 years, and 62.1% were women. Participants showed a moderate quality of life with regard to the physical health dimension (mean score 52.4) and a higher quality of life with regard to the mental health dimension (mean score 63.1) compared to the expected values of the population. Low levels of physical activity were recorded among older adults, reaching a rate of 83.9%. A moderate or high level of physical activity has been found to contribute to a better physical functioning (p = 0.03), vitality (p = 0.02) and general health (p = 0.01). Finally, comorbidity had a negative impact on physical activity (p = 0.03) and quality of life regarding mental and physical health in older adults. The study showed very low levels of physical activity in older Greek adults. The management of this problem, which was intensified during the COVID-19 pandemic, should be a high priority in public health programs focusing on healthy aging, as physical activity affects and promotes many of the basic aspects of quality of life.
Full article
(This article belongs to the Special Issue Physical and Cognitive Decline in Older Adults)
►▼
Show Figures
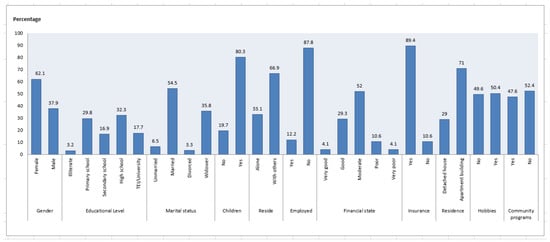
Figure 1
Open AccessArticle
Prediction of In-Hospital Falls Using NRS, PACD Score and FallRS: A Retrospective Cohort Study
by
, , , , , and
Geriatrics 2023, 8(3), 60; https://doi.org/10.3390/geriatrics8030060 - 01 Jun 2023
Abstract
►▼
Show Figures
Background: Harmful in-hospital falls with subsequent injuries often cause longer stays and subsequently higher costs. Early identification of fall risk may help in establishing preventive strategies. Objective: To assess the predictive ability of different clinical scores including the Post-acute care discharge (PACD) score
[...] Read more.
Background: Harmful in-hospital falls with subsequent injuries often cause longer stays and subsequently higher costs. Early identification of fall risk may help in establishing preventive strategies. Objective: To assess the predictive ability of different clinical scores including the Post-acute care discharge (PACD) score and nutritional risk screening score (NRS), and to develop a new fall risk score (FallRS). Methods: A retrospective cohort study of medical in-patients of a Swiss tertiary care hospital from January 2016 to March 2022. We tested the ability of the PACD score, NRS and FallRS to predict a fall by using the area under curve (AUC). Adult patients with a length of stay of ≥ 2 days were eligible. Results: We included 19,270 admissions (43% females; median age, 71) of which 528 admissions (2.74%) had at least one fall during the hospital stay. The AUC varied between 0.61 (95% confidence interval (CI), 0.55–0.66) for the NRS and 0.69 (95% CI, 0.64–0.75) for the PACD score. The combined FallRS score had a slightly better AUC of 0.70 (95% CI, 0.65–0.75) but was more laborious to compute than the two other scores. At a cutoff of 13 points, the FallRS had a specificity of 77% and a sensitivity of 49% in predicting falls. Conclusions: We found that the scores focusing on different aspects of clinical care predicted the risk of falls with fair accuracy. A reliable score with which to predict falls could help in establishing preventive strategies for reducing in-hospital falls. Whether or not the scores presented have better predictive ability than more specific fall scores do will need to be validated in a prospective study.
Full article
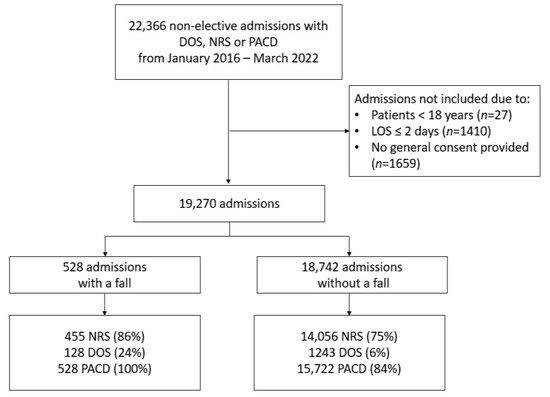
Figure 1
Open AccessEditorial
Intermediate Care in Italy: Addressing the Challenges and Opportunities for Person-Tailored Care
Geriatrics 2023, 8(3), 59; https://doi.org/10.3390/geriatrics8030059 - 30 May 2023
Abstract
The concept of intermediate care is gaining increasing recognition in Italy as a critical strategy for improving quality of care and promoting the integration of healthcare services across different settings. This is driven by demographic changes and the growing prevalence of chronic conditions.
[...] Read more.
The concept of intermediate care is gaining increasing recognition in Italy as a critical strategy for improving quality of care and promoting the integration of healthcare services across different settings. This is driven by demographic changes and the growing prevalence of chronic conditions. One of the key challenges in delivering intermediate care in Italy is ensuring that care is person-tailored, which requires a shift towards a more holistic approach that prioritizes individual preferences and values. This requires greater collaboration and communication across different healthcare settings and a coordinated approach to the delivery of care that promotes innovation and the use of technology to support remote monitoring and care delivery. Despite these challenges, intermediate care offers significant opportunities with which to enhance the quality of care, reduce healthcare costs, and promote social cohesion as well as community engagement. Overall, a coordinated and comprehensive approach is required to address the challenges and opportunities associated with intermediate care and to deliver person-tailored care that improves health outcomes as well as sustainability in Italy.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cancers, Diseases, Geriatrics, Healthcare, Women
Women's Health and Aging
Topic Editors: Li Yang, Rosa Legood, Fei MaDeadline: 25 September 2023
Topic in
Biomedicines, Brain Sciences, Geriatrics, Life, Neurology International
Translational Advances in Neurodegenerative Dementias
Topic Editors: Francesco Di Lorenzo, Annibale AntonioniDeadline: 31 December 2023
Topic in
Biology, Geriatrics, Healthcare, IJMS, JCM, Life, Nutrients
Preventing and Managing Sarcopenia in Older Adults through Physical Activity, Exercise and Nutrition Interventions and Approaches
Topic Editors: Theocharis Ispoglou, Matthew Lees, James McKennaDeadline: 31 January 2024
Topic in
JCM, Healthcare, Diseases, Geriatrics
Clinical Features and Intervention of Patients with Chronic Non-Oncologic Pain
Topic Editors: Ferran Cuenca-Martínez, Josué Fernández-CarneroDeadline: 20 March 2024

Conferences
Special Issues
Special Issue in
Geriatrics
Animal Models for the Research of Alzheimer's Disease and Neurodegeneration
Guest Editors: Dongming Cai, Mariana Lemos DuarteDeadline: 16 August 2023
Special Issue in
Geriatrics
Hypertension in Older Adults
Guest Editor: Pasquale MoneDeadline: 30 September 2023
Special Issue in
Geriatrics
Physical and Cognitive Decline in Older Adults
Guest Editors: Madhuchhanda Mohanty, Prakash KumarDeadline: 15 October 2023
Special Issue in
Geriatrics
Emotional and Cognitive Problems in Older Patients with Cancer
Guest Editors: Philip R. Debruyne, Patricia SchofieldDeadline: 31 October 2023
Topical Collections
Topical Collection in
Geriatrics
Joint Arthroplasty in the Oldest People
Collection Editors: Juan F. Blanco, Carmen da Casa
Topical Collection in
Geriatrics
Ageism, the Black Sheep of the Decade of Healthy Ageing
Collection Editor: Lydia Gimenez Llort
Topical Collection in
Geriatrics
Responding to the Pandemic: Geriatric Care Models
Collection Editor: James Powers













