Journal Description
Audiology Research
Audiology Research
is an international, scientific, peer-reviewed, open access journal on audiology and neurotology, published bimonthly online by MDPI (from Volume 10, Issue 2 - 2020). The Italian Society of Vestibology (VIS) is affiliated with Audiology Research and its members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 23.6 days after submission; acceptance to publication is undertaken in 3.6 days (median values for papers published in this journal in the first half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.7 (2022);
5-Year Impact Factor:
1.6 (2022)
Latest Articles
Hearing Aid in Vestibular-Schwannoma-Related Hearing Loss: A Review
Audiol. Res. 2023, 13(4), 627-635; https://doi.org/10.3390/audiolres13040054 - 08 Aug 2023
Abstract
(1) Background: Several types of hearing aids are available for the rehabilitation of vestibular-schwannoma (VS)-related hearing loss. There is a lack of recently published papers regarding this theme. The aim of the present work is to organize current knowledge. (2) Methods: A review
[...] Read more.
(1) Background: Several types of hearing aids are available for the rehabilitation of vestibular-schwannoma (VS)-related hearing loss. There is a lack of recently published papers regarding this theme. The aim of the present work is to organize current knowledge. (2) Methods: A review of the literature regarding the topics “vestibular schwannoma”, “hearing loss”, and “hearing aid” was performed. Nineteen studies were thus considered. (3) Results: Conventional hearing aids, contralateral routing of signal (CROS) aids, bone anchored hearing aids (BAHA), and others are available options for hearing rehabilitation in VS patients. The speech discrimination score (SDS) is considered the best measure to assess candidacy for rehabilitation with hearing aids. The best hearing rehabilitative conditions in VS patients when using conventional hearing aid devices are a mild−moderate hearing loss degree with good word recognition (more than 50% SDS). CROS-Aid and BAHA are reported to be beneficial. CROS-Aid expands on the area of receiving hearing. BAHA aids use direct bone-conduction stimulation. Unfortunately, there are no available studies focused specifically on VS patients that compare CROS and BAHA technologies. (4) Conclusions: Hearing aids, CROS, and BAHA are viable options for rehabilitating hearing impairment in VS, but require an accurate case-by-case audiological evaluation for rehabilitating hearing impairment in VS. Further studies are needed to prove if what is currently known about similar hearing illnesses can be confirmed, particularly in the case of VS.
Full article
(This article belongs to the Special Issue Hearing and Balance in Acoustic Neuroma)
Open AccessArticle
Vestibular and Oculomotor Findings in Vestibular Migraine Patients
Audiol. Res. 2023, 13(4), 615-626; https://doi.org/10.3390/audiolres13040053 - 08 Aug 2023
Abstract
Background: Vestibular migraine (VM) is the most frequent etiology of recurrent spontaneous episodic vertigo. Vestibular and oculomotor abnormalities have been described in VM; however, the diagnosis is currently based on symptoms. The objective of this study was to determine the most frequent abnormalities
[...] Read more.
Background: Vestibular migraine (VM) is the most frequent etiology of recurrent spontaneous episodic vertigo. Vestibular and oculomotor abnormalities have been described in VM; however, the diagnosis is currently based on symptoms. The objective of this study was to determine the most frequent abnormalities in videonystagmography (VNG), caloric testing (Cal) and video head impulse test (vHIT) in patients with VM. Methods: A retrospective cohort study was conducted, including all VM and probable VM patients seen from January 2021 to July 2022. Demographics, auditory symptoms and results via VNG, Cal and vHIT were evaluated. VNG results were compared with a control group. Results: Sixty patients, 81.7% with VM and 18.3% with probable vestibular migraine, were included. VNG revealed the following abnormalities: 21.7% spontaneous nystagmus; 33.3% positional nystagmus, mostly central; 26.7% optokinetic nystagmus; 56.7% smooth pursuit abnormalities and 70% saccade test abnormalities, mostly velocity and latency. An abnormal unilateral caloric response was seen in 22.9%, while vHIT revealed a low gain in at least one canal in 21.7%, and saccades were seen in at least one canal with normal gains in 18.3%. Concordant results between Cal and lateral vHIT were seen in 77.1% of cases. Conclusions: Although VM is a clinical diagnosis, vestibular and oculomotor abnormalities are commonly seen. The most frequent oculomotor findings were an abnormal saccade test, abnormal smooth pursuit and central positional nystagmus.
Full article
(This article belongs to the Special Issue Episodic Vertigo: Differences, Overlappings, Opinion and Treatment)
►▼
Show Figures

Figure 1
Open AccessArticle
X-Linked Gusher Disease DFNX2 in Children, a Rare Inner Ear Dysplasia with Mixed Hearing and Vestibular Loss
by
, , , , and
Audiol. Res. 2023, 13(4), 600-614; https://doi.org/10.3390/audiolres13040052 - 04 Aug 2023
Abstract
Conductive hearing losses are typically present in disorders of the external/middle ear. However, there is a rare group of inner ear conditions called third windows that can also generate a conductive hearing loss. This is due to an abnormal connection between the middle
[...] Read more.
Conductive hearing losses are typically present in disorders of the external/middle ear. However, there is a rare group of inner ear conditions called third windows that can also generate a conductive hearing loss. This is due to an abnormal connection between the middle and the inner ear or between the inner ear and the cranial cavity. X-linked gusher disorder is an extremely rare congenital inner ear dysplastic syndrome with an abnormal connection due to a characteristic incomplete cochlear partition type III and an incomplete internal auditory meatus fundus. The disorder is inherited in an X-linked fashion due to the mutation of the POU3F4 gene. We present two siblings diagnosed with the condition and their long-term follow-ups. They both presented audiovestibular symptoms and showed progressive mixed losses and bilateral vestibular weakness. They were treated with cochlear implant, digital amplification and with vestibular rehabilitation. Significant others around them were involved in their journey with the medical team, and in both, a very favourable outcome was achieved. This is the first time that we have reported evolving audiovestibular function with vestibular quantification in X-linked gusher disorder and emphasize on the multidisciplinary holistic approach to manage these children effectively.
Full article
(This article belongs to the Special Issue Inner Ear Conductive Hearing Loss: Current Studies and Controversies)
►▼
Show Figures

Figure 1
Open AccessArticle
Contralateral Routing of Signal Disrupts Monaural Sound Localization
Audiol. Res. 2023, 13(4), 586-599; https://doi.org/10.3390/audiolres13040051 - 03 Aug 2023
Abstract
►▼
Show Figures
Objectives: In the absence of binaural hearing, individuals with single-sided deafness can adapt to use monaural level and spectral cues to improve their spatial hearing abilities. Contralateral routing of signal is the most common form of rehabilitation for individuals with single-sided deafness. However,
[...] Read more.
Objectives: In the absence of binaural hearing, individuals with single-sided deafness can adapt to use monaural level and spectral cues to improve their spatial hearing abilities. Contralateral routing of signal is the most common form of rehabilitation for individuals with single-sided deafness. However, little is known about how these devices affect monaural localization cues, which single-sided deafness listeners may become reliant on. This study aimed to investigate the effects of contralateral routing of signal hearing aids on localization performance in azimuth and elevation under monaural listening conditions. Design: Localization was assessed in 10 normal hearing adults under three listening conditions: (1) normal hearing (NH), (2) unilateral plug (NH-plug), and (3) unilateral plug and CROS aided (NH-plug + CROS). Monaural hearing simulation was achieved by plugging the ear with E-A-Rsoft™ FX™ foam earplugs. Stimuli consisted of 150 ms high-pass noise bursts (3–20 kHz), presented in a random order from fifty locations spanning ±70° in the horizontal and ±30° in the vertical plane at 45, 55, and 65 dBA. Results: In the unilateral plugged listening condition, participants demonstrated good localization in elevation and a response bias in azimuth for signals directed at the open ear. A significant decrease in performance in elevation occurs with the contralateral routing of signal hearing device on, evidenced by significant reductions in response gain and low r2 value. Additionally, performance in azimuth is further reduced for contralateral routing of signal aided localization compared to the simulated unilateral hearing loss condition. Use of the contralateral routing of signal device also results in a reduction in promptness of the listener response and an increase in response variability. Conclusions: Results suggest contralateral routing of signal hearing aids disrupt monaural spectral and level cues, which leads to detriments in localization performance in both the horizontal and vertical dimensions. Increased reaction time and increasing variability in responses suggests localization is more effortful when wearing the contralateral rerouting of signal device.
Full article

Figure 1
Open AccessArticle
Influence of Bone Conduction Hearing Device Implantation on Health-Related Quality of Life for Patients with and without Tinnitus
by
and
Audiol. Res. 2023, 13(4), 573-585; https://doi.org/10.3390/audiolres13040050 - 01 Aug 2023
Abstract
(1) Background: Tinnitus, often related to hearing loss, is an addressable public health concern affecting health-related quality of life (HRQoL). This study aimed to explore the influence of bone conduction hearing aid (BCHA) implantation on HRQoL and hearing disability in patients with hearing
[...] Read more.
(1) Background: Tinnitus, often related to hearing loss, is an addressable public health concern affecting health-related quality of life (HRQoL). This study aimed to explore the influence of bone conduction hearing aid (BCHA) implantation on HRQoL and hearing disability in patients with hearing loss suffering from tinnitus. (2) Methods: Data were collected from an international hearing implant registry. Health Utilities Index Mark 3 (HUI-3), Spatial and Qualities of Hearing- 49 Questionnaire (SSQ) and self-reported tinnitus burden data for adult patients implanted with a BCHA (n = 42) who provided baseline as well as follow-up data 1-year post-implantation were extracted from the registry. Wilcoxon signed rank tests and paired samples t-tests were used to analyse outcomes data. (3) Results: Patients, with or without tinnitus, demonstrated clinically important mean improvements in HUI-3 multi-attribute utility scores, HUI-3 hearing attribute and SSQ scores. Hearing loss patients with tinnitus presented with a lower HRQoL than patients without tinnitus. (4) Conclusions: These findings demonstrate the importance of hearing rehabilitation in improving the quality of life and hearing disability of patients with or without tinnitus and in providing tinnitus relief in some patients with hearing loss and tinnitus.
Full article
(This article belongs to the Topic Brain, Hearing and Tinnitus Science)
►▼
Show Figures
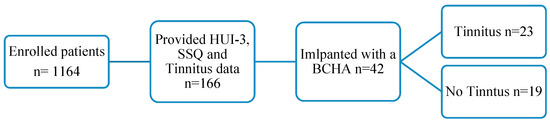
Figure 1
Open AccessArticle
Comparative Analysis of Cartilage Conduction Hearing Aid Users and Non-Users: An Investigative Study
by
, , , , , and
Audiol. Res. 2023, 13(4), 563-572; https://doi.org/10.3390/audiolres13040049 - 27 Jul 2023
Abstract
Clinical findings on cartilage conduction hearing aids (CCHAs) have gradually become clear; however, few reports include a large number of cases. This study included 91 ears from 69 patients who underwent CCHA fitting in our hospital. Their ears were divided into six groups
[...] Read more.
Clinical findings on cartilage conduction hearing aids (CCHAs) have gradually become clear; however, few reports include a large number of cases. This study included 91 ears from 69 patients who underwent CCHA fitting in our hospital. Their ears were divided into six groups (i.e., bilateral aural atresia or severe canal stenosis, unilateral aural atresia or severe canal stenosis, chronic otitis media or chronic otitis externa with otorrhea, sensorineural hearing loss, mixed hearing loss, and conductive hearing loss) according to their clinical diagnosis and type of hearing loss. Most clinical diagnoses were aural atresia or meatal stenosis (bilateral, 21.8%; unilateral, 39.6%). The purchase rate of CCHAs was higher in the closed-ear group (bilateral, 77.3%; unilateral, 62.5%). In the bilateral closed-ear group, air conduction thresholds at 1000, 2000, and 4000 Hz and aided thresholds with CCHAs at 4000 Hz were significantly lower in the purchase group than the non-purchase group. No significant difference was observed between the purchase and non-purchase groups in the unilateral closed-ear group. In the bilateral closed-ear group, air conduction thresholds and aided thresholds were associated with the purchase rate of CCHAs. In the unilateral closed-ear group, factors other than hearing might have affected the purchase rate of CCHAs.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction II)
►▼
Show Figures
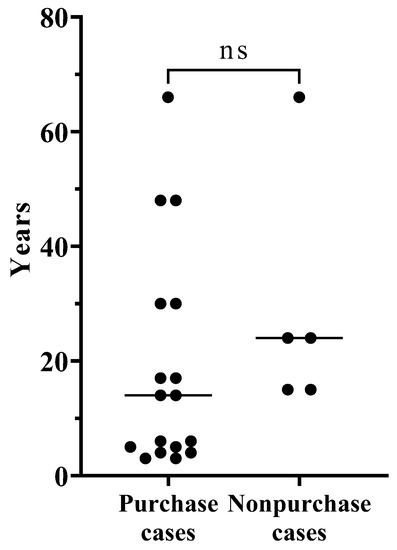
Figure 1
Open AccessArticle
Identifying Health-Related Conditions Associated with Tinnitus in Young Adults
by
, , , , , , , and
Audiol. Res. 2023, 13(4), 546-562; https://doi.org/10.3390/audiolres13040048 - 20 Jul 2023
Abstract
►▼
Show Figures
Objective: The present study investigated the epidemic of tinnitus in college-aged young adults. Our first objective was to identify health conditions associated with tinnitus in young adults. The second objective was to evaluate the predictive utility of some known risk factors. Study design:
[...] Read more.
Objective: The present study investigated the epidemic of tinnitus in college-aged young adults. Our first objective was to identify health conditions associated with tinnitus in young adults. The second objective was to evaluate the predictive utility of some known risk factors. Study design: A cross-sectional design was used to investigate the prevalence and risk factors for tinnitus. Setting: A questionnaire was distributed, reaching out to a large college-aged population. A total of 2258 young adults aged 18–30 years were recruited from April 2021 to February 2022. Interventions: A questionnaire was administered to investigate the epidemiology of tinnitus in a population of college-aged young adults. Results: About 17.7% of young adults reported bothersome tinnitus perception lasting for ≥5 min in the last 12 months. The prevalence of chronic tinnitus (bothersome tinnitus for ≥1 year) and acute tinnitus (bothersome tinnitus for <1 year) was 10.6% and 7.1%, respectively. About 19% of the study sample reported at least one health condition. Individuals reporting head injury, hypertension, heart disease, scarlet fever, and malaria showed significantly higher odds of reporting chronic tinnitus. Meningitis and self-reported hearing loss showed significant associations with bothersome tinnitus. The prevalence of chronic tinnitus was significantly higher in males reporting high noise exposure, a positive history of reoccurring ear infections, European ethnic background, and a positive health history. Risk modeling showed that noise exposure was the most important risk factor for chronic tinnitus, followed by sex, reoccurring ear infections, and a history of any health condition. A positive history of COVID-19 and self-reported severity showed no association with tinnitus. Individuals reporting reoccurring ear infections showed a significantly higher prevalence of COVID-19. Conclusions: While young adults with health conditions are at a higher risk of reporting tinnitus, the predictive utility of a positive health history remains relatively low, possibly due to weak associations between health conditions and tinnitus. Noise, male sex, reoccurring ear infections, European ethnicity, and a positive health history revealed higher odds of reporting chronic tinnitus than their counterparts. These risk factors collectively explained about 16% variability in chronic tinnitus, which highlights the need for identifying other risk factors for chronic tinnitus in young adults.
Full article

Figure 1
Open AccessReview
Management of Migraine-Associated Vestibulocochlear Disorders
Audiol. Res. 2023, 13(4), 528-545; https://doi.org/10.3390/audiolres13040047 - 19 Jul 2023
Abstract
Migraine is a chronic neurological disorder that frequently coexists with different vestibular and cochlear symptoms (sudden hearing loss, tinnitus, otalgia, aural fullness, hyperacusis, dizziness, imbalance, and vertigo) and disorders (recurrent benign positional vertigo, persistent postural perceptual dizziness, mal de debarquement, and Menière’s disease).
[...] Read more.
Migraine is a chronic neurological disorder that frequently coexists with different vestibular and cochlear symptoms (sudden hearing loss, tinnitus, otalgia, aural fullness, hyperacusis, dizziness, imbalance, and vertigo) and disorders (recurrent benign positional vertigo, persistent postural perceptual dizziness, mal de debarquement, and Menière’s disease). Despite evidence of an epidemiological association and similar pathophysiology between migraine and these vestibulocochlear disorders, patients suffering from migraine-related symptoms are usually underdiagnosed and undertreated. Current migraine treatment options have shown success in treating vestibulocochlear symptoms. Lifestyle and dietary modifications (reducing stress, restful sleep, avoiding migraine dietary triggers, and avoiding starvation and dehydration) and supplements (vitamin B2 and magnesium) offer effective first-line treatments. Treatment with migraine prophylactic medications such as tricyclic antidepressants (e.g., nortriptyline), anticonvulsants (e.g., topiramate), and calcium channel blockers (e.g., verapamil) is implemented when lifestyle and dietary modifications are not sufficient in improving a patient’s symptoms. We have included an algorithm that outlines a suggested approach for addressing these symptoms, taking into account our clinical observations. Greater recognition and understanding of migraine and its related vestibular and cochlear symptoms are needed to ensure the appropriate diagnosis and treatment of affected patients.
Full article
(This article belongs to the Special Issue Auditory Disorders: Incidence, Intervention and Treatment)
►▼
Show Figures
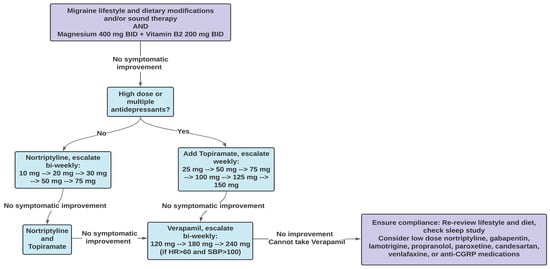
Figure 1
Open AccessArticle
Association between Third Mobile Window Disorders and Symptom Reduction Using a Noise Cancelling Device: Inverse Tullio Phenomena
Audiol. Res. 2023, 13(4), 516-527; https://doi.org/10.3390/audiolres13040046 - 17 Jul 2023
Abstract
Identifying a vestibular source of pathology in patients complaining of post-traumatic brain injury (TBI) dizziness can be difficult. We describe a possible new method utilizing a reduction in post-TBI symptoms (including dizziness) with the use of a noise cancellation device (NCD). This retrospective
[...] Read more.
Identifying a vestibular source of pathology in patients complaining of post-traumatic brain injury (TBI) dizziness can be difficult. We describe a possible new method utilizing a reduction in post-TBI symptoms (including dizziness) with the use of a noise cancellation device (NCD). This retrospective case series included patients with TBI and dizziness presenting to a binocular vision specialty clinic, who were diagnosed with a vertical heterophoria (VH). If they did not respond adequately to microprism lenses and/or if they experienced hyperacusis, they were evaluated with an NCD. If there was marked reduction in TBI symptoms (including dizziness), the patients were referred to a neuro-otologist for vestibular diagnostic evaluation and treatment. Fourteen patients were identified and found to have abnormalities on vestibular testing consistent with third mobile window disorder (TMWD). All were treated with a 6-week medical protocol (diuretics, no straining, low sodium/no caffeine diet). Five responded positively, requiring no further treatment. Nine required surgical intervention and responded positively. In conclusion, in 14 patients with post-concussive dizziness and VH, a positive response to NCD was associated with abnormal vestibular testing, a diagnosis of TMWD, and symptom reduction/resolution with a medical or surgical approach. The removal of sound resulting in reduction or resolution of vestibular symptoms represents an inverse Tullio phenomenon.
Full article
(This article belongs to the Special Issue Inner Ear Conductive Hearing Loss: Current Studies and Controversies)
►▼
Show Figures

Figure 1
Open AccessReview
Cartilage Conduction Hearing Aids in Clinical Practice
Audiol. Res. 2023, 13(4), 506-515; https://doi.org/10.3390/audiolres13040045 - 13 Jul 2023
Abstract
A relatively loud sound is audible when a vibrator is attached to the aural cartilage. This form of conduction is referred to as cartilage conduction (CC). In Japan, a new type of hearing aid has been developed using CC and has been available
[...] Read more.
A relatively loud sound is audible when a vibrator is attached to the aural cartilage. This form of conduction is referred to as cartilage conduction (CC). In Japan, a new type of hearing aid has been developed using CC and has been available in clinical practice since 2017. A clinical study conducted prior to its launch demonstrated its benefits, particularly in patients with aural atresia who were unable to use air conduction hearing aids. Several studies have been published on the benefits of CC hearing aids since their introduction into clinical practice. Most of the patients included in these studies had canal stenosis or aural atresia, and the purchase rates of CC hearing aids in these patients were relatively high. However, the number of patients with canal-open ears was small, with overall poor results in the trials, with the exception of patients with continuous otorrhea. CC hearing aids are considered a good option for compensating for hearing loss in ears with canal stenosis or atresia in both bilateral and unilateral cases. However, CC hearing aids are not currently considered the first choice for patients with a canal-open ear.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction II)
►▼
Show Figures
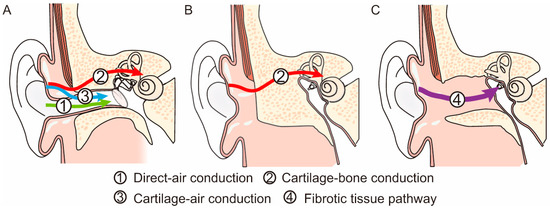
Figure 1
Open AccessArticle
In Vivo Measurement of Ear Ossicle and Bony Wall Vibration by Sound Stimulation of Cartilage Conduction
by
, , , , and
Audiol. Res. 2023, 13(4), 495-505; https://doi.org/10.3390/audiolres13040044 - 12 Jul 2023
Abstract
The cartilage-conduction pathway was recently proposed as a third auditory pathway; however, middle-ear vibrations have not yet been investigated in vivo. We aimed to measure the ossicles and bone vibration upon cartilage-conduction stimulation with a non-contact laser Doppler vibrometer. We recruited adult patients
[...] Read more.
The cartilage-conduction pathway was recently proposed as a third auditory pathway; however, middle-ear vibrations have not yet been investigated in vivo. We aimed to measure the ossicles and bone vibration upon cartilage-conduction stimulation with a non-contact laser Doppler vibrometer. We recruited adult patients with normal ear structures who underwent cochlear implant surgery at our hospital between April 2020 and December 2022. For sound input, a cartilage-conduction transducer, custom-made by RION Corporation (Tokyo, Japan), was fixed to the surface of the tragus and connected to an audiometer to regulate the output. A posterior tympanotomy was performed and a laser beam was directed through the cavity to measure the vibration of the ossicles, cochlear promontory, and posterior wall of the external auditory canal. Five participants (three men, mean age: 56.4 years) were included. The mean hearing loss on the operative side was 96.3 dB HL in one patient, and that of the other patients was off-scale. The vibrations were measured at a sound input of 1 kHz and 60 dB. We observed vibrations of all three structures, demonstrating the existence of cartilage-conduction pathways in vivo. These results may help uncover the mechanisms of the cartilage-conduction pathway in the future.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction II)
►▼
Show Figures

Figure 1
Open AccessArticle
The Effect of Alpha-Lipoic Acid in the Treatment of Chronic Subjective Tinnitus through the Tinnitus Handicap Inventory Scores
by
, , , , , , , and
Audiol. Res. 2023, 13(4), 484-494; https://doi.org/10.3390/audiolres13040043 - 07 Jul 2023
Abstract
►▼
Show Figures
Background and Objectives: Tinnitus affects millions of adults. Many therapies, including complementary and alternative medicine and tinnitus retraining therapies, have been trialed, but an effective option, particularly for chronic subjective tinnitus (CTS), is still lacking. Materials and Methods: This study investigated the effects
[...] Read more.
Background and Objectives: Tinnitus affects millions of adults. Many therapies, including complementary and alternative medicine and tinnitus retraining therapies, have been trialed, but an effective option, particularly for chronic subjective tinnitus (CTS), is still lacking. Materials and Methods: This study investigated the effects of alpha-lipoic acid (600 mg. per day for two months) on two groups of patients using a questionnaire. One group (A) was affected by tinnitus associated with likely cochlear dysfunction and metabolic syndrome, and the other (B) was composed of subjects with acoustic nerve lesions. All the patients were asked to complete the Italian version of the tinnitus handicap inventory (THI) to determine the overall degree of perceived annoyance at the beginning and end of therapy. Pure tone averages for speech frequencies and for high frequencies were computed, and psychoacoustic pitch and loudness matches were determined for each subject before and after treatment. Results: The pure tone audiometry, pitch, loudness, and THI scores of both groups were reported. In group A, statistically significant differences were observed for the “functional” and “emotional” subscales. The total score of THI and the loudness of tinnitus were also significantly reduced. No statistically significant differences were observed in group B. Conclusions: These findings suggest a possible contribution of the antioxidant effect to the organ of Corti in subjects with metabolic syndrome and CST.
Full article

Figure 1
Open AccessReview
Prognostic Factors for Hearing Preservation Surgery in Small Vestibular Schwannoma
Audiol. Res. 2023, 13(4), 473-483; https://doi.org/10.3390/audiolres13040042 - 03 Jul 2023
Abstract
Objective: to evaluate recent contributions to the literature on prognostic factors of hearing preservation in small vestibular schwannoma microsurgery. Methods: review of the most recent studies. Results: factors such as tumor size, preoperative hearing status, tumor growth rate, tumor origin, surgical approach, radiological
[...] Read more.
Objective: to evaluate recent contributions to the literature on prognostic factors of hearing preservation in small vestibular schwannoma microsurgery. Methods: review of the most recent studies. Results: factors such as tumor size, preoperative hearing status, tumor growth rate, tumor origin, surgical approach, radiological characteristics, results of preoperative neurophysiological tests, preoperative symptoms and demographic features have been investigated and some of them reported to be significant in the prediction of hearing preservation. Conclusions: tumor size and preoperative hearing status are the most impactful factors and play a key role in patient selection for hearing preservation surgery. Other features such as fundal extension, tumor origin and impaired ABR could have prognostic value on hearing preservation. Tumor growth rate, preoperative impedance, cVEMPs and age have also recently been found to be significant, but more studies are needed. The role of preoperative tinnitus, vertigo and gender is lacking and controversial, whereas the differences between available surgical approaches have been smoothed out in recent years.
Full article
(This article belongs to the Special Issue Hearing and Balance in Acoustic Neuroma)
Open AccessBrief Report
Similarities and Differences between Vestibular Migraine and Recurrent Vestibular Symptoms—Not Otherwise Specified (RVS-NOS)
Audiol. Res. 2023, 13(3), 466-472; https://doi.org/10.3390/audiolres13030041 - 08 Jun 2023
Abstract
Menière’s disease and vestibular migraine (VM) are two common inner ear disorders whose diagnoses are based on clinical history and audiometric exams. In some cases, patients have been reporting different episodes of vertigo for years but not fulfilling the Bárány Society criteria for
[...] Read more.
Menière’s disease and vestibular migraine (VM) are two common inner ear disorders whose diagnoses are based on clinical history and audiometric exams. In some cases, patients have been reporting different episodes of vertigo for years but not fulfilling the Bárány Society criteria for either. These are called Recurrent Vestibular Symptoms—Not Otherwise Specified (RVS-NOS). It is still under debate if this is a single disease entity or a part of the spectrum of already established disorders. The purpose of our work was to establish similarities and differences with VM in terms of clinical history, bedside examination, and family history. We enrolled 28 patients with RVS-NOS who were followed for at least 3 years with stable diagnosis; results were compared with those of 34 subjects having a diagnosis of definite VM. The age of onset of vertigo was lower in VM than in RVS-NOS (31.2 vs. 38.4 years). As for the duration of attacks and symptoms, we detected no differences other than subjects with RVS-NOS reporting milder attacks. Cochlear accompanying symptoms were more frequently reported by VM subjects (one subject reporting tinnitus and another one reported tinnitus and fullness). Motion sickness was equally reported by subjects across two samples (around 50% for both). Bipositional long-lasting, non-paroxysmal nystagmus was the most common finding in the two groups, with no significant difference. Finally, the percentage of familial cases of migrainous headache and episodic vertigo did not differ between the two samples. In conclusion, RVS-NOS shares some common aspects with VM, including the temporal profile of attacks, motion sickness (commonly considered a migraine precursor), bedside examination, and family history. Our results are not inconsistent with the possibility that RVS-NOS may be a heterogeneous disorder, even if some of these subjects may share common pathophysiological mechanisms with VM.
Full article
(This article belongs to the Special Issue Episodic Vertigo: Differences, Overlappings, Opinion and Treatment)
Open AccessCase Report
Using a Bone Conduction Hearing Device as a Tactile Aid
by
, , , , and
Audiol. Res. 2023, 13(3), 459-465; https://doi.org/10.3390/audiolres13030040 - 07 Jun 2023
Abstract
Background: With the advent of cochlear implants, tactile aids for the profoundly deaf became obsolete decades ago. Nevertheless, they might still be useful in rare cases. We report the case of a 25-year-old woman with Bosley–Salih–Alorainy Syndrome and bilateral cochlear aplasia. Methods: After
[...] Read more.
Background: With the advent of cochlear implants, tactile aids for the profoundly deaf became obsolete decades ago. Nevertheless, they might still be useful in rare cases. We report the case of a 25-year-old woman with Bosley–Salih–Alorainy Syndrome and bilateral cochlear aplasia. Methods: After it was determined that cochlear or brainstem implants were not an option and tactile aids were not available anymore, a bone conduction device (BCD) on a softband was tried as a tactile aid. The usual retroauricular position and a second position close to the wrist, preferred by the patient, were compared. Sound detection thresholds were measured with and without the aid. Additionally, three bilaterally deaf adult cochlear implant users were tested under the same conditions. Results: At 250–1000 Hz, sounds were perceived as vibrations above approximately 45–60 dB with the device at the wrist. Thresholds were approximately 10 dB poorer when placed retroauricularly. Differentiation between different sounds seemed difficult. Nevertheless, the patient uses the device and can perceive loud sounds. Conclusions: Cases where the use of tactile aids may make sense are probably very rare. The use of BCD, placed, e.g., at the wrist, may be useful, but sound perception is limited to low frequencies and relatively loud levels.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction II)
►▼
Show Figures
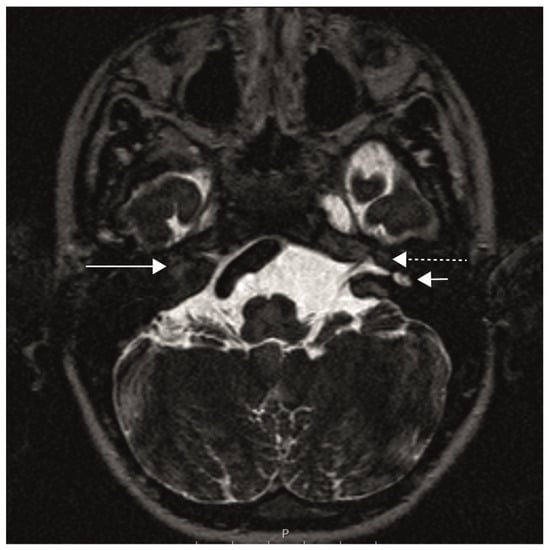
Figure 1
Open AccessArticle
Universal Recommendations on Planning and Performing the Auditory Brainstem Responses (ABR) with a Focus on Mice and Rats
Audiol. Res. 2023, 13(3), 441-458; https://doi.org/10.3390/audiolres13030039 - 02 Jun 2023
Abstract
Translational audiology research aims to transfer basic research findings into practical clinical applications. While animal studies provide essential knowledge for translational research, there is an urgent need to improve the reproducibility of data derived from these studies. Sources of variability in animal research
[...] Read more.
Translational audiology research aims to transfer basic research findings into practical clinical applications. While animal studies provide essential knowledge for translational research, there is an urgent need to improve the reproducibility of data derived from these studies. Sources of variability in animal research can be grouped into three areas: animal, equipment, and experimental. To increase standardization in animal research, we developed universal recommendations for designing and conducting studies using a standard audiological method: auditory brainstem response (ABR). The recommendations are domain-specific and are intended to guide the reader through the issues that are important when applying for ABR approval, preparing for, and conducting ABR experiments. Better experimental standardization, which is the goal of these guidelines, is expected to improve the understanding and interpretation of results, reduce the number of animals used in preclinical studies, and improve the translation of knowledge to the clinic.
Full article
(This article belongs to the Special Issue Translational Research in Audiology)
►▼
Show Figures
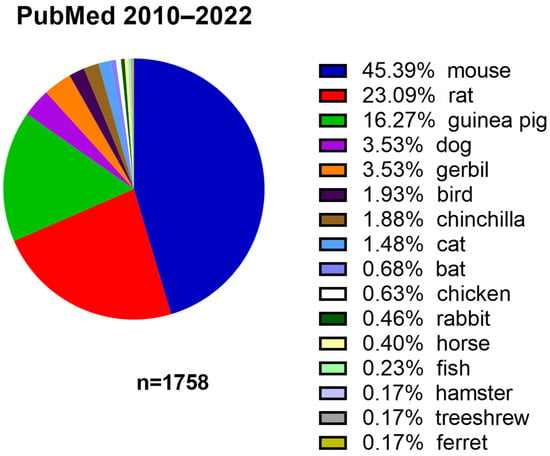
Figure 1
Open AccessArticle
Hearing Outcomes Following Endolymphatic Duct Blockage Surgery and Factors Associated with Improved Audition at Two Years Follow-Up
by
and
Audiol. Res. 2023, 13(3), 431-440; https://doi.org/10.3390/audiolres13030038 - 02 Jun 2023
Abstract
Objective: To evaluate hearing outcomes at 2 years post endolymphatic duct blockage (EDB) surgery, with an analysis of factors that may predict hearing improvement. Study Design: Retrospective comparative study. Setting: Tertiary care center. Subjects: Definite Ménière’s Disease (MD) patients undergoing EDB for refractory
[...] Read more.
Objective: To evaluate hearing outcomes at 2 years post endolymphatic duct blockage (EDB) surgery, with an analysis of factors that may predict hearing improvement. Study Design: Retrospective comparative study. Setting: Tertiary care center. Subjects: Definite Ménière’s Disease (MD) patients undergoing EDB for refractory disease. Methods: Chart review was conducted to assign cases to one of the three hearing outcome groups (deteriorated, stable, and improved). All cases that met our inclusion criteria were selected. Preoperative data collected were audiograms, bithermal caloric tests, preoperative vertigo episodes, history of previous ear surgery for Ménière, intratympanic steroid injections (ITS) and intraoperative endolymphatic sac (ELS) tear or opening. Postoperative data collected at 24 months were audiograms, vertigo episodes and bithermal caloric testing. Results: Preoperative vertigo episodes, caloric paresis and history of surgery, ITS injections or ELS integrity, as well as postoperative vertigo class distribution and caloric paresis changes were not different between our groups. Preoperative word recognition score (WRS) was lowest in the improved hearing group (p = 0.032). The persistence of tinnitus at 2 years postoperatively was associated with deteriorated hearing (p = 0.033). Conclusions: There are no strong predictors of hearing improvement on presentation pre-EDB, but low preoperative WRS may be the best estimator available. Therefore, ablative interventions should be considered very carefully in patients presenting with low WRS, as they may benefit more from EDB; there is a fair chance of a good hearing outcome with EDB surgery. Persistence of tinnitus can reflect deteriorating audition. Vertigo control and hearing preservation are independent outcomes of EDB surgery, making it desirable as an early intervention for refractory MD cases.
Full article
(This article belongs to the Special Issue Inner Ear Conductive Hearing Loss: Current Studies and Controversies)
►▼
Show Figures
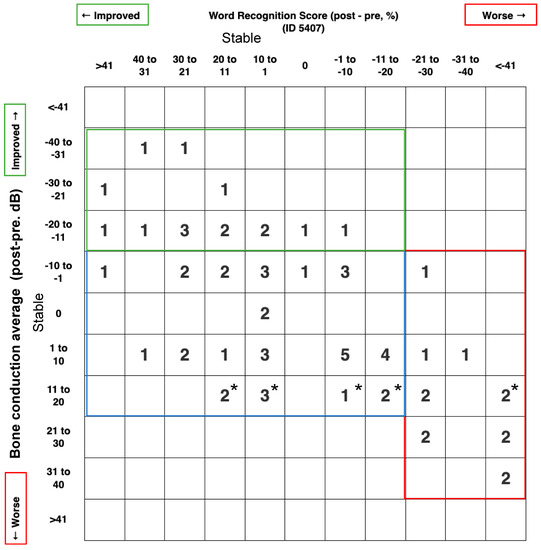
Figure 1
Open AccessFeature PaperReview
A Review of Neural Data and Modelling to Explain How a Semicircular Canal Dehiscence (SCD) Causes Enhanced VEMPs, Skull Vibration Induced Nystagmus (SVIN), and the Tullio Phenomenon
Audiol. Res. 2023, 13(3), 418-430; https://doi.org/10.3390/audiolres13030037 - 02 Jun 2023
Abstract
Angular acceleration stimulation of a semicircular canal causes an increased firing rate in primary canal afferent neurons that result in nystagmus in healthy adult animals. However, increased firing rate in canal afferent neurons can also be caused by sound or vibration in patients
[...] Read more.
Angular acceleration stimulation of a semicircular canal causes an increased firing rate in primary canal afferent neurons that result in nystagmus in healthy adult animals. However, increased firing rate in canal afferent neurons can also be caused by sound or vibration in patients after a semicircular canal dehiscence, and so these unusual stimuli will also cause nystagmus. The recent data and model by Iversen and Rabbitt show that sound or vibration may increase firing rate either by neural activation locked to the individual cycles of the stimulus or by slow changes in firing rate due to fluid pumping (“acoustic streaming”), which causes cupula deflection. Both mechanisms will act to increase the primary afferent firing rate and so trigger nystagmus. The primary afferent data in guinea pigs indicate that in some situations, these two mechanisms may oppose each other. This review has shown how these three clinical phenomena—skull vibration-induced nystagmus, enhanced vestibular evoked myogenic potentials, and the Tullio phenomenon—have a common tie: they are caused by the new response of semicircular canal afferent neurons to sound and vibration after a semicircular canal dehiscence.
Full article
(This article belongs to the Special Issue Third Mobile Window Syndromes: New Insights in Pathomechanisms, Instrumental Diagnosis and Surgical Treatment)
►▼
Show Figures
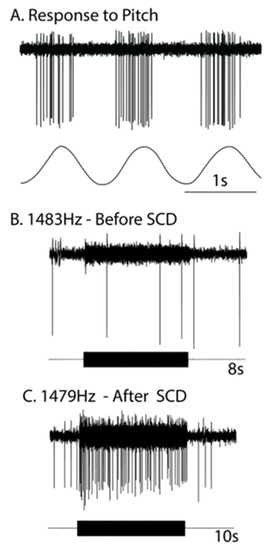
Figure 1
Open AccessArticle
The Effects of Utilizing Cartilage Conduction Hearing Aids among Patients with Conductive Hearing Loss
by
, , , , , , and
Audiol. Res. 2023, 13(3), 408-417; https://doi.org/10.3390/audiolres13030036 - 01 Jun 2023
Abstract
The cartilage-conduction hearing aid (CC-HA) is a new hearing device that is suitable for use in patients with conductive hearing loss. It has been 5 years since the introduction of the CC-HA. Although the number of users has increased, the CC-HA is not
[...] Read more.
The cartilage-conduction hearing aid (CC-HA) is a new hearing device that is suitable for use in patients with conductive hearing loss. It has been 5 years since the introduction of the CC-HA. Although the number of users has increased, the CC-HA is not yet widely known. This study examines the effects of CC-HA on patients with conductive hearing loss and investigates factors that affect the willingness to use the device by comparing purchasers and non-purchasers of CC-HA in patients with unilateral conductive hearing loss. Eight patients had bilateral conductive hearing loss, and 35 had unilateral conductive hearing loss. Each patient underwent sound field tests and speech audiometry, and the effects of the CC-HA were compared with those of conventional bone conduction hearing aids (BC-HA). In patients with bilateral conductive hearing loss, the CC-HA was non-inferior to BC-HA. The CC-HA improved the hearing thresholds and speech recognition in patients with unilateral conductive hearing loss. Moreover, in patients with unilateral conductive hearing loss, experiencing the effect of wearing the CC-HA under conditions such as putting noise in the better ear could affect patients’ willingness to use the CC-HA.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction II)
►▼
Show Figures
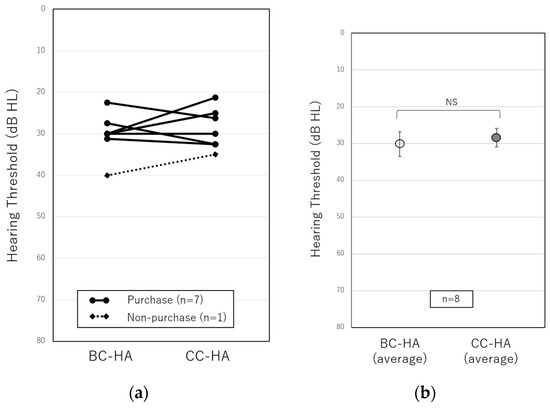
Figure 1
Open AccessReview
Intraoperative Cochlear Nerve Monitoring in Cochlear Implantation after Vestibular Schwannoma Resection
Audiol. Res. 2023, 13(3), 398-407; https://doi.org/10.3390/audiolres13030035 - 30 May 2023
Abstract
Background: The use of a cochlear implant (CI) for hearing rehabilitation after vestibular schwannoma (VS) resection is widely spreading. The procedure is usually performed simultaneously to tumor resection with a translabyrinthine approach. To ensure the best device function, assessing the integrity of the
[...] Read more.
Background: The use of a cochlear implant (CI) for hearing rehabilitation after vestibular schwannoma (VS) resection is widely spreading. The procedure is usually performed simultaneously to tumor resection with a translabyrinthine approach. To ensure the best device function, assessing the integrity of the cochlear nerve is of primary importance. Methods: A narrative review of the literature on the present topic was carried out up to June 2022. Finally, nine studies were considered. Results: Electrically evoked auditory brainstem responses (eABR) is the most widely used method of intraoperative monitoring of cochlear nerve (CN) during VS resection, although its limits are known. It can be assessed through the CI electrode array or through an intracochlear test electrode (ITE). Variations of the graph are evaluated during the surgical procedure, in particular the wave V amplitude and latency. As tumor dissection progresses, the parameters may change, informing of the CN status, and the surgical procedure may be modulated. Conclusion: An eABR positive result seems to be reliably correlated with a good CI outcome in those cases in which a clear wave V is recorded before and after tumor removal. On the contrary, in those cases in which the eABR is lost or altered during the surgical procedure, the positioning of a CI is still debatable.
Full article
(This article belongs to the Special Issue Hearing and Balance in Acoustic Neuroma)

Journal Menu
► ▼ Journal Menu-
- Audiology Research Home
- Aims & Scope
- Editorial Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Topical Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Society Collaborations
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Audiology Research
Auditory Disorders: Incidence, Intervention and Treatment
Guest Editors: Adrien Eshraghi, Rahul MittalDeadline: 15 August 2023
Special Issue in
Audiology Research
Hearing Impairment: Neurocognitive Consequences and Brain Plasticity
Guest Editors: Yang Zhang, Seiji Nakagawa, Gavin M Bidelman, Anu Sharma, Chieh KaoDeadline: 31 August 2023
Special Issue in
Audiology Research
Audio-Vestibular Disorders in the COVID-19 Pandemics
Guest Editors: Andrea Ciorba, Stavros HatzopoulosDeadline: 30 September 2023
Special Issue in
Audiology Research
Cognitive Decline within the Audiology Scope of Practice
Guest Editor: Jennifer ListerDeadline: 15 October 2023
Topical Collections
Topical Collection in
Audiology Research
Cochlear Implants: Challenges and Opportunities in Hearing Rehabilitation
Collection Editors: Andrea Ciorba, Daniele Borsetto
Topical Collection in
Audiology Research
Translational Audiology
Collection Editor: Agnieszka Szczepek







